Obesity and Mental Health – Beyond Pharmacotherapy
Wednesday, February 1, 2012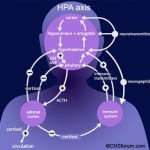 Continuing my posts on the recent articles on obesity and mental health published in the January issue of the Canadian Journal of Psychiatry, I now turn my attention to a paper by Valerie Taylor and colleagues on the many links between mental health issues and obesity.
Continuing my posts on the recent articles on obesity and mental health published in the January issue of the Canadian Journal of Psychiatry, I now turn my attention to a paper by Valerie Taylor and colleagues on the many links between mental health issues and obesity.
Whilst in the previous post I have focussed on the relationship between psychiatric medications and weight gain, a problem that is common knowledge to the mental health community, this article highlights many of the lesser known links between mental health problems and excess weight. These include interesting neurobiological, psychological, and sociological factors, that are now increasingly understood.
For e.g.
“‘Atypical’ depression, a type of major depressive disorder characterized by an increase in the need for sleep and food, may actually characterize the most ‘typical’ presentation of major depression For the majority of people with depression, therefore, a diagnosis of major depression is synonymous with a phenotype that increases vulnerability towards weight problems.”
In fact,
“The neurobiology of depression [also] confers increased risk of obesity. The most common biological perturbation associated with depression is an increase in cortisol. This increase, and the hypothalamic pituitary adrenal axis abnormalities that accompany it, is similar to changes seen in Cushing syndrome, an endocrinological illness caused by an increase in cortisol that is characterized phenotypically by excessive visceral weight gain. While levels of cortisol found in major depression disorders are much lower than that of Cushings, the biological impact of excess cortisol is similar; a predisposition towards increased deposition of centrally located adipose tissue.”
In addition mood disorders often affect sleeping behaviour, which in turn affects important regulators of appetite and metabolism like ghrelin, leptin, adiponectin, and other hormones. Moreover, chronic inflammation may play a role in both major depression and obesity.
In the case of schizophrenia, primary negative symptoms like amotivation, which can be observed even in the earliest stages of the illness, may lead to reduced physical capacity and altered self-perception. Hypodopaminergic activity may in part explain increased propensity for substance use, especially cannabis, which can promote hyperphagia.
There is an increasingly recognized association between obesity and attention deficit disorder, and it may well be that impulsivity may play an important role in overeating.
Also,
“Poor planning and an inability to delay reward, processes largely mediated by the pre-frontal cortex, may lead individuals with ADHD to over-consume highly palatable, fattening foods. A related hypothesis is that individuals with low intrinsic dopamine activity in brain areas mediating reward may attempt to compensate by using various reinforcing behaviors including increased food consumption. This has been termed the “reward deficiency syndrome” and has been described separately in ADHD and in obesity suggesting that ADHD and obesity may thus reflect different manifestations of a single biological change related to low dopamine activity in prefrontal attentional areas and brain reward pathways.”
The paper also discussed findings showing that ADHD is associated with more media consumption, less participation in physical activity and organized sports.
Finally, the paper examines the literature on the relationship between obesity and childhood adverse events like sexual, mental, physical abuse and emotional neglect, which can have important impacts on the hypothalamic-pituitary-adrenal axis as well as on sex hormones that may promote fat accumulation.
“The use of food as a coping strategy or a “self-soothing behavior” is seen in both trauma patients and in those with mood disorders, and it may be related to the use of food to modulate neurotransmitters involved in affect control. Most work in this area has focused on serotonin and dopamine, both of which play a critical role in both eating behavior and mood regulation. It may be that the ability of certain foods to temporarily boost mood can create a behavioral cycle where food is consumed to control feelings of sadness.”
As readers of these posts may be well aware,
“The relationship between trauma and weight is especially evident during weight loss treatment programs and in bariatric surgery programs, a past history of trauma can be a harbinger of post-operative problems. Food and weight gain in response to abuse may be related to a desire to become “bigger” to be able to defend against an abuser, it may have been a way to change appearance when an individual inaccurately felt they were somehow provoking the abuse or it may have become a surrogate comfort mechanism when appropriate supports failed.”
Thus, clinicians (and patients) must be aware of the complex relationship between obesity and mental health issues that go well beyond just the issue of weight gain with psychiatric medications (which of course further compound these issues).
All the more reason, why all health professionals called upon to manage obesity should be well versed in recognizing and helping patients address mental health problems.
AMS
Edmonton, Alberta


