Obesity in Indian Girls and Women
 During my current visit to New Delhi, it is hard to overlook the substantial increase in the prevalence of obesity in Indian men and women. While this may not be the phenotype that immediately comes to mind when thinking of India, there is no doubt that obesity prevalence is continuing to rise at an alarming rate.
During my current visit to New Delhi, it is hard to overlook the substantial increase in the prevalence of obesity in Indian men and women. While this may not be the phenotype that immediately comes to mind when thinking of India, there is no doubt that obesity prevalence is continuing to rise at an alarming rate.
Recent evidence for this comes from a study published by Chopra and colleagues from New Delhi, published in a recent issue of the European Journal of Clinical Nutrition.
In this systematic review of obesity in Indian girls and women were found to have consistently higher obesity rates than Indian boys or men.
Interestingly enough, abdominal obesity, sometimes referred to as ‘male-pattern’ obesity is in fact more common in Indian women than in men.
Not surprisingly, this increased rate of obesity is reflected in an increasing prevalence of type 2 diabetes that was reported to be as high as 14% in the 2001 National Urban Diabetes Survey.
Clustering of cardiovascular disease risk factors was further increased in post-menopausal women, not least due to a number of factors that may be of particular relevance in Indian women including sedentariness and overly caloric diets.
How exactly these increasing rates of obesity can be addressed remains anyones guess. While it is easy to see the proliferation of “slimming-centres” and “spas” at every corner, as in the West, these centres often provide little long-term help and of course generally do not cater to the folks, who would likely benefit the most.
Needless to say, the medical system in India, is as overwhelmed and insufficiently prepared to address obesity, as we are in the West.
Clearly a challenge if I ever saw one.
AMS
New Delhi, India
Will Lifestyle Changes Improve Polycystic Ovary Syndrome?
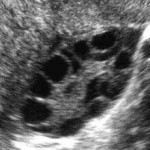 Polycystic ovary syndrome (PCOS) affects 4% to 18% of reproductive-aged women and is associated with significant reproductive, metabolic and psychological problems.
Polycystic ovary syndrome (PCOS) affects 4% to 18% of reproductive-aged women and is associated with significant reproductive, metabolic and psychological problems.
Obesity, not always, but often, an accompanying problem, worsens the presentation of PCOS. Current treatment guidelines for PCO, therefore, strongly recommend ‘weight management’ (both weight loss and the prevention of excess weight gain) through diet and exercise as an initial treatment strategy.
But how effective are these ‘lifestyle’ strategies and how consistent are the improvements?
This was the topic of a recent review by Lisa Moran and colleagues from Australia, published in the Cochrane Database of Systematic Reviews.
The authors identified six randomised controlled trial (including a total of 165 participants). Three studies compared physical activity to minimal dietary and behavioural advice or no advice; three compared combined dietary, exercise and behavioural interventions to minimal intervention.
Although these interventions resulted in modest weigh loss (~3.5 kg) and significantly reduced testosterone levels and associated male-pattern hair growth (hrisutism) as well as fasting insulin levels, there was no relevant effect on glucose or lipid levels or other cardiovascular risk factors.
Notably, none of these studies examined the impact of these interventions on quality of life, patient satisfaction or reproductive health (a common problem in PCOS). There was also no assessment of depression or anxiety, which have been reported to be commonly associated with PCOS.
Perhaps, as the authors point out, the most important result of this analysis is the apparent paucity of large studies that have addressed this issue – surprising enough, given that as many as 1 in 5 women of reproductive age may present with this problem and PCOS is a major cause of female infertility.
As the authors note:
“This review has identified that there are limited well-designed studies in lifestyle intervention in PCOS that are available to guide clinical practice.”
Given the impact of PCOS on reproductive health, it is most surprising that
“There are no existing RCT data identified in this review to assess whether lifestyle intervention improves reproductive outcomes including fertility, menstrual regularity or ovulation”
The overall conclusion is thus rather sobering:
“With the current evidence, it is not possible to comment on the relative effectiveness or sustainability of different durations or types of lifestyle interventions, or their relative success, in a weight loss or non-weight loss environment or with overweight or non-overweight participants……this indicates a considerable gap in the research literature.”
On other hand, this paucity of data should not be interpreted to show that interventions aimed at weight management do not impact on fertility or reproductive health in overweight and obese women with PCOS. Indeed, there is now accumulating anecdotal evidence that more significant weight loss (as can be achieved with bariatric surgery) may prove most beneficial in women with PCOS both in terms of reducing symptoms as well as in improving chances of conception.
Still, one wonders why a topic of such importance has not received more attention from researchers or funding agencies.
AMS
New York, NY
Moran LJ, Hutchison SK, Norman RJ, & Teede HJ (2011). Lifestyle changes in women with polycystic ovary syndrome. Cochrane database of systematic reviews (Online) (2) PMID: 21328294
Treatment Options For Polycystic Ovary Syndrome
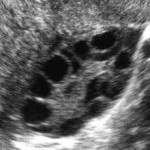 Polycystic Ovary Syndrome (PCOS) is by far the most common endocrine problem in women and may be present in about one in five women who fail to get pregnant.
Polycystic Ovary Syndrome (PCOS) is by far the most common endocrine problem in women and may be present in about one in five women who fail to get pregnant.
Although the exact etiology of PCOS remains unclear, it is commonly associated with overweight and obesity, with patients often (but not always!) presenting with signs of increased androgen production (or action) and (often quite severe) insulin resistance.
Clinically the signs and symptoms of PCOS can range from mild menstrual disorders to severe disturbance of reproductive and metabolic functions.
Because of its variability, the definition of PCOS has changed over the years – current diagnoses requires the demonstration of hyperandrogenism and ovarian dysfunction (including infrequent or irregular ovulation or anovulation) and/or polycystic ovaries as demonstrated by imaging (e.g. ultrasound).
A paper by Ahmed Badawy and Abubaker Elnashar from the Universities of Mansoura and Benha, Egypt, just published in the International Journal of Women’s Health, presents a comprehensive overview of the current treatment options for PCOS.
With regard to excess weight, the authors note:
Obesity is observed in 35%–60% of women with PCOS and is related to lack of or delayed response to different treatments…Weight loss improves the endocrine profile and increases the likelihood of ovulation and pregnancy. Normalization of the menstrual cycles and ovulation could occur with modest weight loss as little as 5% of the initial weight. Weight loss can improve not only circulating androgen and glucose levels but also ovulation and pregnancy rates in obese women with PCOS.
The authors also report that a few recent studies describe high success rates in restoring regular cycles and pregnancies in severely obese women with PCOS, who underwent bariatric surgery.
The paper describes in great detail other treatment options that can often complement weight loss, including the use of medications such as clomiphene citrate, tamoxifen, aromatase inhibitors, metformin, glucocorticoids, or gonadotropins or even surgically by laparoscopic ovarian drilling.
Treatment options of course also include in vitro fertilization as a last resort to achieve pregnancy when all other treatments fail.
The paper also touches on the treatment of androgenic symptoms, such as excessive hair growth on the body and face, balding, or acne.
Given that PCOS is such a common problem, I wonder if my readers wish to share their experience with managing this syndrome.
As always, comments are greatly appreciated.
AMS
Edmonton, Canada
Badawy A, & Elnashar A (2011). Treatment options for polycystic ovary syndrome. International journal of women’s health, 3, 25-35 PMID: 21339935
Gender Differences in Trauma and Addictions
 This week, I am attending a Scientific Symposium called “Recovery From Addiction“, organised as part of the Alberta Family Wellness Initiative of the Norlien Foundation. My interest in this meeting (where, for once, I am not a speaker on the program), comes from the close links between mental health, addictions and obesity that I regularly note in my patients.
This week, I am attending a Scientific Symposium called “Recovery From Addiction“, organised as part of the Alberta Family Wellness Initiative of the Norlien Foundation. My interest in this meeting (where, for once, I am not a speaker on the program), comes from the close links between mental health, addictions and obesity that I regularly note in my patients.
As someone with no formal training in diagnosing or treating addiction disorders, this symposium is turning out to be most interesting.
Yesterday, much of the program focussed on the link between trauma and addictions; on how addictive behaviours (including food addictions) can result from a wide range of traumatic experiences.
I was particularly interested in the presentation by Stephanie Covington from the Institute for Relational Development at the Center for Gender and Justice, La Jolla, CA, who talked about the important differences in both the nature and behavioural impact of trauma between genders.
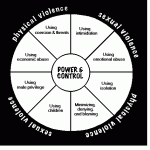
Some of these differences are profound and should be noted by anyone dealing with trauma in men and women. For example, while much of the mental, physical or sexual trauma in men is often inflicted by strangers, women often experience these traumas from very people they love and want to be close to. Perhaps not surprisingly, women often have a history of domestic violence, something men are far less likely to have experienced.
This perhaps explains the very different responses that men and women have to trauma: while men tend to respond to trauma with destructive actions (aggression, violence, rages), women tend to respond more often with retreat (isolation, dissociation, depression, anxiety). Interestingly, both genders can respond with self-destructive action (substance abuse, eating disorder, deliberate self-harm, suicidal actions). Overall it appears that women are more likely to respond to trauma with depression than with classical PTSD as defined in DSM IV.
While men will use addictive behaviours to escape and distance themselves from the realities of their lives, women will often manifest addictive behaviours in order to maintain a relationship, to fill a void of what is missing in a relationship, or to self-medicate the pain of abuse or betrayal.
These important differences have a direct relevance for addressing addictions (or obesity) in group settings, which is why Covington made a strong case for running separate groups for men and women.
Overall, Covington made a strong case for using a trauma-informed gender-responsive intervention for women in addiction treatments. Thus, in a paper published in the Journal of Psychoactive Drugs back in 2008, Covington and colleagues found that applying manualised programs (Helping Women Recover and Beyond Trauma), founded on research and clinical practice and grounded in the theories of addiction, trauma, and women’s psychological development, resulted in significantly less substance use, less depression, and fewer trauma symptoms, including anxiety, sleep disturbances, and dissociation.
Covington also notes that the way that women look at the classical 12-steps approach to dealing with addictions, is very different from how men approach the 12-steps. These differences are nicely summarised in Covington’s book A Woman’s Way Through The Twelve Steps.
All of this not only reconfirms my own views on the close links between trauma, addictions and obesity but also made me realise that anyone working with obese clients must be well versed in assessing trauma history, addictions and understanding these powerful emotional and neurobiological influences on ingestive behaviour.
On a closing note, Covington recommended that when working in a setting where there are likely to be many trauma patients, it may be important to do a walk-thru to ensure that the physical environment of the clinic does not have subtle triggers of traumatic memories.
Simply prescribing a diet plan to someone who is using food as a coping strategy is neither useful nor respectful. Relating back to my post yesterday on the secondary prevention of obesity, I sincerely believe that addressing mental health and addictions will be an important part of the solution.
I, for my part, will certainly be paying more attention to the literature on trauma and addictions from now on.
AMS
Banff, Alberta
Covington SS, Burke C, Keaton S, & Norcott C (2008). Evaluation of a trauma-informed and gender-responsive intervention for women in drug treatment. Journal of psychoactive drugs, Suppl 5, 387-98 PMID: 19248396
Women Are Fat – Men Are Just Big And Strong?
 Being overweight or obese has been associated with a poor body image and a lower quality of life specially in females, but the impact on males is less clear.
Being overweight or obese has been associated with a poor body image and a lower quality of life specially in females, but the impact on males is less clear.
This relationship was now examined by Saloumi and Plourde from McGill University, Montreal, in a paper just published in Psychology, Health & Medicine.
The analysis was based on data from the nationally representative Canadian Community Health Survey, which included 25,246 males and females aged 15-29 years.
As expected, both satisfaction with their looks and satisfaction with life were inversely associated with excess weight in females.
In contrast, excess weight in older men was associated with greater satisfaction with life (body image in men was not examined).
While older overweight men were less likely to smoke, excess weight was associated with higher rates of smoking, particularly in younger women.
Both men and women with excess weight reported avoiding food because of caloric content and an attempt to control their weight.
Although most males and females with excess weight acknowledged the fact that they were overweight, 20.4, 29.6, and 36.1% of males with excess weight in the age group of 15-19, 20-24, and 25-29, respectively, seemed to think that their weight is “just about right”.
In contrast less than 10% of females with excess weight in all three age groups thought that their weight is “just about right”.
The study points to important differences in how young men and women perceive their excess weight and the strategies that they may adopt to control it.
The authors explain their interesting finding that overweight men appear more satisfied with life than do overweight women with the notion that while men associate excess weight with being “big and strong”, women tend to associate excess weight with being “fat”, something both sexes appear to fear.
Previous researchers have also suggested that while men may avoid high-caloric foods for health reasons, women tend to do so primarily to control their weight.
These differences have important implications both for public health messaging as well as for individual counseling of men and women with excess weight.
I am guessing that distinctly different strategies will be needed to address excess weight in men and women.
I look forward to any ideas my readers may have on how to better convince men that some of that “big and strong” may actually be a significant health risk.
AMS
Edmonton, Alberta
p.s. Join my new Facebook page for more posts and links on obesity prevention and management
Saloumi C, & Plourde H (2010). Differences in psychological correlates of excess weight between adolescents and young adults in Canada. Psychology, health & medicine, 15 (3), 314-25 PMID: 20480435


