Do Changes in Leptin, Ghrelin or Insulin Predict Weight Regain?
 One of the main reasons why keeping weight off, is because of the complex neuroendocrine response to weight loss, which serve to promote weight regain.
One of the main reasons why keeping weight off, is because of the complex neuroendocrine response to weight loss, which serve to promote weight regain.
While some of the players involved in these responses are known, whether or not measuring them would help predict who may have a harder time losing weight or who is more likely to regain weight is not.
As paper by Stohacker and colleagues from Brown University, Rhode Island, USA, published in the International Journal of Obesity suggests that this may be more complicated than some may think.
In their review of 12 studies reporting changes in leptin, ghrelin or insulin during intentional weight loss with a follow-up period to assess regain, no consistent relationship was found between any of these factors and weight regain.
Indeed, if anything, the data on this issue is more than confusing.
For e.g. as the authors note,
“…two of the nine studies examining leptin suggested that larger decreases were associated with great regain, three studies found the opposite (smaller decreases were associated with regain) while four studies found no significant relationship”.
Similarly,
“One study suggested that improvements in insulin resistance were associated with weight gain, but five subsequent studies reported no association.”
Thus, the notion that simply measuring some of the hormones associated with weight loss is unlikely to predict weight regain in a given individual.
This should come as no surprise.
Not only, are these only three of a whole array of possible biological mediators of weight regain but, as the authors point out, there may also be important behavioural and environmental (and I would add psychological and medical) reasons why some people may find it easier to sustain weight loss than others. And of course, genetic factors as well as past weight-loss history may also play a role in this.
Overall, there does not appear to be any simple test that clinicians can use to predict who is likely to regain weight and who is not.
On the other hand, given that the vast majority of people who lose weight ultimately put it back on (perhaps with the exception of those undergoing bariatric surgery – but even there regain may happen), this question may not be the most pressing – after all, spotting weight regain when it happens is not rocket science.
@DrSharma
Edmonton, AB
![]() Strohacker K, McCaffery JM, Maclean PS, & Wing RR (2013). Adaptations of leptin, ghrelin or insulin during weight loss as predictors of weight regain: a review of current literature. International journal of obesity (2005) PMID: 23801147
Strohacker K, McCaffery JM, Maclean PS, & Wing RR (2013). Adaptations of leptin, ghrelin or insulin during weight loss as predictors of weight regain: a review of current literature. International journal of obesity (2005) PMID: 23801147
.
Hindsight: PPARg and Adipose Tissue
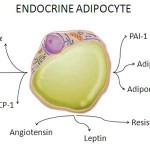 Back in 2006 there was a tremendous interest in the biology of peroxisome proliferator-activated receptor gamma (PPARg).
Back in 2006 there was a tremendous interest in the biology of peroxisome proliferator-activated receptor gamma (PPARg).
Not only had this nuclear hormone receptor been well recognised as a key regulator of adipocyte differentiation, but the introduction of thiazolidinediones (“glitazones”) in diabetes treatment sparked a tremendous amount of work in this ligand.
In a paper I co-athored with my French colleague Bart Staels, published in the Journal of Clinical Endocrinology and Metabolism in 2006, we reviewed the literature on the role of PPARg in regulating lipid and glucose metabolism in adipose tissue.
Our review included all articles we could find on the role of PPARg in adipose tissue of healthy individuals and those with obesity, metabolic syndrome, or type 2 diabetes published between 1990 and 2006.
As we discuss in detail in the article, PPARg is highly expressed in adipose tissue, where its activation with thiazolidinediones alters fat topography and adipocyte phenotype and up-regulates genes involved in fatty acid metabolism and triglyceride storage.
In addition, PPARg activation is associated with potentially beneficial effects on the expression and secretion of a range of factors, including adiponectin, resistin, IL-6, TNFalpha, plasminogen activator inhibitor-1, monocyte chemoattractant protein-1, and angiotensinogen, as well as a reduction in plasma nonesterified fatty acid supply.
This effects of PPARg-agonists also extends to macrophages, where they suppress production of inflammatory mediators.
Thus, we speculated that PPARg-activating ligands may have a role in preventing progression of insulin resistance to diabetes and endothelial dysfunction to atherosclerosis.
Since then the optimism about this class of medications has been tempered by the fact that larger clinical trials have raised concerns particularly about cardiovascular complications in patients with heart failure.
At the time, however, this state-of-the-art review received considerable attention with over 230 citations to date.
AMS
Edmonton, Alberta
Hindsight: Bound Leptin and Sympathetic Activity
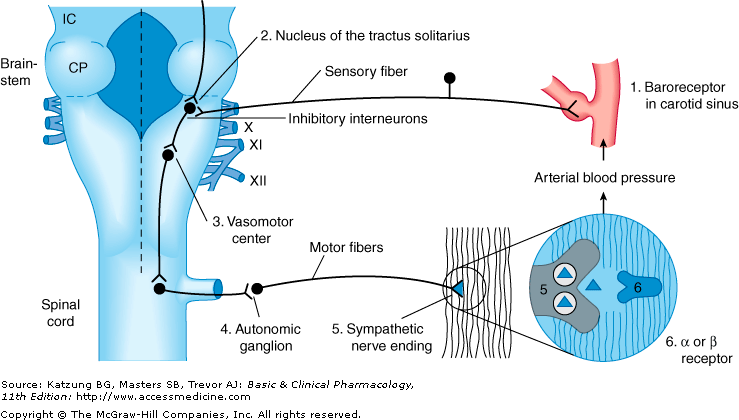 As readers are probably well aware, leptin is one of the key hormones (secreted by fat cells), that regulate energy balance – not just by affecting food intake but also energy output. The latter happens in part through stimulation of the sympathetic nervous system.
As readers are probably well aware, leptin is one of the key hormones (secreted by fat cells), that regulate energy balance – not just by affecting food intake but also energy output. The latter happens in part through stimulation of the sympathetic nervous system.
In a paper we published in the Journal of Clinical Endocrinology and Metabolism in 2003, we examined the relationship between both free and protein-bound plasma leptin levels and sympathetic activity as assessed by microneurography.
Study participants included 25 healthy normal weight men, 8 individuals with central (multiple system atrophy) and 4 individuals with peripheral (pure) autonomic failure. Baroreflex sensitivity was measured using phenylephrine and nitroprusside infusions.
MSNA was consistently correlated with protein-bound leptin concentrations but not with free leptin levels. MSNA at baseline was about 15 bursts per minute in subjects with lower and about 24 bursts per minute in subjects with higher bound leptin concentrations.
We concluded that protein-bound rather than free leptin levels are correlated with basal sympathetic outflow, a relationship that was difficult to explain through a direct central nervous effect of protein-bound leptin. Rather, we suggested that protein-bound leptin may increase sympathetic vasomotor tone indirectly via a baroreflex mechanism.
According to Google Scholar, this paper has been cited 26 times.
AMS
Edmonton, Alberta
Obesity and Mental Health – Beyond Pharmacotherapy
 Continuing my posts on the recent articles on obesity and mental health published in the January issue of the Canadian Journal of Psychiatry, I now turn my attention to a paper by Valerie Taylor and colleagues on the many links between mental health issues and obesity.
Continuing my posts on the recent articles on obesity and mental health published in the January issue of the Canadian Journal of Psychiatry, I now turn my attention to a paper by Valerie Taylor and colleagues on the many links between mental health issues and obesity.
Whilst in the previous post I have focussed on the relationship between psychiatric medications and weight gain, a problem that is common knowledge to the mental health community, this article highlights many of the lesser known links between mental health problems and excess weight. These include interesting neurobiological, psychological, and sociological factors, that are now increasingly understood.
For e.g.
“‘Atypical’ depression, a type of major depressive disorder characterized by an increase in the need for sleep and food, may actually characterize the most ‘typical’ presentation of major depression For the majority of people with depression, therefore, a diagnosis of major depression is synonymous with a phenotype that increases vulnerability towards weight problems.”
In fact,
“The neurobiology of depression [also] confers increased risk of obesity. The most common biological perturbation associated with depression is an increase in cortisol. This increase, and the hypothalamic pituitary adrenal axis abnormalities that accompany it, is similar to changes seen in Cushing syndrome, an endocrinological illness caused by an increase in cortisol that is characterized phenotypically by excessive visceral weight gain. While levels of cortisol found in major depression disorders are much lower than that of Cushings, the biological impact of excess cortisol is similar; a predisposition towards increased deposition of centrally located adipose tissue.”
In addition mood disorders often affect sleeping behaviour, which in turn affects important regulators of appetite and metabolism like ghrelin, leptin, adiponectin, and other hormones. Moreover, chronic inflammation may play a role in both major depression and obesity.
In the case of schizophrenia, primary negative symptoms like amotivation, which can be observed even in the earliest stages of the illness, may lead to reduced physical capacity and altered self-perception. Hypodopaminergic activity may in part explain increased propensity for substance use, especially cannabis, which can promote hyperphagia.
There is an increasingly recognized association between obesity and attention deficit disorder, and it may well be that impulsivity may play an important role in overeating.
Also,
“Poor planning and an inability to delay reward, processes largely mediated by the pre-frontal cortex, may lead individuals with ADHD to over-consume highly palatable, fattening foods. A related hypothesis is that individuals with low intrinsic dopamine activity in brain areas mediating reward may attempt to compensate by using various reinforcing behaviors including increased food consumption. This has been termed the “reward deficiency syndrome” and has been described separately in ADHD and in obesity suggesting that ADHD and obesity may thus reflect different manifestations of a single biological change related to low dopamine activity in prefrontal attentional areas and brain reward pathways.”
The paper also discussed findings showing that ADHD is associated with more media consumption, less participation in physical activity and organized sports.
Finally, the paper examines the literature on the relationship between obesity and childhood adverse events like sexual, mental, physical abuse and emotional neglect, which can have important impacts on the hypothalamic-pituitary-adrenal axis as well as on sex hormones that may promote fat accumulation.
“The use of food as a coping strategy or a “self-soothing behavior” is seen in both trauma patients and in those with mood disorders, and it may be related to the use of food to modulate neurotransmitters involved in affect control. Most work in this area has focused on serotonin and dopamine, both of which play a critical role in both eating behavior and mood regulation. It may be that the ability of certain foods to temporarily boost mood can create a behavioral cycle where food is consumed to control feelings of sadness.”
As readers of these posts may be well aware,
“The relationship between trauma and weight is especially evident during weight loss treatment programs and in bariatric surgery programs, a past history of trauma can be a harbinger of post-operative problems. Food and weight gain in response to abuse may be related to a desire to become “bigger” to be able to defend against an abuser, it may have been a way to change appearance when an individual inaccurately felt they were somehow provoking the abuse or it may have become a surrogate comfort mechanism when appropriate supports failed.”
Thus, clinicians (and patients) must be aware of the complex relationship between obesity and mental health issues that go well beyond just the issue of weight gain with psychiatric medications (which of course further compound these issues).
All the more reason, why all health professionals called upon to manage obesity should be well versed in recognizing and helping patients address mental health problems.
AMS
Edmonton, Alberta
Hindsight: 1st International Symposium on Obesity and Hypertension, October 28–30, 1999, Berlin, Germany
Continuing in my series of past publications on obesity, today’s post is special, because it is about an event that ‘officially’ launched my shift from hypertension into obesity research and for the first time made some of the leading obesity researchers of the time aware of my very existence.
Back in 1998, I had already well-established myself in the hypertension field, being widely recognized as an expert on salt-sensitive hypertension. I was already being invited to speak at various hypertension meetings around the world and was nationally and internationally recognized for this work.
However, it would be fair to say that despite having published a few minor papers on obesity, no one in the obesity arena had ever heard of me. This was by no means surprising as, having attended a few obesity conferences by then, it was evident that few hypertension researchers interacted with obesity researchers and vice versa. Apparently, no one had yet thought of bringing the two research communities together – surprising perhaps, given the fact that obesity is the most common and powerful risk factor for hypertension.
So, perhaps for the first time demonstrating my potential talent as a ‘networker’, I decided to organize the 1st International Symposium on Obesity and Hypertension (ISOH), to which I rather cheekily ventured to invite some of the most distinguished researchers from the obesity field – cheeky, because these folks had certainly never heard of me and I was not offering any honoraria or expensive airplane tickets. I just looked for big names in obesity on the internet and sent out the invitations.
Little would I have imagined that I would assemble a roster of cutting edge ‘big names’ from both the hypertension and obesity communities for a tightly packed two day event in Berlin.
To my lay readers, the names may mean nothing, but to my professional colleagues, the following list probably reads like a ‘who-is-who’ of obesity.
W. P. T. James (Chairman, International Obesity Task Force, Aberdeen, UK) presented new data suggesting that obesity-associated comorbidity may increase rapidly in non-Caucasians with a body mass index as low as 18 kg/m2.
M. E. J. Lean (Department of Human Nutrition, University of Glasgow, UK) presented new data indicating that waist circumference (measured midway between the lowest rib and the iliac crest) is the best clinical marker of intraabdominal fat accumulation and that risks are high enough to warrant professional guidance with a waist over 102 cm in men or 88 cm in women.
R. Negrel (Centre de Biochimie, UMR6543CNRS & IFR349, Faculty of Sciences, Nice, France) and G. Löffler (University of Regensburg, Institute of Biochemistry, Regensburg, Germany), who provided convincing evidence on the presence of the renin-angiotensin system in adipose tissue.
D. L. Crandall (Wyeth Ayerst Research, Radnor, PA, USA) presented a comprehensive review, inncluding historical review of the classical experiments that identified early hemodynamic changes observed in obesity and the important role of neovascularization for the growth and development of adipose tissue.
H. Hauner (Diabetes Research Institute at the University of Düsseldorf, Germany) stressed the point that stromal cells from adipose tissue can undergo differentiation in the presence of defined adipogenic factors, including a variety of hormones and cytokines.
T. Unger (Institute for Pharmacology, Christian-Albrechts University of Kiel, Germany) presented evidence that the AT1 and AT2 angiotensin receptors may play an important role in the growth and development of a variety of tissues, including cardiac, endothelial, and neuronal cells.
F. C. Luft (Franz Volhard Clinic and Max Delbrück Center, Humboldt University of Berlin, Germany) presented the results of linkage analysis in an Arab pedigree with familial hypercholesterolemia in which heterozygous persons with normal LDL levels were identified.
T. W. Kurtz (University of California, San Francisco, CA, USA) and M. Pravenec (Czech Academy of Sciences, Prague, Czech Republic) presented data indicating that a Cd36 Mutation in some strains of spontaneously hypertensive rat may be associated with insulin resistance in these strains.
X. Jeunemaitre (INSERM U36, College de France, Paris, France) provided new evidence indicating that several polymorphisms located in the 5’ region and in the first intron of the angiotensinogen gene may contribute to the variability of plasma angiotensinogen levels.
M. L. Tuck (Veterans Administration Medical Center, Sepulveda, CA, USA) presented an up-to-date review on the role of the systemic renin-angiotensin system in obesity-related hypertension.
A. Natali (Department of Internal Medicine, University of Pisa, Italy) discussed the role of insulin resistance in obesity-related hypertension and provided data that suggesting that the sympatho-adrenergic system plays an important role in the development of obesity hypertension.
W. G. Haynes (Department of Internal Medicine, University of Iowa, Iowa City, USA), who discussed the important role of leptinergic and melanocortin influences on the sympathetic nervous system in obesity-related hypertension.
G. Seravalle (Clinica Medica, University of Milan, Italy) studied the effects of the acute blockade of corticotropin-releasing hormone (CRH) secretion induced by dexamethasone (DEX) on the sympathoexcitatory response elicited by insulin.
A. D. Strosberg (Institut Cochin de Génétique Molèculaire, Paris, France) discussed the potential role of beta-3 adrenergic receptors in the development of obesity.
S. L. H. Schiffelers (NUTRIM, Department of Human Biology, Maastricht University, Maastricht, The Netherlands) on the effects of beta 1- and beta 2-adrenoreceptors–stimulated thermogenesis and fat oxidation in lean and obese men.
S. Rössner (Huddinge University Hospital, Sweden) presented the first clinical data on a new lipase inhibitor orlistat which reduces the absorption of dietary fat by 30% and reduces weight and blood pressure.
R. Donelly (University of Nottingham, Division of Cardiovascular Medicine, Nottingham, UK) reviewed the pharmacological treatment of obesity-related hypertension.
P. G. Kopelman (St. Bartholomew’s Hospital and The Royal London School of Medicine, University of London, UK) provided an outlook of the management problems that will become apparent in the early part of the 21st century.
With this roster of leading experts, it was perhaps not surprising that we attracted over 150 attendees from over 30 countries to his ‘impromptu’ meeting.
It turns out that this was to be only the first of a total of four ISOH meetings, the last held in 2005, by which time I had not only made a name for myself in obesity (having been appointed to a Tier 1 Canada Research Chair in Cardiovascular Obesity Research and Management at McMaster University in 2002), but had also managed to build professional and personal relationships around the world that last to this day.
I also learnt important lessons that formed the very basis for eventually creating the Canadian Obesity Network, now with almost 7,000 members, by far the largest national professional obesity association in the world.
For those, who would like to read more about the symposium, the proceedings were published in Kidney and Blood Pressure Research in 2000.
For anyone who may have attended the event (or any of the subsequent ISOH meetings), I’d love to hear about your recollections of these Symposia.
AMS
Edmonton, Canada
![]() Sharma AM, Distler A, & Hauner H (2000). International symposium on obesity and hypertension genetics and molecular mechanisms. Genetics and molecular mechanisms Kidney & blood pressure research, 23 (1), 49-72 PMID: 10567854
Sharma AM, Distler A, & Hauner H (2000). International symposium on obesity and hypertension genetics and molecular mechanisms. Genetics and molecular mechanisms Kidney & blood pressure research, 23 (1), 49-72 PMID: 10567854
.



