Going to BAT for Obesity Solutions?
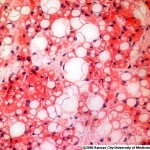 Last week saw an almost complete edition of the New England Journal of Medicine devoted to obesity – the key finding: brown adipose tissue (BAT) is alive and well in adults and in some people may contribute significantly to resting metabolic rate.
Last week saw an almost complete edition of the New England Journal of Medicine devoted to obesity – the key finding: brown adipose tissue (BAT) is alive and well in adults and in some people may contribute significantly to resting metabolic rate.
Without going into details on the findings (as these have been widely described in numerous media articles and TV reports) here is what’s new:
Although the discussion has been going on for a long time, these articles now provide conclusive evidence that BAT is indeed present in adults – women have more than men.
The presence of BAT is negatively correlated with BMI – the higher the BMI, the lesser the BAT. This suggests that having BAT may protect from weight gain (are these the folks, who can eat all they want without gaining a pound?).
BAT is stimulated by exposure to cold – not entirely unexpected. I can’t wait to see how this concept is embraced by the weight loss industry and public media.
BAT is less present in older individuals – again, not unexpected, given that expression of BAT is linked to sympathetic nervous activity, which tends to decrease with age.
Obviously, lots of interesting questions:
Can pharmacological stimulation of BAT promote weight loss – remember, this was already tried unsuccessfully with beta 3-agonists. They stimulated BAT but were poorly tolerated and never made it to market.
Can BAT imaging help identify folks at risk for weight gain – certainly not with current technology (PET-CTs), which would be prohibitively expensive.
Is turning down the ambient temperature an effective solution to preventing obesity – my guess is not.
Great science – unfortunately, no quick fix for the obesity epidemic.
AMS
Edmonton, Alberta
Mitochondria and Obesity Revisited
 Several months ago I blogged about the results from a Finnish twin study that found lower mitochondria numbers and disturbed mitochondrial energy metabolism activity in fat cells from identical twins who were leaner than their genetically identical co-twins. These impairments correlated with critical clinical measures of obesity including liver fat accumulation, reduced whole-body insulin sensitivity, hyperinsulinemia, hypoadiponectinemia and adipocyte hypertrophy.
Several months ago I blogged about the results from a Finnish twin study that found lower mitochondria numbers and disturbed mitochondrial energy metabolism activity in fat cells from identical twins who were leaner than their genetically identical co-twins. These impairments correlated with critical clinical measures of obesity including liver fat accumulation, reduced whole-body insulin sensitivity, hyperinsulinemia, hypoadiponectinemia and adipocyte hypertrophy.
In this month’s issue of OBESITY, Tomas Gianotti and colleagues from the University of Buenos Aires, Argentina, report a significantly lower mitochondrial-to-nuclear DNA ratio (mtDNA/nDNA) in insulin resistant (IR) adolescents recruited out of a subset (n=175) of a cross-sectional, population-based study of 934 high school students. In this study, the mtDNA/nDNA ratio was also inversely correlated with HOMA index, a crude but simple measure of insulin resistance.
This study is very much in line with the notion that obesity-prone individuals may have impaired mitochondrial number and/or function resulting in increased risk for obesity.
From the aforementioned twin study, we know that the decreased number and function is not corrected by weight loss.
Indeed the question is whether or not mitochondrial number and function can be increased by prescribing higher activity levels? If yes, how much activity will be needed to reverse these changes? And most importantly, will people with impaired mitochondrial function actually be able to enjoy exercise enough to actually stick with this prescription?
Perhaps it is not obesity that causes impaired mitochondrial function but rather impaired mitochondrial number and/or function that predisposes to obesity. This impairment could be genetic but also due to intrauterine programing or perhaps simply luck of the draw (remember – all mtDNA comes from your mom).
Of course this is not an “excuse” for obesity as is often misinterpreted when data on the genetics and biology are presented. However, it is clear that if you have impaired mitochondrial number and/or function you are much more likely to become obese in an environment that promotes sedentariness than if you were dependent on physical activity to meet your basic needs for survival.
Remember, there were times, not too long ago, when people were actually paid to be physically active. Today, choosing to be physically active actually costs money (not to mention time).
AMS
Edmonton, Alberta
Obesities and What to do About Them
Over the last couple of days I have been reading a new 160 page report on “Tackling Obesities: Future Choices” produced by the UK Government’s Foresight Program which is run under the Government Office for Science.
The report was prepared by some 200 experts (mostly from the UK) and ends with several “what if” scenarios that model the outcomes of possible policy decisions.
The first point of note is that the title of the work refers to “Obesities” rather than “Obesity”, thereby formally recognizing that this is a heterogeneous entity and that there are many forms of obesity.
Over all the work is impressive and discusses obesities in all their complexities – the biological and environmental system map is enough to let anyone serious about trying to understand the causes of the epidemic throw up their hands in despair and flee the room.
Nevertheless, the work is useful in that it contains a lot of interesting bits that are “quotable” and deserve discussion.
Sentences like:
“The forces that drive obesity are, for many people, overwhelming.”
are notable because they depart from the usual idea that obesity is essentially a consequences of individuals’ choices and decisions and all anyone has to do is to be “smarter” about their health.
This obviously we know is not true – in fact, if, as stated elsewhere in the report,
“People [in the UK] today don’t have less willpower and are not more gluttonous than previous generations.”
and
“…for an increasing number of people, weight gain is the inevitable – and largely involuntary – consequence of exposure to a modern lifestyle.”
we need to be careful not to blame the victims.
It will rather be changes in social values and the way society as a whole chooses to respond to this epidemic that will make a difference. Amongst the experts, there was clearly no expectation of any spontaneous reversal of obesity trends.
The report is a challenging but fun read. I will probably be posting more on stuff I find in it over the next few weeks.
For those wanting to read the full report, you can download it by clicking here.
AMS


