Osteoarthritis Management in Obesity
Tuesday, April 19, 2011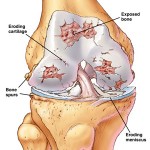 Osteoarthritis is one of the most disabling and painful conditions attributable (in part) to excess weight. Once established, osteoarthritis significantly reduces quality of life and mobility, often precipitating further weight gain and posing an important barrier to weight management.
Osteoarthritis is one of the most disabling and painful conditions attributable (in part) to excess weight. Once established, osteoarthritis significantly reduces quality of life and mobility, often precipitating further weight gain and posing an important barrier to weight management.
A panel of experts (The Ottawa Panel) has now released a comprehensive set of evidence-based clinical practice guidelines for the management of osteoarthritis in overweight and obese patients, published in PHYSICAL THERAPY.
The recommendations are based on an extensive review of published articles with strict application of quality criteria to rate the strength of evidence (A, B, C, C+, D, D+, or D-) as well as experimental design (I for randomized controlled trials and II for nonrandomized studies).
Clinical significance was established by an improvement of ≥15% in the experimental group compared with the control group.
The panel decided on a total of 79 recommendations: 36 positive (21 grade A and 15 grade C+) – all were of clinical benefit.
Overall the data supports the recommendation that physical activity combined with (mildly restrictive) diet programs are beneficial for pain relief, functional status, strength and quality of life.
Although 5% reduction in body weight reduced pain and functional status, this degree of weight loss was insufficient to slow disease progression.
Both aquatic and land-based aerobic exercise were shown to be more effective in reducing pain than home-based strengthening exercises. On the other hand, land-based exercise performed in a gym that included strength, aerobic, stretching, and range-of-motion training was more effective in reducing pain compared with a home-based strengthening exercise program.
These benefits of exercise are independent of any changes in body weight and the authors suggest:
“The significant improvements in QoL among study participants with OA who were obese or overweight may be a reflection of mental health and social benefits associated with the participation in physical activities. Physical activity promotes psychological well-being by reducing feelings of fatigue, depression, and anxiety and improving self-esteem, confidence, concentration, and mental awareness. The social benefits of participation in physical activity include a reduction in the sense of isolation and loneliness, improved social networks and social capital, and increased community connectedness and cohesion.”
Importantly, the authors also note that:
“To the knowledge of the Ottawa Panel, there is no conclusive evidence on the most appropriate methodological scale to apply for OA and obesity research. The use of BMI, waist circumference, and body weight as valid indicators of successful weight loss in individuals with OA is debatable because these measurements do not discriminate between lean and fat body mass.”
Nevertheless, the panel recommends:
“…reducing weight prior to the implementation of weight-bearing exercise to maintain joint integrity and to avoid joint disease and dysfunction.”
How this weight loss is best achieved (and maintained) of course remains open to debate.
Importantly perhaps, the readers should also note that the review did not look at surgical studies, where patients generally experience substantially greater weight loss than with ‘diet and exercise’ alone.
I would certainly love to hear my readers’ experience of the impact of diet and exercise and/or weight loss on their osteoarthritis symptoms. What worked? What didn’t?
AMS
Edmonton, Alberta
p.s. the issue of osteoarthritis and obesity will be an important topic at the upcoming 2nd National Obesity Summit in Montreal next week.
Brosseau L, Wells GA, Tugwell P, Egan M, Dubouloz CJ, Casimiro L, Bugnariu N, Welch VA, De Angelis G, Francoeur L, Milne S, Loew L, McEwan J, Messier SP, Doucet E, Kenny GP, Prud’homme D, Lineker S, Bell M, Poitras S, Li JX, Finestone HM, Laferrière L, Haines-Wangda A, Russell-Doreleyers M, Lambert K, Marshall AD, Cartizzone M, & Teav A (2011). Ottawa Panel Evidence-Based Clinical Practice Guidelines for the Management of Osteoarthritis in Adults Who Are Obese or Overweight. Physical therapy PMID: 21493746


