What Can Best Practices Achieve in The Treatment of Severe Obesity?
Monday, January 13, 2014Despite “miracle” foods, diet “breakthroughs” and “success” stories promoted in popular media and by commercial weight-loss programs, the reality of achieving and sustaining weight loss, even with the best evidence-based medical care remains modest at best.
A new paper by Raj Padwal and colleagues from the University of Alberta, published in Medical Care, now describes the weight outcomes from a prospective two-year naturalistic evaluation (APPLES) of parallel cohorts of 500 patients while on waiting list (n=150), undergoing medical (n=200) or surgical (n=150) management in a large Edmonton-based publicly funded multi-disciplinary bariatric program (Weight Wise).
This comprehensive bariatric program delivers integrated, patient-focused, evidence-based care to the Edmonton Zone of Alberta Health Services. This region is one of the largest integrated health delivery systems in Canada and includes a catchment population of approximately 1.6 million residents.
Specific features of the program include a central, region-wide single-point-of-access referral system; community education and weight management sessions; and bariatric specialty services offered to patients with BMI levels of great than 35 kg/m2 referred from a medical practitioner.
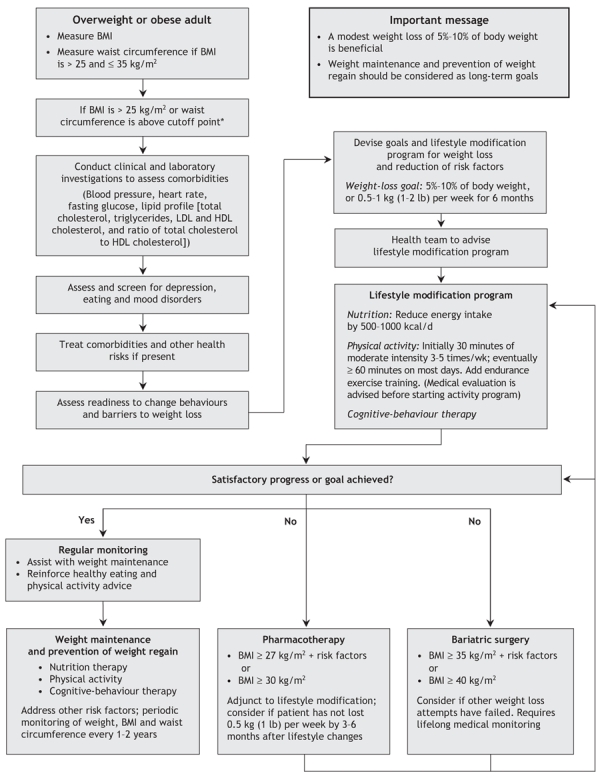
The program is structured such that patients progress from the wait-list to intensive medical management through to bariatric surgery (if indicated).
When the APPLES study, funded by the Canadian Institutes of Health Research (CIHR) as the first evaluation of representative outcomes in a publicly funded bariatric program in Canada, began in 2008, approximately 800 new patients were seen and about 200 surgeries were performed annually in the program. At that time there were also 1,500 adults waitlisted for clinic entry (2-y average wait time).
The results of the APPLES study are of considerable interest, as publicly funded bariatric services in Canada differ from commercial and third-party payor programs in that they are universally accessible, centrally triaged and population-based.
These features, likely also mean that patients seen in these programs are less highly selected and perhaps more treatment-refractory than those seen in private payor settings.
Moreover, the evidence-based nature of the interdisciplinary services provided in this tertiary care setting represent the current standard of specialised bariatric care.
However, the prime importance of these data lie in the fact that, contrary to the current “benchmark” weight-loss data derived largely from randomized controlled trials or programs enrolling highly selected populations, the APPLES study, for the first time, provides Canadian real-life data on the efficacy and effectiveness of publicly funded bariatric care (albeit at a specialised tertiary care centre).
Importantly, APPLES was conducted as a prospective study, thus largely avoiding the problems commonly seen in retrospective case-control analyses (e.g. confounding and selection bias).
In the coming posts, I will discuss the results and considerations arising from the findings of the three arms of the APPLES study – the waiting list, the medically managed and the surgically managed patients – each of which provides important insights into the outcomes and challenges in managing patients with severe obesity.
At this point a short mention and vote of thanks to all of the patients, who agreed to participate in this project.
@DrSharma
Edmonton, AB
![]() Padwal RS, Rueda-Clausen CF, Sharma AM, Agborsangaya CB, Klarenbach S, Birch DW, Karmali S, McCargar L, & Majumdar SR (2013). Weight Loss and Outcomes in Wait-listed, Medically Managed, and Surgically Treated Patients Enrolled in a Population-based Bariatric Program: Prospective Cohort Study. Medical care PMID: 24374423
Padwal RS, Rueda-Clausen CF, Sharma AM, Agborsangaya CB, Klarenbach S, Birch DW, Karmali S, McCargar L, & Majumdar SR (2013). Weight Loss and Outcomes in Wait-listed, Medically Managed, and Surgically Treated Patients Enrolled in a Population-based Bariatric Program: Prospective Cohort Study. Medical care PMID: 24374423
.