Lifestyle Patterns Among Obese Adults – Chicken or Egg?
Tuesday, November 3, 2009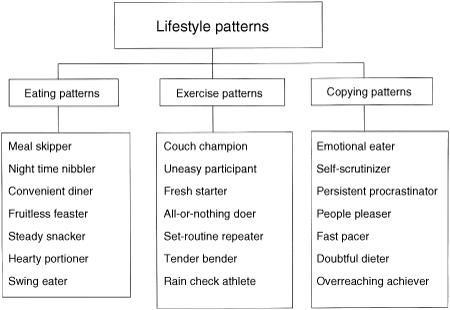 Weight gain is the result of positive energy balance and the only way you can get into positive balance is if energy input exceeds output.
Weight gain is the result of positive energy balance and the only way you can get into positive balance is if energy input exceeds output.
As all calories enter the body as food or drink, ingestive behaviour is obviously an important determinant of energy balance.
Although physical activity accounts for only around one-third of total energy expenditure (two-thirds of energy is burnt just to keep your body alive), it is still an important component of energy balance.
It is therefore not surprising when studies find that “eating too much” or “not moving enough” is often (but not always!) associated with weight gain.
This is in fact exactly what was found in a new study by Robert Kushner and SW Choi from the Northwestern University, Chicago, IL, just published in OBESITY.
This study looked at responses to a 53-item lifestyle pattern questionnaire posted on a commercial weight loss program Web site (2004- 2008) in 446,608 adults with an average BMI of 30.5. Categorically, 25.5% were healthy weight, 29.0% were overweight, 33.7% were class I-II obesity, and 11.8% class III obesity.
A stratified random sample was used to estimate the prevalence of 21 lifestyle patterns (7 eating, 7 exercise, and 7 coping: figure) and the odds ratio of the pattern prevalence for each BMI category.
“Unhealthy” lifestyle patterns in diet, exercise, and coping were highly prevalent among the entire population, whereby, the prevalence of these patterns rose with increasing BMI and advancing age.
Gender differences were seen with many of the patterns, most noticeably among the coping patterns. Thus, prevalence of five coping patterns was noticeably higher among women compared to men: emotional eater (41% vs. 29%), self-scrutinizer (negative self-talk) (52% vs. 27%), persistent procrastinator (73% vs. 61%), people pleaser (low self-care) (54% vs. 40%), and doubtful dieter (pessimistic thinking) (41% vs. 29%).
Overall, the lifestyle patterns and terminology used in this study is reminiscent of the “personality types” that Dr. Kushner has described before (see previous blog entry on this).
Based on the current study, the authors conclude that “unhealthy” behavioural patterns are associated with obesity and that behavioural pattern recognition could help identify patients at risk.
For me the paper raises more questions than it answers:
Firstly, I was surprised that despite the significant associations, the effect sizes of individual patterns was actually quite low: this means that a lot of people in the “healthy weight” range apparently also engage in these “unhealthy” behaviours – so why do they not gain weight? Are we missing something?
Secondly, even if these “unhealthy” behaviours are major determinants of weight gain (and not just associations), the real question is what underlies these behaviours – after all, as blogged before, more important than “what someone does” is “why does it” (see Obesity is a Sign, Overeating is a Symptom).
Thus, someone could be a “Couch Champion” because of arthritis, depression, cardio-respiratory disease, low self-efficacy, agorophobia, fibromyalgia, or any number of other reasons that may limit physical activity.
Similarly, the “Meal Skipper” could have attention deficit order, irregular working hours, long commutes, high stress levels or simply false ideas about dieting.
Clearly, to understand obesity, we must move beyond simply describing behaviours to truly understanding the root causes of such behaviours. Any approach to obesity that focuses on behaviours (i.e. “eat less – move more”) while ignoring the key determinants of these behaviours is unlikely to succeed.
AMS
Edmonton, Alberta


