Treating Obesity In People With Prediabetes Could Save Billions
Monday, September 12, 2011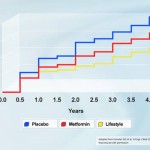 Today, as I attend the 47th European Association for the Study of Diabetes (EASD) Annual Meeting here in Lisbon, I cannot help but discuss an article by Kenneth E. Thorpe and Zhou Yang, Emory University, Atlanta, Georgia, published in the latest issue of Health Affairs.
Today, as I attend the 47th European Association for the Study of Diabetes (EASD) Annual Meeting here in Lisbon, I cannot help but discuss an article by Kenneth E. Thorpe and Zhou Yang, Emory University, Atlanta, Georgia, published in the latest issue of Health Affairs.
Based on their analysis of the significant impact of even modest sustained weight reduction on the incidence of type 2 diabetes, these authors suggest that enrolling overweight and obese pre-diabetic US adults aged 60–64 into a proven, community-based weight loss program nationwide could save Medicare $1.8–$2.3 billion over the following ten years.
Estimated savings would be even higher ($3.0–$3.7 billion) if equally overweight people at risk for cardiovascular disease were also enrolled.
Thus, lifetime Medicare savings could range from approximately $7 billion to $15 billion, depending on how broadly program eligibility was defined and actual levels of program participation, for a single “wave” of eligible people.
A key assumption in their proposal, is that a fully funded sixteen-twenty week community program (perhaps delivered by the YMCA), would deliver about 4% weight loss and replicate the almost 50-70% reduction in progression to diabetes seen in some diabetes prevention studies.
Using our Edmonton Obesity Staging System definitions – this program would target Stage 1 patients (pre-diabetes) or Stage 2 patients (with hypertension or dyslipidemia).
There is no doubt that community based ‘lifestyle’ interventions are the only plausible way in which any program can be delivered to millions of eligible individuals. There is also little doubt that in randomised controlled trials, considerable benefits have been demonstrated.
The question remains, however, whether enough eligible participants will in fact participate and persist with these ‘lifestyle’ changes without continuing and ongoing support (which is generally what the clinical trials have delivered). The notion that an intervention of limited duration (even twenty weeks) will lead to sustainable effects, may be a bit over optimistic, even if 10 year follow-up data from some diabetes preventions studies suggest long-term benefits even after the end of the trials.
It is also worth discussing whether or not success is actually dependent on losing weight (not a behaviour) rather than simply increasing physical activity and eating better (which are behaviours).
Whether or not there is indeed a realistic chance that millions of people can be enrolled in community based interventions programs will remain to be seen, but it is certain that, if feasible, savings would indeed be substantial.
This is why, in the recently announced Alberta Health Services Obesity Initiative, there is a significant emphasis on the importance of community based programs (such as Thr!ve on Wellness, a joint initiative from Alberta Health Services and the Alberta Cancer Foundation, which will soon be expanded to over 100 Alberta communities).
If successfully adopted, these programs should have benefits far beyond diabetes prevention and reduce rates of heart disease, cancers, musculoskeletal problems and hopefully also improve mental health and well being.
Perhaps this is when we can truly claim to be moving towards a ‘health care’ rather than a ‘sickness care’ system.
AMS
Lisbon, Portugal
Thorpe KE, & Yang Z (2011). Enrolling people with prediabetes ages 60-64 in a proven weight loss program could save medicare $7 billion or more. Health affairs (Project Hope), 30 (9), 1673-9 PMID: 21900657


