Obesity Network Joins Incontinence Coalition
 As blogged before, urinary incontinence is a common problem in women with excess weight, which often responds well to weight loss.
As blogged before, urinary incontinence is a common problem in women with excess weight, which often responds well to weight loss.
Unfortunately, however, this problem is seldom talked about and people with incontinence face many problems including substantial costs for supplies that are not generally covered by health care.
Yesterday, the Canadian Obesity Network and several other organisations called upon governments to pay more attention to the needs of people with this unfortunate health problem.
The text of the press release is as follows:
TORONTO, April 27 /CNW/ – Members of The Incontinence Coalition endorsed a letter to Federal and Provincial Ministers of Health urging greater recognition of the prevalent and chronic condition of incontinence. Incontinence affects more than 3 million Canadians and is a chronic condition
that carries an enormous stigma.
The newly formed Incontinence Coalition is made up of respected and well-known organizations that represent the voice of many Canadians affected by the condition. These groups include the Canadian Continence Foundation, Canadian Obesity Network, Canadian Paraplegic Association (Ontario), Canadian Prostate Cancer Network, CARP, Easter Seals Canada and the Spina Bifida and Hydrocephalus Association of Ontario.
“Incontinence can impact all parts of a person’s life: their social interactions, their sex life, their ability to work, travel, play sports, and participate in community life,” stated Jacqueline Cahill, Executive Director of the Canadian Continence Foundation. “It can be an emotionally devastating condition that causes social isolation, low self-esteem, depression, and a fear of intimacy.”
“Canadians living with incontinence usually endure the condition in silence because of the stigma attached. Many are too embarrassed to seek treatment,” said Derek Lawrence, Director of the Canadian Prostate Cancer Network.
To help de-stigmatize the condition and improve access to care, the Incontinence Coalition encouraged Federal and Provincial Ministers of Health to:
– Publicly Acknowledge the Condition. There is a need to publicly acknowledge the prevalence of the condition and the need for treatment. This will help normalize and de-stigmatize the condition.
– Improve public education and awareness. There is a need for the government to take a pro-active role in promoting awareness and education of this condition to the public.
– Improve access to treatments, including medications; absorbent products (for community dwelling individuals and those in Long Term Care facilities); surgical treatments and catheters.
– Increase the emphasis on incontinence education for general practitioners. GPs must become more knowledgeable and proactively bring up the subject with their older patients.
– Ensure access to trained nurses and other supportive care-givers. Nurses and nurse practitioners who are trained in continence care are needed to help provide support for those individuals living with incontinence in the community and their caregivers.
– Fund Continence Care Clinics These clinics will provide assessment, management, education and referral for people living with incontinence.
“It is important for the Government to publicly acknowledge the prevalence of incontinence and the need for treatment,” stated Holly Vengroff, Vice President at CARP.
Members of the public are encouraged to contact their MPs to voice their support for the Coalition and its recommendations.
For further information: Media Contact: Jacqueline Cahill, Executive Director, Canadian Continence Foundation, jcahill@continence-fdn.ca, (705) 931-4488
AMS
Edmonton, Alberta
Weight Loss for Urinary Incontinence
 Urinary incontinence affects millions of women and has a profound adverse effect on quality of life. Overweight and obesity are well known to make symptoms of incontinence worse and there is preliminary evidence suggesting that weight loss has a beneficial effect on symptoms in overweight and obese women.
Urinary incontinence affects millions of women and has a profound adverse effect on quality of life. Overweight and obesity are well known to make symptoms of incontinence worse and there is preliminary evidence suggesting that weight loss has a beneficial effect on symptoms in overweight and obese women.
Last week the N Engl J Med published the results of the PRIDE study (Program to Reduce Incontinence by Diet and Exercise), a large randomized trial in 338 overweight and obese women with at least 10 urinary-incontinence episodes per week. Patients were randomized to an intensive 6-month weight-loss program that included diet, exercise, and behavior modification (226 patients) or to a structured education program (112 patients).
The average age of the patients was around 53 years, the average BMI was 36; the weekly number of incontinence episodes was around 24/week. After six months, women in the intervention group had a mean weight loss of 8.0% (7.8 kg), as compared with 1.6% (1.5 kg) in the control group. The number of incontinence episodes decreased by 47% in the intervention group, as compared with 28% in the control group. The reduction was mainly seen in the frequency of stress-incontinence, but not of urge-incontinence episodes.
These findings suggest that urinary incontinence should be added to the long list of health problems that improve with moderate weight loss.
Obesity Can Make you Pee Your Pants
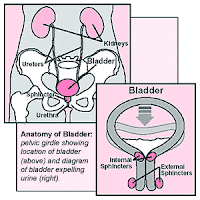 Not a very pleasant picture: wetting your pants every time you laugh, sneeze, lift a heavy load, exercise, drink too much coffee – the medical term for this common but rarely talked about problem is urinary incontinence.
Not a very pleasant picture: wetting your pants every time you laugh, sneeze, lift a heavy load, exercise, drink too much coffee – the medical term for this common but rarely talked about problem is urinary incontinence.
For anatomical reasons, this problem (the involuntary leakage of urine) is largely limited to women.
Experts essentially speak of three common types of incontinence (there are others):
1) Stress incontinence: loss of small amounts of urine with coughing, laughing, sneezing, exercising or other movements that increase intraabdominal pressure and thus increase pressure on the bladder.
2) Urge incontinence: involuntary loss of urine often due to (nervous) overactivity of the bladder resulting in the sudden need or urge to urinate, sometimes after drinking a glass of water or even hearing the sound of running water.
3) Mixed incontinence: as the name says – when aspects of both forms of incontinence are present.
Obesity can not only increase the risk for urinary incontinence but also makes it worse in people who have it for other reasons (e.g. after childbirth).
So how strong is the link between urinary incontinence and obesity?
This was the question asked by Townsend and colleagues from Harvard in a recent article pulbished in OBESITY.
The researchers examined the associations of BMI and waist circumference with new-onset urinary incontinence among women aged 54-79 years in the Nurses’ Health Study. From 2000 to 2002, they identified 6,790 women who reported at least monthly episodes of incontinence among 35,754 women reporting no UI in 2000. They also looked at the type of incontinence in individuals who had at least weekly incontinence.
There were highly significant trends of increasing risk of urinary incontinence with increasing BMI and waist circumferenc. Women with a BMI>35 were around 70% more likely to have incontinence compared to women with BMI 21-22.9.
Interestingly, while BMI was associated with urge and mixed, but not stress incontinence, waist circumference was associated only with stress urinary incontinence.
Fortunately, urinary incontinence is a very treatable condition, whereby, when present, obesity treatment can have a significant benefit.
As I have noted before – obesity affects virtually every organ system. The distress of having obesity-related urinary incontinence can far outweigh the “inconvenience” of having high blood pressure or dyslipidemia.
Always important to remember, obesity is not just about the heart!
AMS
Edmonton, Alberta


