Sleep Apnea Increases in the US Population
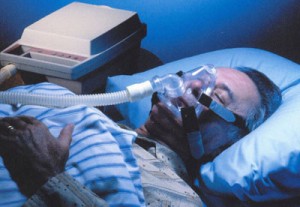 To anyone involved in bariatric care, screening for sleep apnea should be an essential part of clinical assessment. Thus, not surprisingly, a substantial proportion of bariatric patients are diagnosed with this condition and receive (often life-changing) therapy.
To anyone involved in bariatric care, screening for sleep apnea should be an essential part of clinical assessment. Thus, not surprisingly, a substantial proportion of bariatric patients are diagnosed with this condition and receive (often life-changing) therapy.
But how common is this condition in the overall population?
This question is addressed in a paper by Peppard and colleagues published in the American Journal of Epidemiology.
Based on data in bout 1,500 participants from the Wisconsin Sleep Cohort Study, an ongoing community-based study established in 1988 with participants randomly selected from an employed population of Wisconsin adults, prevalence of sleep-disordered breathing in the United States for the periods of 1988-1994 and 2007-2010 was estimated using NHANES data for age, sex, and body mass index.
Based on these estimates, the current prevalence of moderate to severe sleep-disordered breathing (apnea-hypopnea index, measured as events/hour, ≥15) in the US are 10% among 30-49-year-old men; 17% among 50-70-year-old men; 3% among 30-49-year-old women; and 9% among 50-70 year-old women.
Not only do these estimated prevalence rates represent a substantial increase over the last 2 decades but, as expected even higher rates of sleep apnea are seen in the more obese section of the population.
Thus, sleep apnea is certainly a condition that will require a lot of attention both in terms of diagnostics and management.
AMS
Edmonton, Alberta
![]() Peppard PE, Young T, Barnet JH, Palta M, Hagen EW, & Hla KM (2013). Increased Prevalence of Sleep-Disordered Breathing in Adults. American journal of epidemiology PMID: 23589584
Peppard PE, Young T, Barnet JH, Palta M, Hagen EW, & Hla KM (2013). Increased Prevalence of Sleep-Disordered Breathing in Adults. American journal of epidemiology PMID: 23589584
.
Perioperative Management of Obesity Hypoventilation Syndrome
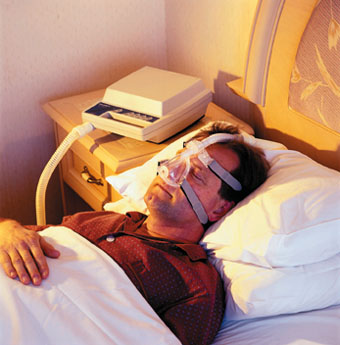 One of the major mechanical complications associated with severe obesity is the obesity hypoventilation syndrome – sometimes referred to as “Pickwickian Syndrome” in allusion to Joe, the rather stout kid in Charles Dickens’ Pickwick Papers.
One of the major mechanical complications associated with severe obesity is the obesity hypoventilation syndrome – sometimes referred to as “Pickwickian Syndrome” in allusion to Joe, the rather stout kid in Charles Dickens’ Pickwick Papers.
A paper by Edmond Chau and colleagues from the University of Toronto, published in Anaesthesiology, reviews the epidemiology, pathophysiology, and perioperative considerations of this syndrome.
The obesity hypoventilation syndrome (OHS) is defined by
“the triad of obesity, daytime hypoventilation, and sleep-disordered breathing without an alternative neuromuscular, mechanical, or metabolic cause of hypoventilation. It is a disease entity distinct from simple obesity and obstructive sleep apnea.”
As the authors point out,
“OHS is often undiagnosed but its prevalence is estimated to be 10-20% in obese patients with obstructive sleep apnea and 0.15-0.3% in the general adult population.”
Patients present with hypercapnia (which, in part explains the extreme drowsiness) resulting from severe upper airway obstruction, restrictive chest physiology, blunted central respiratory drive, and pulmonary hypertension.
Not surprisingly, it is associated with a vastly increased risk of mortality.
The mainstay of conservative therapy is noninvasive positive airway pressure, which can markedly reduce the symptoms and quite possibly reduce overall risk.
The most effective treatment, however, is bariatric surgery, where weight loss is accompanied by often dramatic improvement in pulmonary function.
However, operating on patients with severe OHS also has its risks.
Perioperative management begins by having a high level of suspicion as this syndrome is often undiagnosed.
The definitive test for hypoventilation is an arterial blood gas performed on room air during wakefulness.
Patients may also have increased serum bicarbonate level due to metabolic compensation of chronic respiratory acidosis. A serum HCO3- threshold of 27 mEq/L demonstrated a 92% sensitivity in predicting hypercapnia on arterial blood gas. Together with an elevated apnea-hypopnea index (AHI), elevated serum HCO3 has a specificity of 95% with a sensitivity of 100%.
In addition, hypoxemia (SpO2 <90%, corresponding to PaO2 < 60 mmHg)99 during wakefulness should lead clinicians to suspect OHS in patients with OSA.
Thus, the authors recommend that all patients presenting with a high BMI and AHI should be screened for OHS, serum HCO3- level being the easiest test for hypercapnia before elective surgery.
Once hypercapnia is confirmed with an arterial blood gases, referral to sleep medicine and further testing, such as pulmonary function testing, chest imaging, thyroid-stimulating hormone, and clinical assessment of neuromuscular strength, is recommended to rule out other important causes of hypoventilation.
The article goes on to make specific recommendations for pre-, intra- and post-operative management of patients with OHS – something perhaps all health professionals dealing with severely obese patients should be aware of.
AMS
Edmonton, Alberta
![]() Chau EH, Lam D, Wong J, Mokhlesi B, & Chung F (2012). Obesity hypoventilation syndrome: a review of epidemiology, pathophysiology, and perioperative considerations. Anesthesiology, 117 (1), 188-205 PMID: 22614131
Chau EH, Lam D, Wong J, Mokhlesi B, & Chung F (2012). Obesity hypoventilation syndrome: a review of epidemiology, pathophysiology, and perioperative considerations. Anesthesiology, 117 (1), 188-205 PMID: 22614131
Sleep Apnea Limits Response to Obesity Interventions
 In follow up to yesterday’s post on the positive impact of CPAP treatment for obstructive sleep apnea (OSA) on weight and cardiometabolic risk factors, here is another study highlighting the importance of diagnosing and managing OSA in obesity patients.
In follow up to yesterday’s post on the positive impact of CPAP treatment for obstructive sleep apnea (OSA) on weight and cardiometabolic risk factors, here is another study highlighting the importance of diagnosing and managing OSA in obesity patients.
This study by Anne-Laure Borel and colleagues from the Institut universitaire de cardiologie et de pneumologie de Québec, Québec, Canada, published in THORAX, the researchers show that OSA attenuates the effects of a lifestyle intervention programme in men with visceral obesity.
The authors compare the response of 77 men, selected on the basis of increased waist circumference (≥90 cm) and dyslipidaemia (triglycerides ≥1.69 and/or high-density lipoprotein (HDL) cholesterol <1.03 mmol/litre) to a 1-year healthy eating, physical activity/exercise intervention programme.
After the 1-year lifestyle intervention, despite similar compliance to the programme, the 28 men with sleep apnoea syndrome at baseline (ODI ≥10 events/h) showed smaller reductions in body mass index, waist circumference, triglycerides and smaller increases in HDL cholesterol and adiponectin than the 49 men without sleep apnoea.
In addition, the higher the baseline ODI and the time spent under 90% oxygen saturation, the lower the reductions in fat mass and visceral adiposity, and the smaller the improvement in glucose/insulin homeostasis indices after 1 year.
This finding certainly supports the notion that diagnosis and management of OSA has to be seen as an essential part of obesity management.
Here again (according to Helpguide) are the most common symptoms associated with sleep apnea:
Major signs and symptoms of sleep apnea
- Loud and chronic snoring
- Choking, snorting, or gasping during sleep
- Long pauses in breathing
- Daytime sleepiness, no matter how much time you spend in bed
Other common signs and symptoms of sleep apnea include:
- Waking up with a dry mouth or sore throat
- Morning headaches
- Restless or fitful sleep
- Insomnia or nighttime awakenings
- Going to the bathroom frequently during the night
- Waking up feeling out of breath
- Forgetfulness and difficulty concentrating
- Moodiness, irritability, or depression
Signs and symptoms of sleep apnea in children
While obstructive sleep apnea can be common in children, it’s not always easy to recognize. In addition to continuous loud snoring, children with sleep apnea may adopt strange sleeping positions and suffer from bedwetting, excessive perspiration at night, or night terrors. Children with sleep apnea may also exhibit changes in their daytime behavior, such as:
- Hyperactivity or inattention
- Developmental and growth problems
- Decrease in school performance
- Irritable, angry, or hostile behavior
- Breathing through mouth instead of nose
Edmonton, Alberta
![]() Borel AL, Leblanc X, Alméras N, Tremblay A, Bergeron J, Poirier P, Després JP, & Series F (2012). Sleep apnoea attenuates the effects of a lifestyle intervention programme in men with visceral obesity. Thorax PMID: 22396182
Borel AL, Leblanc X, Alméras N, Tremblay A, Bergeron J, Poirier P, Després JP, & Series F (2012). Sleep apnoea attenuates the effects of a lifestyle intervention programme in men with visceral obesity. Thorax PMID: 22396182
.
CPAP Lowers Body Weight and Improves Metabolic Syndrome in Patients With Sleep Apnea
 Regular readers will be well aware of the rather strong association between obstructive sleep apnea (OSA) and excess weight. This is often a two-way street, with OSA leading to poor sleep and sleep cycle disruption, which in turn can affect daytime activity levels and (most likely) eating behaviour. In addition, the intermittent hypoxia associated with OSA has been implicated in hypertension and poor metabolic control.
Regular readers will be well aware of the rather strong association between obstructive sleep apnea (OSA) and excess weight. This is often a two-way street, with OSA leading to poor sleep and sleep cycle disruption, which in turn can affect daytime activity levels and (most likely) eating behaviour. In addition, the intermittent hypoxia associated with OSA has been implicated in hypertension and poor metabolic control.
A recent study by Surendra Sharma (no relation) from the All India Institute of Medical Sciences, New Delhi India, published in the New England Journal of Medicine, demonstrates the positive impact of treating OSA with CPAP on body weight and metabolic syndrome.
Sharma and colleagues, studied 86 patients, 75 (87%) of whom had the metabolic syndrome, in a double-blind, placebo-controlled trial, in which they randomly assigned patients with OSA to 3 months of therapeutic CPAP followed by 3 months of sham CPAP, or vice versa, with a washout period of 1 month in between.
CPAP treatment (vs. sham CPAP) was associated with small but significant mean decreases in blood pressure, cholesterol and triglyceride levels, as well as Hba1C levels.
Metabolic syndrome status was reversed in 13% under CPAP vs. 1% under sham treatment.
I was quite interested in seeing that there was also a small, but statistically significant reduction in body weight, BMI, and waist circumference.
Thus, as the authors note,
“We demonstrated a significant decrease in BMI and abdominal fat, by using CT, in association with CPAP therapy. These findings could be secondary to a decrease in daytime somnolence and a consequent increase in physical activity after CPAP use at night.”
Moreover,
“Weight loss could also be a mechanism for improvement in components of the metabolic syndrome in this study, as suggested by the correlation of the metabolic syndrome with a change in BMI. However, baseline BMI was not a determinant of response to therapy.”
The latter finding comes as no surprise given that there is a rather poor relationship between BMI and cardiometabolic risk factors (which is exactly why we came up with the Edmonton Obesity Staging System).
Overall, the findings certainly support the notion that patients presenting with excess weight and cardiometabolic risk factors should be routinely screened for OSA and that they stand to substantially benefit from its treatment.
AMS
Edmonton, Alberta
![]() Sharma SK, Agrawal S, Damodaran D, Sreenivas V, Kadhiravan T, Lakshmy R, Jagia P, & Kumar A (2011). CPAP for the metabolic syndrome in patients with obstructive sleep apnea. The New England journal of medicine, 365 (24), 2277-86 PMID: 22168642
Sharma SK, Agrawal S, Damodaran D, Sreenivas V, Kadhiravan T, Lakshmy R, Jagia P, & Kumar A (2011). CPAP for the metabolic syndrome in patients with obstructive sleep apnea. The New England journal of medicine, 365 (24), 2277-86 PMID: 22168642
.
How Lack of Sleep Makes You Gain Weight
 Regular readers of these pages will recall numerous posts on the profound effect of sleep deprivation on appetite and metabolism – a factor, believed by many, to be a major driver of the obesity epidemic (and not just in kids!).
Regular readers of these pages will recall numerous posts on the profound effect of sleep deprivation on appetite and metabolism – a factor, believed by many, to be a major driver of the obesity epidemic (and not just in kids!).
Although epidemiological studies on sleep leave much to be desired both in quality and representativeness, current estimates suggest that we may be sleeping around two hours less than in the 60s.
Add to this the increase in night work, extended exposure to artificial light, and a increased eating in the late evening and night hours, and it is not hard to see how these changes would have affected our natural biology.
Enough reason for last month’s issue of Best Practices & Research Endocrinology and Metabolism to be entirely dedicated to the topic of Sleep and Metabolism.
As pointed out in the preface by Eve van Cauter and David Ehrmann from the University of Chicago, independent observations linking metabolism, sleep and circadian function include the idenfication of the orexin system which links the control of wakefulness with eating behavior, the identification of the circadian ‘Clock’ gene as conferring an increased risk of obesity and diabetes and the “sleep debt study” which showed that short term sleep restriction in healthy young adults results in decreased glucose tolerance (see previous blog entries on all of these landmark studies).
The special issue attempts to provide a comprehensive overview of this exciting field with contributions spanning from the molecular circuitry of hypothalamic pathways linking sleep and metabolism to the clinical relevance of sleep for nocturnal hypoglycemia in diabetic patients.
Readers may particularly be interested in the following articles in this issue:
Role of sleep duration in the regulation of glucose metabolism and appetite (Lisa Morselli et al.)
Sleep duration and cardiometabolic risk: A review of the epidemiologic evidence (Kristen L. Knutson)
Bariatric surgery and its impact on sleep architecture, sleep-disordered breathing, and metabolism (Silvana Pannain & Babak Mokhlesi)
The impact of sleep disturbances on adipocyte function and lipid metabolism (Josiane Broussard & Matthew J. Brady)
Sleep loss and inflammation (Janet M. Mullington, et al.)
Circadian disruption and metabolic disease: Findings from animal models (Deanna Marie Arble, et al.)
Sleep and the response to hypoglycaemia (Kamila Jauch-Chara & Bernd Schultes)
Sleep and metabolism: Role of hypothalamic neuronal circuitry (Asya Rolls, et. al.)
New evidence for a role of melatonin in glucose regulation (Elmar Peschke & Eckhard Mühlbauer)
Metabolic consequences of intermittent hypoxia: Relevance to obstructive sleep apnea (Luciano F. Drager, et al.)
I can only concur with the hopes of the editors that,
“… this volume will offer a thought provoking overview of this new area of investigation and inspire novel lines of research on the intriguing links between sleep, circadian function and metabolism and their impact on the health and well-being of billions of individuals in modern society.”
AMS
Acapulco, Mexico
Van Cauter E, & Ehrmann DA (2010). Preface. Best practice & research. Clinical endocrinology & metabolism, 24 (5) PMID: 21112018


