Readiness To Do The Right Thing?
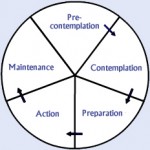 One of the most pervasive behavioural modification paradigms is Prochaska and DiClemente’s stages of change: precontemplation, contemplation, preparation, action, and maintenance.
One of the most pervasive behavioural modification paradigms is Prochaska and DiClemente’s stages of change: precontemplation, contemplation, preparation, action, and maintenance.
It is therefore not surprising, that the recent Scientific Statement on New and Emerging Weight Management Strategies for Busy Ambulatory Settings From the American Heart Association, recommends the use of this paradigm in obesity management.
As the Statement points out:
“…providers should ask whether they want to lose weight and whether they believe they are ready to make changes to promote weight loss.”
The statement describes the use of a simple 5-item questionnaire, used in a descriptive study in a primary care setting, in which patients were asked to choose which of 5 statements best described their readiness for weight loss:
“I have not really thought about it” (pre-contemplation)
“I mean to lose weight but I don’t actually get around to it” (contemplation)
“From time to time, I go on a diet/exercise, but then I stop after a few days” (preparation)
“I have been working on losing weight for the past 6 months” (action)
“I have been working on losing weight for over 6 months, or I have kept my weight I lost off for over 6 months” (maintenance)
According to this study,
“Patients who were in the latter 4 stages of readiness were more likely to recall having received counseling for weight loss than those in the precontemplation stage.”
Based on this and similar studies, the Statement goes on to suggest
“…that although assessing readiness to change adds an extra step in caring for overweight and obese adults, it is a useful indicator of whether any accompanying weight loss counseling will be recalled by the patient. A patient who at least recalls weight loss counseling is better equipped to take steps toward weight loss than one who does not.”
While there is certainly nothing wrong with the ‘Readiness for Change’ paradigm in that someone in the ‘pre-contemplation’ or ‘contemplation’ stage may not be ready to embark on weight management, I often encounter patients, who are more than ready and are already ‘preparing’ or even ‘acting’, but just not preparing for or doing the right thing.
So for e.g., it is not uncommon at all, to meet patients ready to ‘lose weight’ and anxious to follow a diet or exercise plan but completely unready to actually deal with the underlying psychological or other issues that would really need to be tackled for any chance at keeping the weight off.
We see patients ready to exercise but not ready to give up their daily supply of pop, patients ready to eat more fruit and vegetables but not ready to have breakfast, patients ready to join a commercial weight loss program but not ready to tackle their abusive marriage, patients ready to go on a low-calorie diet but not ready to consider treatment for their depression.
These are patients, who are ‘ready’ to do the wrong thing but far from ready to do what is really necessary.
So being ‘ready’ alone is hardly a measure or predictor of ‘success’.
I am also not comfortable with how the ‘Readiness for Change’ model is presented in this Statement, as the focus is clearly on weight-loss, which, I cannot emphasize enough, IS NOT A BEHAVIOUR!
To be useful as a behavioural change model, the focus should be on changing a behaviour (keeping a food diary, turning off my lights at 10 pm, adding 20 mins of relaxation exercises to my daily routine, etc.).
A key challenge for health professionals, thus, is not just helping clients across the Stages of Change, but also, ensuring that their readiness is indeed focussed on doing the right thing – this, of course, is easier said than done.
AMS
Edmonton, Alberta
Rao G, Burke LE, Spring BJ, Ewing LJ, Turk M, Lichtenstein AH, Cornier MA, Spence JD, Coons M, & on behalf of the American Heart Association Obesity Committee of the Council on Nutrition, Physical Activity and Metabolism, Council on Clinical Cardiology, Council on Cardiovascular Nursing, Council on the Kidney in Cardiovascular Disease, and Stroke Cou (2011). New and Emerging Weight Management Strategies for Busy Ambulatory Settings: A Scientific Statement From the American Heart Association * Endorsed by the Society of Behavioral Medicine. Circulation, 124 (10), 1182-1203 PMID: 21824925
Household Intervention Changes Behaviour But Not Body Weight
 When it comes to weight management (especially in kids), the consensus appears to be that lifestyle changes are easier to implement and more effective when they target whole households.
When it comes to weight management (especially in kids), the consensus appears to be that lifestyle changes are easier to implement and more effective when they target whole households.
But do household interventions really change behaviour?
This question was now addressed by Simone French and colleagues from the University of Minnesota in a paper just published online in OBESITY.
In this one-year study, the researchers randomised 99 households an intervention consisting of six face-to-face group sessions, placement of a TV-locking device on all home TVs, and home-based intervention activities, or to a control group.
While the interventions households did not report any changes in the frequency of meals eaten at fast food restaurants, or intake of fruits and vegetables or sugar-sweetened beverages, there were significant (albeit modest) reductions in frequency of consumption of sweets and snack foods and in dollars spent eating out.
TV viewing decreased by about 30 mins per day in intervention households with significant reductions reported during meals.
Adults in intervention households reported walking around 10 extra minutes per day and about 15 extra minutes of moderate/vigorous physical activity per day. No changes in physical activities were seen in adolescents.
Weekly self-weight increased from 50 to 70%.
As would perhaps be expected from these rather modest effects on lifestyle, no changes in body weight were noted.
Thus, as the authors point out, targeting households can improve some health-related behaviours, however, the duration of the intervention and follow-up may be too short to say whether these changes (if maintained) will in the end lead to prevention of weight loss.
Thus, while the study supports the idea of targeting households for behaviour change, it also reminds us that healthier behaviours alone do not necessarily translate into weight loss.
As often in these type of studies, the authors fail to mention the actual cost of the intervention or the likelihood of such interventions being feasible and effective outside the context of a research trial.
Certainly, most readers will appreciate that it probably takes more to lose and maintain a lower body weight than to simply eat healthier and watch less TV.
But then again, who ever said that weight alone was a good measure of health?
AMS
Edmonton, Alberta
French SA, Gerlach AF, Mitchell NR, Hannan PJ, & Welsh EM (2011). Household Obesity Prevention: Take Action-a Group-Randomized Trial. Obesity (Silver Spring, Md.) PMID: 21212771
Traditional Family Routines Reduce Childhood Obesity?
 So, as Michelle Obama yesterday announced her childhood obesity initiative, another piece of news on childhood obesity crowded the news wires.
So, as Michelle Obama yesterday announced her childhood obesity initiative, another piece of news on childhood obesity crowded the news wires.
This was a study by Sarah Anderson (Ohio State) and Robert Whitaker (Temple) published as an early release in Pediatrics.
The researchers performed a cross-sectional analysis of a nationally representative sample of 8550 four-year-old US children who were assessed in 2005 in the Early Childhood Longitudinal Study.
The study focussed on the relationship between obesity and three household routines: regularly eating the evening meal as a family (>5 nights per week); obtaining adequate nighttime sleep on weekdays (10.5 hours per night); and having limited screen-viewing (television, video, digital video disk) time on weekdays (2 hours/day).
Analyses were adjusted for the child’s race/ethnicity, maternal obesity, maternal education, household income, and living in a single-parent household.
While the prevalence of obesity was 14.3% among children exposed to all 3 routines (14.5% of the sample), it was 24.5% among those exposed to none of the routines (12.4%).
The odds of obesity associated with exposure to all 3, any 2, or only 1 routine (compared with none) were 0.63, 0.64, and 0.84, respectively.
So if you do have kids ask yourself:
1) Do we regularly sit down for supper as a family?
2) Do my kids regularly get at least 10.5 hrs of sleep?
3) Do my kids have less than 2 hrs of screen time on weekdays?
A “no” to all of the above, probably puts your kids in the high-risk category, a “yes” to all of the above, and your kids are probably doing fine.
Now comes the tough part, i.e. wether or not, if you are not doing all of the above, simply doing these three things will actually change your kids risk for obesity. Or in other words, if you did nothing else, except sit down for dinner, have the kids in bed by 8.30, and limit their screen time, would your kids actually have healthy weights?
I am guessing that it will take far more than that. In fact I would not at all be surprised if the families that do any of the above were probably quite different from the families that don’t. I would indeed expect that these families are different in so many ways that really, these three factors are probably just “markers” rather than the actual explanation for the lower obesity risk.
Indeed, if you did have the time and parenting skills to ensure that your whole family sits down for supper, your kids don’t watch too much TV, and are off to bed at bedtime, then you are probably also doing a lot of other things right.
On the other hand, if your family meals are chaotic, you have no control over your kids’ screen time, and they are still running around at midnight, there are probably other issues that need to be addressed.
So while the findings are interesting (and by no means surprising), I am not exactly sure how they will help us address the childhood epidemic.
Perhaps a well-designed intervention study will show wether or not simply adopting these three “routines” will actually make a difference.
I certainly appreciate any comments or opinions on whether or not any of my readers think this will work.
AMS
Hamburg, Germany
US College Promotes Weight Bias and Discrimination?
 What is not shocking is that according to a report on CNN, a US college (Lincoln University, Pennsylvania) has mandated a fitness course that its students have to pass in order to get their degree.
What is not shocking is that according to a report on CNN, a US college (Lincoln University, Pennsylvania) has mandated a fitness course that its students have to pass in order to get their degree.
What is shocking, however, is that only students with a BMI greater than 30, who fail to lose weight during their time at that school are required to take and pass this course.
The underlying assumption of course is that fat people are apparently too stupid to know about healthy eating and exercise and that requiring them to take and pass a course on this will make them drop those excess pounds and become healthy and successful human beings.
Apart from the fact that you would expect college educators to know that wasting resources on well-intended but largely useless weight interventions based solely on “healthy” eating and exercise are not an evidence-base approach to weight management (due to their rather modest effectiveness), assuming that it is even remotely possible to identify individuals in need of “lifestyle education” by simply calculating their BMI (or measuring their waist circumference), is ridiculous.
Perhaps the folks who came up with this idea are unaware of the fact that there is indeed no shortage of “thin” people frequenting fast food restaurants, living sedentary lifestyles or simply using cigarette smoking (if not other drugs), unhealthy dieting, purging, and/or excessive exercise to control their weight.
Singling out students based solely on weight for intervention is nothing else than stereotyping individuals who meet population-based BMI cuttoffs as unhealthy or unfit.
Not only is this discriminatory practice reflective of a limited understanding of the determinants of health, it is also an insult to anyone who’s BMI is greater than 30 despite trying their best to manage their excess weight in this obesogenic environment.
If excess weight is truly affecting a students’ health (and it takes more than a scale or measuring tape to determine this), I have nothing against these students being offered appropriate counseling and interventions by a licensed health professional.
Dictating “lifestyles” to people identified only by virtue of an arbitrarily defined “excess” weight is neither helpful nor supported by scientific evidence.
Perhaps, as one reader comments on the CNN website in response to the college’s response that they are less concerned about health than about the fact that obese students may be less successful in life, “the ones voted as ugly should take a beauty class as this is also related to success”.
As always, I appreciate any comments on this topic.
AMS
Frankfurt, Germany
p.s. Hat tip to Gabriela Tymowski for drawing my attention to this story
Obesity: Lifestyle Choice or Lifestyle Chance?
 Readers of these pages should by now recognize that obesity is an extraordinarily heterogeneous and complex condition.
Readers of these pages should by now recognize that obesity is an extraordinarily heterogeneous and complex condition.
While energy balance is simply a matter of energy in and energy out, the determinants of energy in and energy out are anything but simple.
Indeed, the sociopsychobiology of ingestive behaviour is perhaps the most complex of all human behaviours (not surprising given its importance for survival of the species) and the physiological, neuroendocrine and biochemical pathways that determine energy metabolism and activity thermogenesis are clearly no simpler.
It is perhaps, therefore, not all that unexpected when study after study (let alone your own experience) shows that the simplistic formula: “eat less – move more” is so disappointingly ineffective in either preventing or treating excess weight.
Yet, health professionals, decision makers and the general public continue to believe that obesity is simply a matter of “choice”, or in other words, people struggling with excess weight are simply making the wrong choices. Were they only to smarten up and chose differently, their fat would simply melt away – hopefully forever.
The fact that this “simple” formula for maintaining a healthy weight is about as realistic and effective as the “simple” formula for getting rich on the stock market by simply buying low and selling high, apparently does not deter the “healthy living missionaries” from preaching to the uninitiated, who are simply too stupid to understand that weight management is really just a matter of choosing to do the right thing!
Let us for a minute assume that “lifestyle” truly is a major determinant of weight gain (and let us simply ignore the vast body of research on genetics, imprinting, fetal programming, environmental toxins, gut bugs, adipogenic adenoviruses, activated hypothalamic-pituitary adrenal axes, mood and anxiety disorders, addictions, attention deficit, abuse, emotional neglect, poor body image, obesogenic medications and the many other well-documented causes of obesity), then the question remains how much of lifestyle is truly simply a matter of “choice”.
How many of us simply chose sedentary jobs that keep us in front of a computer all day, simply chose to live in neighbourhoods with no sidewalks, simply chose to work in jobs where we earn so little that the only food we can afford to feed our family is crap, simply chose to live so far from work that we face daily hour-long commutes that leave little time for recreational activity (let alone enough sleep), chose to work rather than stay home so we can be around to fix a healthy meal from scratch in time for when the kids come home from school, simply chose to drive a car rather than spend our money on the 5-9 daily servings of fruits and vegetables for everyone in our family, simply chose to have a TV in the house that streams endless hours of advertising to our children, simply chose to drive our kids to school rather than let them cross those five busy intersections, simply chose to live in a country where the government subsidizes corn and meat producers rather than fruit and vegetables growers, etc, etc, etc? Are all of these “lifestyle” factors simply a matter of choice? If yes, then, I am sure we can all simply chose differently and obesity will simply vanish!
But what if obesity is not simply the result of lifestyle “choice” but rather the result of lifestyle “chance”. Do we all truly have a chance to always feed our families healthy foods, have the chance to live in neighbourhoods where it is safe for our kids to walk to school and play outside, have the chance to enroll them in daily sport programs, have the chance to prevent them from ever seeing ads for unhealthy foods, have the chance to ensure that they (and we) get 8 to 9 hours of sound sleep every night, have a chance to convince our politicians to make the right food and environmental policies?
If we don’t, but rather chose to continue living in this obesogenic environment, then do we truly have a chance of not gaining weight? Remember also, that the same environment does not treat everyone fairly – some people (the mutants?) can eat all the junk food they want and stay as thin as a rake, others, despite eating as healthy as possible and despite regular exercise, just keep packing on the pounds.
When it comes to lifestyle’s impact on obesity – is it not far more often a question of CHANCE than of CHOICE?
Let us do our best to first give everyone a fair lifestyle chance and then see if we can perhaps beat the obesity epidemic after all.
AMS
Edmonton, Alberta


