Antipsychotic Prescriptions to Children – Too Much Too Soon?
 Following yesterday’s post on the issue of weight gain and metabolic syndrome seen in kids treated with second-generation antipsychotics (SGAs), today, I look at another paper by Silvia Alessi-Severini and colleagues from the University of Manitoba published in the same issue of the Canadian Journal of Psychiatry.
Following yesterday’s post on the issue of weight gain and metabolic syndrome seen in kids treated with second-generation antipsychotics (SGAs), today, I look at another paper by Silvia Alessi-Severini and colleagues from the University of Manitoba published in the same issue of the Canadian Journal of Psychiatry.
This paper examines the use of antipsychotics in children and adolescents (aged 18 years or younger) based on data collected from the administrative health databases of Manitoba Health and the Statistics Canada census between the fiscal years of 1999 and 2008.
Over these 10 years, prevalence of antipsychotic use increased with the introduction of the SGAs from 1.9 per 1000 in 1999 to 7.4 per 1000 in 2008.
The male-to-female antipsychotic usage ratio increased from 1.9 to 2.7 as the male youth population represented the fastest-growing subgroup of antipsychotic users in the entire population of Manitoba.
Notably, the paper finds that total number of prescriptions also increased significantly despite the lack of approved indications in this population.
More than 70% of antipsychotic prescriptions to children and adolescents were written by general practitioners with the most common diagnoses being attention-deficit hyperactivity disorder and conduct disorders. In fact, the use of antipsychotics in combination with methylphenidate (ritalin) increased from 13% to 43%.
Thus, it appears that there is extensive off-label use of SGAs in kids and youth in Manitoba (and likely in other provinces), a finding that is of concern not least because of the significant (30-fold increased) risk of weight gain and metabolic syndrome associated with the use of these compounds.
So, while there is no doubt that these drugs may provide important clinical benefits in kids who do need them, it is hard to imagine that this degree of off-lable prescription is indeed warranted.
Again, I would love to hear from my readers regarding experience with these medications in children and youth.
AMS
Ottawa, Ontario
Attention Deficit Disorder
 Today’s post is another excerpt from “Best Weight: A Practical Guide to Office-Based Weight Management“, recently published by the Canadian Obesity Network.
Today’s post is another excerpt from “Best Weight: A Practical Guide to Office-Based Weight Management“, recently published by the Canadian Obesity Network.
This guide is meant for health professionals dealing with obese clients and is NOT a self-management tool or weight-loss program. However, I assume that even general readers may find some of this material of interest.
ATTENTION DEFICIT DISORDER
Attention deficit disorder with or without hyperactivity (ADD or ADHD) and impulsiveness has been associated with increased risk for weight gain in both children and adults. In one study, ADHD was present in over 25% of all obese patients and 40% of patients with class III obesity. Reasons for this prevalent co-morbidity are unknown, but brain dopamine or insulin receptor activity may be involved.
Patients with ADD or ADHD usually manifest a long history (since childhood) of impulsivity, lack of concentration, decreased attention, inability to complete tasks, impairment in school or work performance and social dysfunction. Being “hyperactive” in the sense of the DSM-IV diagnosis of ADHD does not prevent the development or persistence of overweight and obesity in children.
Bariatric patients showing poor focus during treatment should be investigated for ADD or ADHD. Identifying the disorder is crucial as they will not be able to focus on the weight- management plan until their impulsiveness and lack of concentration are addressed.
Pharmacological and behavioural therapies can often help patients improve task persistence and decrease impulsivity and distractibility, which will increase the likelihood of success with weight-control efforts.
© Copyright 2010 by Dr. Arya M. Sharma and Dr. Yoni Freedhoff. All rights reserved.
The opinions in this book are those of the authors and do not represent those of the Canadian Obesity Network.
Members of the Canadian Obesity Network can download Best Weight for free.
Best Weight is also available at Amazon and Barnes & Nobles (part of the proceeds from all sales go to support the Canadian Obesity Network)
If you have already read Best Weight, please take a few minutes to leave a review on the Amazon or Barnes & Nobles website.
Cognitive Behavioural Therapy for Attention Deficit Disorder
 Regular readers will recall that almost 30% of adults with severe obesity may have signs of attention deficit hyperactivity disorder (ADHD) and, when present, this can be a major barrier to weight management.
Regular readers will recall that almost 30% of adults with severe obesity may have signs of attention deficit hyperactivity disorder (ADHD) and, when present, this can be a major barrier to weight management.
Thus, all patient in our obesity clinic are routinely screened for ADHD and often treating this condition is the first step to successful weight management.
However, not all patients with ADHD are willing to undergo treatment, some do not tolerate the medications, and in others, medications are simply not effective enough.
Now, a study by Steven Safren and colleagues from Harvard University, Boston, MA, published in JAMA, demonstrates the effectiveness of adding cognitive behavioural therapy (CBT) to medication for better control of ADHD.
Safren and colleagues randomised 86 symptomatic adults with ADHD who were already being treated with medication to 12 individual sessions of either cognitive behavioral therapy or relaxation with educational support (controls). 79 participants completed treatment and 70 completed the 12 month follow-up assessments.
CBT was delivered according to the manual, “Mastering Your Adult ADHD” and consisted of 3 core modules and 2 optional modules. The first module (4 sessions) focused on psychoeducation about ADHD and training in organizing and planning (use of calendar and task list system), including problem-solving training (generating alternatives and picking the best solution, breaking down overwhelming tasks into steps).
The second module (2 sessions) involved learning skills to reduce distractibility, such as techniques to time the length of one’s attention span, and, when doing a task, write down distractions vs acting on them. The third module (3 sessions) was cognitive restructuring, which involved learning to think more adaptively in situations that cause distress.
Optional modules were one session of application of skills to procrastination and one session including the patient’s family member for support.
Patients for whom the optional sessions were not relevant had booster sessions on prior material.
The final session was focused on review and relapse prevention.
Patients in the relaxation condition received training in progressive muscle relaxation and other relaxation techniques as applied to ADHD symptoms, as well as education about ADHD and supportive psychotherapy.
Participants undergoing the CBT intervention achieved lower posttreatment scores and self-reported significant improvement in symptoms. Participants in the CBT arm were about four-times more likely to respond compared to the relaxation group. Most of this response was maintained over 6 and 12 months.
This study demonstrates that the use of CBT in adults with persistent ADHD symptoms despite medication can provide important clinical benefits not seen with relaxation techniques. It is likely that CBT may also be the treatment of choice for patients who refuse medical treatment or would like to reduce their dose of ADHD medications.
AMS
Edmonton, Alberta
You can now also follow me and post your comments on Facebook
Safren SA, Sprich S, Mimiaga MJ, Surman C, Knouse L, Groves M, & Otto MW (2010). Cognitive behavioral therapy vs relaxation with educational support for medication-treated adults with ADHD and persistent symptoms: a randomized controlled trial. JAMA : the journal of the American Medical Association, 304 (8), 875-80 PMID: 20736471
Energy Expenditure in ADHD Kids
 I have repeatedly posted on the relationship between Attention Hyperactivity Deficit Disorder (ADHD) and obesity. We see a remarkable number of adults with this disorder in our bariatric clinic and, as blogged before, treating this disorder is often a key step in helping these patients manage their weight.
I have repeatedly posted on the relationship between Attention Hyperactivity Deficit Disorder (ADHD) and obesity. We see a remarkable number of adults with this disorder in our bariatric clinic and, as blogged before, treating this disorder is often a key step in helping these patients manage their weight.
In kids, this disorder is often characterized by substantial hyperactivity, which would be expected to burn more calories. But what about the impact of ADHD on resting energy expenditure (REE) and the thermogenic effect of food (together accounting for about 60% if not more of the daily calories burnt)?
This question was addressed by my colleague Thomas Mueller and other researchers from the University of Alberta in a paper just published online in Eating and Weight Disorders.
Mueller and his team studied 12 pre-pubertal boys with untreated ADHD of the hyperactive-impulsive type and 12 control boys without ADHD. In addition, they examined an independent group of 60 boys with ADHD.
On average, REE was 6.5 kcal/kg fat free mass/day higher in the ADHD compared to the control group. However, there was no difference in the thermogenic effect of food between groups. Neither age nor restlessness explained the differences in REE.
Despite the higher REE (and likely higher activity energy expenditiure due to the innate restlessness that comes with this condition), boys with ADHD had similar BMI levels compared to non-ADHD reference groups.
Thus, this paper shows that despite a notably greater energy expenditure, ADHD kids are not generally leaner, clearly suggesting that they manage to make up for their greater energy needs through higher caloric intake.
One may well speculate that as these kids become older and their REEs (and activity expenditures?) decrease, persistence of a higher caloric intake than their non-ADHD peers may well make them more prone to obesity as adults.
How and why REE is elevated in ADHD clearly deserves further study. I’d certainly appreciate hearing from any of my readers, who have experience with the ingestive behaviour of ADHD kids.
AMS
Burlington, Ontario
Please Pay Attention – You May Have Obesity
While I am taking a brief break from clinics and other obligations (including daily blog posts), I will be reposting past articles, which I still believe to be relevant but may have escaped the attention of the 100s of new readers who have signed up in the past months.
The following was first posted on 04/01/08 (For more recent posts on this topic click here)
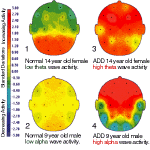 There are over 50 recent publications in PubMed on the possible link between Attention Deficit Disorder (ADD) and obesity. In my own anecdotal experience I continue to be surprised on how many patients presenting with obesity have clear signs of this disorder.
There are over 50 recent publications in PubMed on the possible link between Attention Deficit Disorder (ADD) and obesity. In my own anecdotal experience I continue to be surprised on how many patients presenting with obesity have clear signs of this disorder.
They are usually the patients who show up late for appointments because they locked their keys in their cars, did not fill the last prescription for their metformin because they lost it, started filling out food records but never got past the first day, used their new bike only once because they never got around to fixing the flat tire from their first ride, take a packed lunch to work but forget to eat it, enthusiastically start a new diet but lose interest three days later because weight loss is too slow – I could go on forever – you probably get the picture.
In my practice I have come to recognize that ADD is probably one of the most common and frustrating barriers to obesity management. By definition, individuals with ADD lack the ability to plan ahead and to follow through on their plans, easily lose interest, and are constantly sabotaged by their impulsiveness when it comes to making healthy choices.
There is now evidence to support the notion that alterations in the dopaminergic reward system may be common to both ADD and hedonistic hyperphagia. Not surprisingly there is some work showing that methylphenidate (ritalin) can sometimes reduce cravings for sweet and fatty foods.
It does not surprise me that someone with ADD is probably more prone to “mindless eating” and thus more likely to gain weight than someone with proper impulse control.
One of the most remarkable cases I recall was a patient, who after being started on ritalin, at his next visit for the first time brought in and proudly presented meticulously completed food records (he was also a couple of pounds lighter).
In medicine it is always easiest to blame the patient – not motivated, not interested, not focused, not following instructions, not compliant, not adherent, etc.
Recognizing that this behavior may be due to ADD and providing proper treatment for this condition may in these cases be the first step to obesity management.
AMS
Edmonton, Alberta


