Critical Care for Critically Obese Patients
 Yes, the usual term is “morbidly” obese (a term I do not like), but today’s post is simply to draw my readers’ attention to a special issue of Critical Care Clinics dedicated entirely to the critical care of patients with severe obesity.
Yes, the usual term is “morbidly” obese (a term I do not like), but today’s post is simply to draw my readers’ attention to a special issue of Critical Care Clinics dedicated entirely to the critical care of patients with severe obesity.
This special issue is edited by Marilyn Haupt and Mary Jane Reed from Temple University School of Medicine, Danville, who describe the timeliness of this collection of articles as follows:
“As critical care practitioners, we have seen our ICU transformed over the last 20 years from a facility challenged with the care of an occasional morbidly obese patient to one that cares for multiple morbidly obese patients on a daily basis. Nevertheless, our approach to the management continues to be primarily empiric and without guidance from clinical research directed toward this population of patients. Although research is evolving in this area, large gaps in knowledge persist. Optimal dosing, for example, is unknown for many drugs, including those that may be lifesaving. Although a modest body of literature exists on antibiotic dosing in the obese, the studies addressing dosing of cardiac medications in these patients are infrequent and sporadic. Controversy continues to persist over whether a calorie-restricted diet is safe or beneficial in the critically ill obese patient.“
The issue contains a total of 21 articles ranging from the “obesity paradox” to hands-on topics like airway management, tracheostomy, vascular access, lumbar puncture, and radiological procedures.
There are articles on cardiovascular and pulmonary care, acute kidney failure, gastrointestinal complications, immunological changes, endocrine problems, venous thromoboembolic disease, hematological considerations, and pharmacotherapy.
Special situations and populations include trauma and disasters, severely obese children and pregnant mothers, and the bariatric surgery patient in the intensive care unit.
The series sensibly ends with a note on sensitivity in caring for patients with obesity – whereby, my only criticism of the entire series is in the frequent use of the word “obese” as a noun rather than an adjective (see my previous post on this issue).
With regard to this series, the editors note:
“Practitioners and clinical researchers with experience and interest have authored these articles, providing scientific backup whenever possible as well as wisdom and common sense that derives from years of practice. We hope that clinicians will find useful applications of this knowledge base and that clinical researchers will recognize areas requiring investigation.“
This is not a problem that is going away anytime soon, and the more clinicians familiarise themselves with these issues, the better they will be able to help their patients.
AMS
Hamilton, Ontario
Haupt MT, & Reed MJ (2010). Preface. Critical care clinics, 26 (4) PMID: 20970042
Obesity Paradox Holds for General Surgery
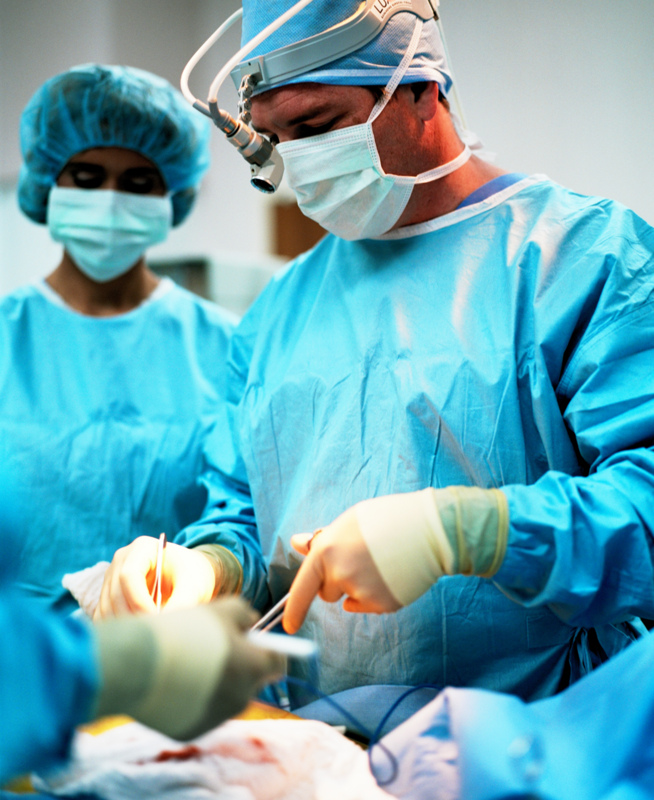 Regular readers of these posts will by now be quite familiar with the seemingly paradoxical survival benefit of carrying extra pounds in patients who have chronic diseases like heart or kidney failure, chronic lung disease or even critical illness that requires admission to an intensive care unit.
Regular readers of these posts will by now be quite familiar with the seemingly paradoxical survival benefit of carrying extra pounds in patients who have chronic diseases like heart or kidney failure, chronic lung disease or even critical illness that requires admission to an intensive care unit.
A new study by Mullen JT and colleagues from Harvard Medical School, Boston, USA, just out in the Annals of Surgery, suggests that the same may may be true for patient undergoing general surgery, i.e. surgery for reasons other than weight loss.
Their prospective, multi-institutional, risk-adjusted cohort study included 118,707 patients undergoing nonbariatric general surgery who were included in the National Surgical Quality Improvement Program Participant Use database in 2005 and 2006.
The risk of death according to BMI exhibited a reverse J-shaped relationship, with the highest rates in the underweight and morbidly obese extremes and the lowest rates in patients with overweight and moderate oebsity. Overweight and moderately obese patients had a 15% and 25% lower risk of death than normal weight patients, respectively.
However, beyond the moderately obese category, there was a progressive increase in the likelihood of a complication with increasing BMI class, almost entirely due to increasing rates of wound infection.
This finding is thus in line with previous data suggesting that overweight and moderately obese patients with critical illness have paradoxically “lower” risks of mortality compared with patients at a “normal” weight.
While this finding does not mean that normal weight people need to gain extra pounds prior to undergoing general surgery, it certainly does not support the idea that overweight or moderately obese individuals need to lose weight prior to undergoing an operation.
Recommendations to overweight and moderately obese individuals to lose weight prior to surgery may be more a reflection of weight bias than sound clinical judgement.
AMS
Edmonton, Alberta
Obesity and Emergency Intubation
 Intubation to secure a patent airway for ventilation is one of the most common procedures performed in the emergency care of severely injured trauma patients.
Intubation to secure a patent airway for ventilation is one of the most common procedures performed in the emergency care of severely injured trauma patients.
As anyone, who has performed intubations is well aware, the anatomic and physiological characteristics associated with obesity often makes the intubation of larger patients more challenging. It is therefore reasonable to assume that obese trauma patients requiring emergency intubation are at increased risk for unsuccessful intubation and airway-related complications.
But is this really the case?
To answer this question, Ziad Sifri and colleagues from the New Jersey Medical School, Newark, New Jersey, USA, performed a retrospective review of prospectively collected data from an airway surveillance database of 9,980 patients seen at an urban Level I trauma center between 2001 and 2004 (Journal of Trauma). The study population included all adult patients admitted to the trauma center, who required urgent airway management. The patients were stratified into four groups according to their BMI.
During the three-year study period, 1,435 (14%) were emergently intubated and made up the study population. About 92% of ED intubations were performed by the anesthesia team. Of all emergently intubated patients, 46% were lean, 37% were overweight, 15% were obese, and 2% were morbidly obese.
Interestingly, BMI was not an independent risk factor for failed intubations in the field or in the ED, postintubation airway complications, or death. Only early respiratory complications demonstrated a statistically significant, but unlikely clinically relevant association with a higher BMI.
The authors conclude that emergency intubation of obese trauma patients can be safely and successfully performed in a high volume Level I trauma center. Whether the same is true at less-experienced centres, of course, remains to be seen.
Overall, this study is very much in line with previous findings that body weight or size in itself is not a key determinant of patient outcome or survival in critical situations.
Clearly, in experienced hands, there is no reason to shy away from intubating patients with larger BMIs.
AMS
Edmonton, Alberta
Weighing in on In-Car Traffic Injuries
 Given the increase in average body size (and weight), it is not surprising that the automotive safety community is questioning the impact of obesity on the performance and assessment of occupant protection systems.
Given the increase in average body size (and weight), it is not surprising that the automotive safety community is questioning the impact of obesity on the performance and assessment of occupant protection systems.
This issue was recently addressed by David Viano and colleagues, who work at ProBiomechanics LLC, a Michigan firm specializing in occupant kinematics and injury causation, published last month in Traffic Injury Prevention.
The authors investigated the relationship between fatality and serious injury risks for front-seat occupants by body mass index (BMI) using a matched-pair analysis. They also developed a simple model for the change in injury risk with obesity which includes the normal mass (m) and stiffness (k) of the body resisting compression during a blunt impact. For a given impact severity, the risk of injury was assumed proportional to compression. Energy balance was used to determine injury risks with increasing mass.
Data for 1993-1004 was analyzed from the National Automotive Sampling System Crashworthiness Data Set (NASS-CDS), an ongoing study of more than 5,000 accidents each year, in which trained investigators look at wrecked vehicles, read through police reports, and talk to accident victims. Occupant injury was divided into normal and obese categories. A matched-pair analysis was carried out. Driver and front-right passenger fatalities or serious injuries (MAIS 3+) were analyzed in the same crash to determine the effect of obesity.
Based on the model, an obese occupant (BMI = 30-35 kg/m2) has 54-61% higher risk of injury than a normal BMI occupant (22 kg/m2). Matched pairs showed that obese drivers have a 97% higher risk of fatality and 17% higher risk of serious injury than normal BMI drivers. Obese passengers have a 32% higher fatality risk and a 40% higher risk than normal passengers. Obese female drivers have a 119% higher risk than normal BMI female drivers and young obese drivers have a 20% higher serious injury risk than young normal drivers.
These data add to several prior publications highlighting the increased risk for overweight and obese drivers and passengers in automobiles.
Viano and colleagues also estimated how much extra ballast the family of Hybrid III crash test dummies would need to represent an obese or morbidly obese occupant. According to these assessments, the smallest crash test dummies need proportionately more ballast to represent an obese or morbidly obese occupant in the evaluation of safety systems. The 5% female Hybrid III (BMI = 20.4) and needs 22 kg of ballast to represent an obese and 44.8 kg to represent a morbidly obese female, while the 95% male needs only 1.7 and 36.5 kg, respectively.
The authors conclude that
“Obesity influences the risk of serious and fatal injury in motor vehicle crashes. The effect is greatest on obese female drivers and young drivers. Since some of the risk difference is related to lower seatbelt wearing rates, the comfort and use of seatbelt extenders should be examined to improve wearing rates by obese occupants. Also, crash testing with ballasted dummies to represent obese and morbidly obese occupants may lead to refined safety systems for this growing segment of the population.“
As also noted recently by Ben Zarzaur and Stephen Marshall, Surgeons at the University of Tennessee Health Science Center, Memphis, in The Journal of Trauma, the combination of obesity and not using a seat belt is particularly deadly.
Most importantly, David Schlundt and colleagues from Vanderbilt University just reported in OBESITY based on data from the 2002 Behavioral Risk Factor Surveillance System Survey, that seatbelt use declines as BMI increases, with approximately 55 percent of extremely obese individuals say that they do not use a seatbelt.
Consequence of these finding for counseling our obese patients: buy cars where seatbelts fit your size or buy seatbelt extenders AND USE THEM!
Sounds like a class-action waiting to happen!
AMS
Edmonton, Alberta
Is Obesity Critical in Critical Care?
Although obesity is now well-recognized as a risk factor for the development of many chronic diseases, its role in acute situations is less clear.
So while one might assume that severe obesity in critical ill patients is a predictor of poor outcomes, this hypothesis was not confirmed in a recent meta-analysis of studies comparing outcomes in obese (BMI > 30 kg/m2) critically ill patients in intensive care settings published by Akinnusi and colleagues from the University of Buffalo School of Medicine in the January issue of Critical Care Medicine (for Abstract click here).
Fourteen studies with 15,347 obese patients met inclusion criteria. Surprisingly, obesity was not associated with an increased risk of intensive care unit mortality, albeit duration of mechanical ventilation and intensive care unit length of stay were statistically but not remarkably longer in the obese group.
Interestingly, in a subgroup analysis, an improved survival was observed in obese patients with body mass index ranging between 30 and 39.9 compared with nonobese patients (relative risk, 0.86; 95% Cl, 0.81-0.91; p < .001). This latter finding is reminiscent of the "obesity survival paradox” alluded to in previous blogs.
Clearly, obesity is not a significant risk factor for poor survival outcomes in critical care. Whether or not this also applies to the subset of extremely obese patients that are now increasingly seen in hospital settings remains to be seen.
AMS


