Weighty Problems in Oversized Young Athletes?
 Over the next little while, I will be taking a few days off and so I will be reposting some of my favourite past posts. The following article was first posted on Dec 2, 2009:
Over the next little while, I will be taking a few days off and so I will be reposting some of my favourite past posts. The following article was first posted on Dec 2, 2009:
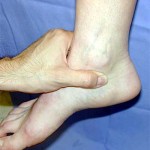
According to a paper by Malachy McHugh from the Nicholas Institute of Sports Medicine and Athletic Trauma, Lenox Hill Hospital, US, published in the latest issue of the British Journal of Sports Medicine, overweight and obese adolescents are more than twice as likely to be injured in sports and other physical activities compared with non-overweight and non-obese adolescents. Moreover, obese adolescent athletes are more than three times as likely to sustain an ankle sprain compared with normal weight adolescent athletes.
The increased risk of injury associated with being overweight or obese may in part be due to low physical activity levels and therefore promotion of physical activity for children can provide neuromuscular training that may be beneficial in decreasing injury risk associated with general play and sports. In addition, specific neuromuscular training interventions, such as balance training, may also help reduce the risk of injury associated with overweight and obesity.
Importantly, injured overweight young athletes tend to have more prolonged recovery periods than non-overweight young athletes.
According to McHugh, early aggressive treatment of swelling with physical modalities, prolonged non-weight bearing, limited period of immobilization, and regular repetitive passive joint motion are all indicated for the overweight young athlete with a lower extremity joint injury.
AMS
Frankfurt, Germany
Obesity Increases Risk For Occupational Injury?
 Earlier this week, I posted on the increased risk for severe ultra-low-velocity knee injuries associated with severe obesity.
Earlier this week, I posted on the increased risk for severe ultra-low-velocity knee injuries associated with severe obesity.
A study by Ian Janssen and colleagues from Queen’s University, Kingston, Ontario, published in the Journal of Obesity, examines the relationship between occupational injury and obesity in the canadian workforce.
These authors have previously described a biophysical framework on the possible determinants of increased risk in obese individuals:
“… obesity is associated with (1) a number of risk factors for unintentional injury (increased comorbidities, increased use of psychotropic medications, altered gait and balance, increased forces involved in falls, lower neural sensitivity, greater extremity friction, and sleep apnea and fatigue) as well as (2) some protective factors that will help prevent injury (greater bone density and increased cushioning during falls from excess fat).”
In their analysis of data in a representative longitudinal sample of 7,678 adult Canadian workers obese workers were about 40% more likely to report any occupational injuries and almost 50% more likely to report serious occupational injuries than normal-weight workers.
These relationships were more pronounced for sprains and strains (80% higher risk), injuries to the lower limbs (2-fold higher risk) or torso (almost 2.5-fold higher risk), and injuries due to falls (2-fold) or overexertion (2-fold).
Female workers, workers ≥40 years, and workers employed in sedentary occupations were particularly vulnerable.
Importantly, while this association was found for obese individuals, risk for overweight workers was not increased.
Nevertheless, regarding population attributable risk (PAR), the authors point out that:
“If the relationships under study are accurate and causal in nature, the PAR estimates indicate that approximately one in ten occupational injury events in the Canadian workforce are directly attributable to obesity, with up to one in five occupational injuries being attributable to obesity in susceptible population subgroups.”
Thus, the authors have the following suggestions for employers:
“…employers should consider how obesity impacts and interacts with other salient and modifiable risk factors for workplace injury such as job and task design, physical environments, and social factors. For example, workstations can be designed to be ergonomically sound for heavier persons and not just the average person.
In addition:
“…employers should consider adopting or expanding workplace wellness initiatives aimed at improving physical activity and eating behaviours in their workforce.”
The authors also note that:
“Although the medical services associated with workplace injury in Canada are covered by our public health care system and not the employer or its insurance provider, employers need to recognize that investments into workplace wellness initiatives could still have a favourable impact on the bottom line by reducing absenteeism and lost productivity.”
Is your workplace ‘safe’ for obese employees? How can it be made safer?
All suggestions are appreciated.
AMS
Duchesnay, Quebec
Janssen I, Bacon E, & Pickett W (2011). Obesity and its relationship with occupational injury in the canadian workforce. Journal of obesity, 2011 PMID: 21773008
Weight Increases Recovery Time From Injuries in Kids
 Seems like this is injury week on these pages.
Seems like this is injury week on these pages.
After blogging about injury patterns in obese US high-school athletes on Monday, today’s article is some Canadian data just published by Warsh and colleagues from Queen’s University, Kingston, Ontario, in the International Journal of Injury Control and Safety Promotion, looking at whether overweight and obese kids take longer to recover from injury.
The data source was the 2002 Canadian Health Behaviour in School-Aged Children (HBSC) survey, which included 7266 youth in grades 6 through 10 sampled from all Canadian provinces and territories. Of these, 2831 students reported an injury event and were included in the analysis.
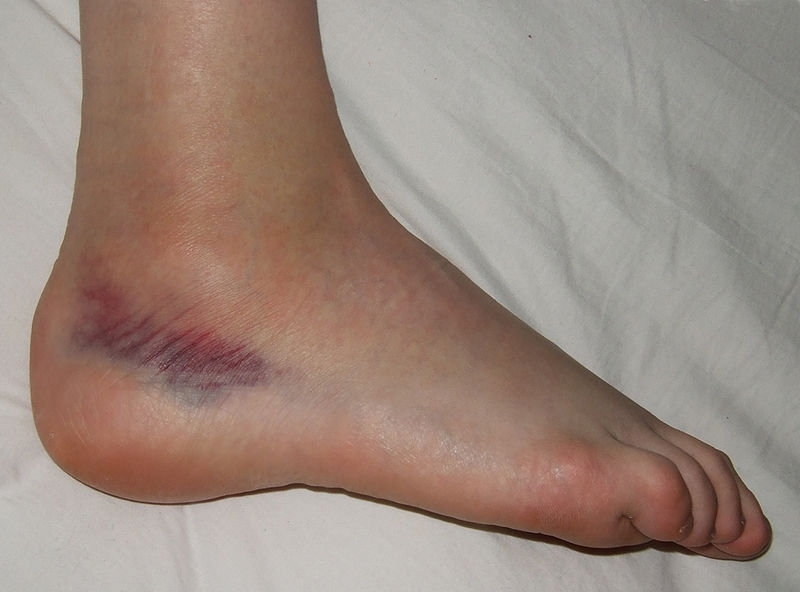
Youth who were obese and suffered a combined injury (broken bone and strain/sprain) took significantly longer to recover compared to normal weight youth but the recovery time for uncomplicated injuries (fractures or strains alone) was not significantly higher.
Clinicians providing an injury recovery prognosis may need to take into account BMI status and allow for extra recovery time for heavier patients in this age range.
AMS
Heidelberg, Germany
Warsh J, Janssen I, & Pickett W (2011). Do overweight and obese youth take longer to recover from injury? International journal of injury control and safety promotion, 1-7 PMID: 21424972
Injury Patterns in Overweight and Obese High School Athletes
 In case readers are wondering whether the term “obese athlete” is an oxymoron, it is not: from my own practice I know that there are a number of high-performance athletes out there, who can have significant weight-related health problems including obstructive sleep apnea, hypertension and fatty liver disease. But that is NOT the topic of this post!
In case readers are wondering whether the term “obese athlete” is an oxymoron, it is not: from my own practice I know that there are a number of high-performance athletes out there, who can have significant weight-related health problems including obstructive sleep apnea, hypertension and fatty liver disease. But that is NOT the topic of this post!
This post is about the findings of Ellen Yard and Dawn Comstock from the Centre for Injury Research and Policy, Columbus, Ohio, just published in the Journal of Physical Activity and Health, regarding the the relationship between injury pattern and BMI in US high school athletes.
This question is of considerable interest, as the authors note that about one-third of the over 7 million US high school athletes meet the BMI criteria for overweight or obesity.
The researchers analysed data from 100 nationally representative US high schools, which submitted athlete exposure (AE) and injury information during the 2005 to 08 school years via High School RIO (Reporting Information Online).
A total of 13,881 injuries during 5,627,921 athlete-exposures (2.47 injuries per 1000 AE) were reported, representing an estimated 4,339,247 injuries sustained nationally during the 2005–08 school years, for an average of 1,446,416 injuries sustained annually.
Injury rates were higher in competition (4.65 per 1000 AE) compared with practice (1.65 per 1000 AE).
Injury rates were highest in football (4.32 per 1000 AE), wrestling (2.43 per 1000 AE) and girls’ soccer (2.40 per 1000 AE). Injury rates were lowest in baseball (1.13 per 1000 AE), softball (1.19 per 1000 AE), and volleyball (1.39 per 1000 AE).
Two-thirds (61.4%) of these injuries occurred in normal weight athletes, with the exception of football, where 54% of injured athletes were overweight or obese. Specifically, in football, the majority of injured defensive tackles (65.2%), offensive tackles (64.7%), centers (63.1%), and offensive guards (58.4%) were obese.
Sport-specific overweight and obesity prevalence was also high in wrestling (31.7%), baseball (28.6%), and boys’ basketball (19.3%). Conversely, injured girls’ soccer athletes were least likely to be overweight or obese (13.5%). Other sport-specific positions with large proportions of obese athletes included first basemen in baseball (20.5%) and softball (17.2%).
The most common injury diagnoses were incomplete ligament sprains (28.2%), incomplete muscle strains (14.0%), contusions (13.2%), fractures (9.8%), and concussions (9.2%), with one in twenty (5.9%) injured athletes requiring surgery.
Compared with normal weight athletes, obese athletes sustained a larger proportion of knee injuries and their injuries were more likely to have resulted from contact with another person.
Interestingly, compared with normal weight athletes, underweight athletes sustained a larger proportion of fractures and a larger proportion of injuries resulting from ‘illegal’ activity.
With regard to the high prevalence of obesity amongst football players, the authors note:
“Although the use of BMI instead of body fat percentage may have classified some very muscular football players as overweight or obese, these findings are consistent with the previously reported epidemic of overweight and obesity in football. Football culture not only accepts but often encourages large body size, particularly among offensive and defensive linemen.“
These results point to important differences in the pattern of injuries incurred by heavier compared to normal or underweight athletes – some of which may be accounted for by the propensities of heavier athletes to participate in different types of sports than their leaner counterparts.
While this study does not support the notion that higher BMI athletes are at greater risk for injury (reported in previous studies), it may point to an increased risk in underweight athletes:
“With high school athletes being bigger and faster today than in previous years, collisions between mismatched athletes may be putting smaller, underweight athletes at greater risk for severe injury.”
What the paper does not discuss is the long-term risk of athletics for future weight gain, in overweight and obese athletes who retire due to injury or other life events. As blogged before, there seems to be no shortage of patients in my adult bariatric clinic, who report having been competitive athletes in younger years.
AMS
Edmonton, Alberta
Yard E, & Comstock D (2011). Injury Patterns by Body Mass Index in US High School Athletes. Journal of physical activity & health, 8 (2), 182-91 PMID: 21415445
Is Obesity a Risk Factor for Tendinopathy?
 Without question, people carrying extra weight are at high risk for mechanical injury to their musculoskeletal system and need to be careful when attempting any form of physical activity to not inadvertently promote injury and subsequent immobility with all its detrimental consequences for further weight gain and loss of fitness.
Without question, people carrying extra weight are at high risk for mechanical injury to their musculoskeletal system and need to be careful when attempting any form of physical activity to not inadvertently promote injury and subsequent immobility with all its detrimental consequences for further weight gain and loss of fitness.
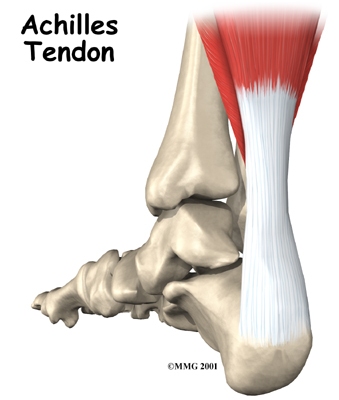
Apart from the excess mechanical pressures on the joints and ligaments, new research suggests that obesity may also play an important, hitherto largely unrecognized role, in tendinopathies, a common painful condition that affects the tendons rather than the joints. (Tedons are the ligament-like structures that attach muscles to bone and are thus the key tissues responsible for transferring muscle strength to the skeletal system.)
In a systematic review published in this month’s issue of Arthritis and Rheumatism, James Gaida and colleagues from Deakin University, Melbourne, Australia, examined studies that compared adiposity between subjects with and without tendon injury or examined adiposity as a predictor of conservative treatment success.
They identified 4 longitudinal cohorts, 14 cross-sectional studies, 8 case-control studies, and 2 interventional studies (28 in total), providing a total of 19,949 individuals.
Overall, the studies suggest a substantially increased risk for tendon injury associated with obesity, although there was some heterogeneity in study findings depending on study populations and mode of assessment.
This finding has some important implications:
1) it would be interesting to see if obesity treatment can indeed reduce the risk of tendon injury;
2) clinicians making exercise recommendations to individuals with excess weight must be fully aware of the increased potential for tendon injury and design exercise routines with this in mind.
Anyone, who has experienced tendon injury is well aware that once established, this condition is notoriously hard to treat and often results in chronic pain ultimately reducing mobility and thus further increasing the potential for weight gain.
Another good reason, why exercise professionals working with obese clients (as blogged before) need a sound understanding not just of exercise physiology but also of musculoskeletal pathology.
AMS
Edmonton, Alberta



