Diagnosis and Treatment of Obstructive Sleep Apnea in Adults
 In follow up to yesterday’s guest post by Christy Turer on her challenges in getting timely diagnostics and treatment for a patient with severe obstructive sleep apnea (OSA), it appears timely that this week’s issue of the Canadian Medical Association Journal (CMAJ) features a full-length update on the diagnosis and treatment of OSA in adults.
In follow up to yesterday’s guest post by Christy Turer on her challenges in getting timely diagnostics and treatment for a patient with severe obstructive sleep apnea (OSA), it appears timely that this week’s issue of the Canadian Medical Association Journal (CMAJ) features a full-length update on the diagnosis and treatment of OSA in adults.
As Cheryl Laratta form the University of British Columbia and colleagues point out, OSA) is likely underdiagnosed in Canada with lack of appropriate treatment putting many at risk of poor quality of life, comorbidity, motor vehicle crashes and increased health care utilization.
Clinical features include daytime sleepiness, unrefreshing sleep or fatigue, frequent nocturnal waking due to choking or gasping, nocturia, morning headaches, poor concentration, irritability and erectile dysfunction. Bed partners may report snoring or witnessed apneas. Atypical symptoms, more frequently reported by women, include insomnia, impaired memory, mood disturbance, reflux and nocturnal enuresis.
However, as the authors point out, the correlation of symptoms with disease severity is poor, which is why it is important for physicians to be alert to milder symptoms and screen individuals who present with known risk factors like overweight/obesity, increased neck circumference and nasopharangeal crowding. Importantly, while the presence of these features increases pre-test probability, neither history nor physical examination are enough to rule out OSA.
A number of questionnaires (e.g. Berlin Questionnaire, STOP-Bang, etc.) are available to assist in screening patients.
As for diagnosis,
“The gold standard for diagnosis of OSA is attended polysomnography (level I study), which involves collection of seven or more data channels, including electroencephalogram and electrooculogram for sleep staging, electromyogram, electrocardiogram and respiratory channels.”
Less reliably,
“Level III sleep studies record a minimum of three channels of data while the patient sleeps at home. Level III studies usually monitor airflow, snoring, respiratory excursion, body position, heart rate and oxygen saturation, but some validated devices use surrogate measurements for these variables, such as tonometry or actigraphy, and the technology is constantly evolving.51 Level III studies do not record sleep; therefore, severity of OSA is estimated using the respiratory event index, which is the number of desaturation events per hour of total recording time.”
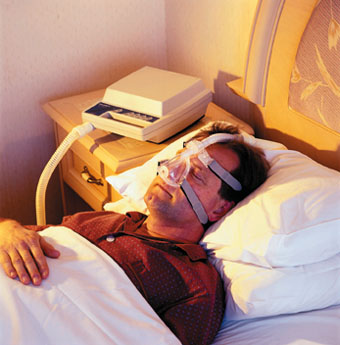
Treatment options include nightly use of a continuous positive airway pressure (CPAP) device or the use of oral devices (for less severe cases). The latter should be custom fitted by a dentist with extensive experience or additional training in dental sleep medicine.
Oddly enough, there is no mention of obesity treatment as an effective measure to manage OSA, given that there is evidence from both medical and surgical obesity treatment studies that document clinically important improvement in OSA with weight loss.
The article also briefly discusses on-going long-term patient management as well as some of the important research issues that remain to be studied regarding the rather complex pathophysiology of this common disorder.
In addition,
“Research into the models of service delivery for OSA, including strategies to improve timely access to care, funding for OSA treatment and patient preference, will be important to improve the care of Canadians with sleep disordered breathing.”
@DrSharma
Edmonton, AB
Urgent Need For Low-Cost In-Home Diagnostics For Obstructive Sleep Apnea

Christy Turer, MD, Assistant Professor of Pediatrics, Internal Medicine, and Clinical Sciences at University of Texas Southwestern (UTSW) Medical Center, Dallas, Texas, USA
Today’s guest post comes from Christy Turer, MD, Assistant Professor of Pediatrics, Internal Medicine, and Clinical Sciences at University of Texas Southwestern (UTSW) Medical Center, Dallas, Texas, USA.
This week, I saw a 50 year-old female patient with obesity (BMI 44) who desperately needs screening and treatment for obstructive sleep apnea (OSA).
Over the past four years, her heart function (ejection fraction) has declined from >60% to now ~20% with significant pulmonary hypertension, almost certainly related to undiagnosed, untreated OSA based on multiple nightly witnessed apneas.
Although she now sleeps with oxygen, this does nothing for her hypopnea-related, sympathetic overdrive-mediated, cardiac dysfunction.
Without CPAP treatment, her life expectancy is two years or less.
Unfortunately, within the public health system for which I work (county system that offers free or discounted healthcare to poor residents in a metropolitan city, USA), the average wait time for a sleep study is 1-2 years.
To be fair, this patient has had a previous attempt at a sleep study in a sleep lab a couple of years ago. At that time, however, the study was inconclusive, because she could not fall asleep in the sleep lab’s unfamiliar environment.
It is frustrating not being able to help my patients with suspected sleep apnea, especially, when I know that help could be available.
It is high time we had a technological disruption that enables cheap, reliable, in-home OSA assessment for patients.
Christy Turer, MD
Dallas, TX
Dr Turer is a standing member of the US Food and Drug Administration’s Pediatric Advisory Committee, a consultant to the FDA’s Endocrinologic/Metabolic Drugs Advisory Committee, and Past-Chair of the Obesity Society’s Clinical Management of Obesity Section. She has authored numerous scientific articles and lectured widely on primary-care evaluation and management of overweight/obesity and related metabolic comorbidities across the lifespan. Her comments do not reflect the views of UTSW, FDA, or any of her funding sources.


