The Importance of Positive Emotions: The Neurobiology of Resilience (Part 3)
 Yesterday, I discussed the importance of secure attachments in early-life for developing resilience.
Yesterday, I discussed the importance of secure attachments in early-life for developing resilience.
The second key positive predictor of resilience according to the paper by Bart Rutten and colleagues from Maastricht University, published in Acta Psychiatrica Scandinavica, is having positive emotional experiences
Having genuinely positive emotions (rather than just fewer negative emotions) has been found to predict better mental health and recovery from depression. Moreover, positive emotions have been associated with better stress tolerance.
Although there is a fair amount of heritability (h2 = 0.60), societal influences, particularly gender socialisation can be important modulators of positive emotional experience.
“Part of the fluctuation in positive emotions comes from internal (i.e. hormonal) or diurnal influences (i.e. circadian rhythm). Another part arises from interactions in daily life. Meeting up with a friend, playing tennis, or being smiled at in the supermarket are examples of experiences, which may temporarily boost levels of positive emotion. Research has shown that the tendency to use pleasant daily life experiences to boost positive emotions (positive affect reactivity) is associated with increased resilience against depressive symptoms in the future.”
Despite these fluctuations, it is perhaps noteworthy that the overall level of positive emotions (trait) appear to be stable over age with minor decreases With minor decreases in the elderly. In contrast, emotional reactivity may be slightly higher during childhood, a critical period during which caregiver and child learn to fine-tune emotional reactivity.
This emotional response may in part be influenced by genetic factors. Thus,
“A recent study on gene–environment interactions has found that levels of positive emotions of children with the short (S-) allele of the serotonin transporter gene 5-HTT [compared with the long (L-) allele] were more reactive to differences in parenting style. When raised in a warm and supportive environment, individuals with the S-allele experienced higher levels of positive emotions than individuals with the long (L-) allele. In contrast, they experienced lower levels of positive emotions than individuals with the L-allele when raised in unsupportive environments.”
Not only do individuals often learn to identify and seek pleasant activities, it also appears that those, who manage to hold on to positive emotions longer, appear to be more resilient.
Not surprisingly,
“Dopaminergic neuronal transmission in the pathway from the VTA to the NAc has been found to be involved in the responses to both natural rewards like food and sex, as well as unnatural rewards like psychotropic drugs. The conscious subjective experience of pleasure and reward likely takes place in the orbitofrontal cortex, which has reciprocal links with the mesolimbic system. Animal studies show that the catechol-O-methyl transferase (COMT) enzyme, which breaks down dopamine, is closely involved in dopamine regulation in both subcortical and prefrontal areas, and plays a major role in the dopaminergic signalling exchange between these areas….Consistent with this proposition, a recent study found that daily life reward experience increased proportionally with the number of Met alleles on the COMT Val158Met polymorphism. The Met allele encodes for a less active COMT enzyme, resulting in lower COMT activity, and, as a result, higher levels of prefrontal dopamine.”
For clinicians, these findings may have some important implications.
For one, enhancing positive experiences can improve resilience. Thus,
“A meta-analysis established that positive psychology interventions as diverse as writing gratitude letters, practising optimistic thinking, replaying positive experiences and socializing have beneficial effects on levels of depression. Another option may be to give individuals feedback on their own daily life dynamics of emotions. Through the identification of situations associated with positive emotions, people may learn to adapt their behaviour and become more resilient.”
“In addition, meditation- or mindfulness-based approaches may be a promising venue to increase positive emotions…In a randomized controlled trial, loving-kindness meditation was associated with increased levels of positive emotion, which in turn predicted reduced depressive symptoms. Another randomized controlled trial recently showed that mindfulness-based cognitive therapy (MBCT) was associated with increases not only in positive emotions but also the ability to make use of natural, moment-to-moment rewards in the environment.”
The importance of mental training such as meditation is born out by brain imaging studies.
“..functional MRI studies have shown that loving-kindness meditation regulates neural circuitries (insula, cingulate cortices, amygdala) linked to emotion, theory of mind and empathy….grey matter volumes in certain areas of the cortex and brain stem differ between novices and experienced meditators….Recently, a randomized clinical trial compared participants before and after participation in an 8-week course of mindfulness….was associated with changes in grey matter concentration in brain regions involved in learning and memory processes, emotion regulation, self-referential processing and perspective taking.”
These findings clearly demonstrate the impact of positive emotions elicited by pleasurable activities, thoughts and mindfulness can influence brain structures thereby possibly strengthening resilience.
It is easy to recall previous conversations with recreational and occupational therapists, who told me about their work with clients to help them seek out and engage in positive social and creative activities, resulting in much improved functioning and quality of life.
I would not at all be surprised if similar efforts can promote health behaviours in my obese patients, many of who struggle to find positive experiences in a world that treats them with disdain and negativity.
AMS
Edmonton, AB
![]() Rutten BP, Hammels C, Geschwind N, Menne-Lothmann C, Pishva E, Schruers K, van den Hove D, Kenis G, van Os J, & Wichers M (2013). Resilience in mental health: linking psychological and neurobiological perspectives. Acta psychiatrica Scandinavica PMID: 23488807
Rutten BP, Hammels C, Geschwind N, Menne-Lothmann C, Pishva E, Schruers K, van den Hove D, Kenis G, van Os J, & Wichers M (2013). Resilience in mental health: linking psychological and neurobiological perspectives. Acta psychiatrica Scandinavica PMID: 23488807
.
All Obese Patients Should Be Screened For ADHD
 Regular readers will recall previous posts on the association between attention deficit disorder (ADD) and obesity.
Regular readers will recall previous posts on the association between attention deficit disorder (ADD) and obesity.
As this condition significantly affects impulse control, ability to plan, perseverance, time management, and many other factors and skills essential for weight management, this relationship should be no surprise.
In our own clinical experience (as suggested in several recent publications from others), managing ADD can often be the key step to managing weight gain.
Once you start systematically screening patients for ADD in an obesity clinic, it seems to be present in a surprisingly large number – almost 20-30%.
This number is consistent with the findings of another study, this time by Bruno Palazzo Nazar and colleagues from the Federal University of Rio de Janeiro, Brazil, published in the Journal of Attention Disorders.
The study sample consisted of women seeking nonsurgical treatment of obesity at a public endocrinology hospital with an eating disorders and obesity clinic, in Rio de Janeiro.
One hundred and fify-five consecutive patients presenting in the clinic were approached for this study. Exclusion criteria included less than 5 years of schooling/inability to read and fill out forms and questionnaires; current alcohol or drug abuse, history of bipolar or psychotic disorder; current treatment with psychoactive drugs; and presence of uncontrolled clinical, neurological, or endocrine disorders, especially if they interfere with weight, appetite, and attention; and patients older than 60 years.
Based on a battery of validated questionnaires and semi-structured interviews, 28.3% of patients were diagnosed with ADD, which, in turn, was significantly correlated with more severe binge eating, bulimic behaviors, and depressive symptoms.
As the authors note, this rate of almost 30% is far higher than the expected rate of less than 5% in the general population.
In fact, given the rather rigorous exclusion criteria, the actual prevalence of ADHD in this patient set may actually be even higher.
As a clinician, I’d certainly support the notion that we should be aware of the high prevalence of ADHD in patients presenting in obesity programs. Making this diagnosis and managing this issue, may make all the difference in long-term outcomes.
AMS
Cambridge, UK
photo credit: Peter Vidrine via photo pin cc
![]() Nazar BP, Pinna CM, Suwwan R, Duchesne M, Freitas SR, Sergeant J, & Mattos P (2012). ADHD Rate in Obese Women With Binge Eating and Bulimic Behaviors From a Weight-Loss Clinic. Journal of attention disorders PMID: 22930790
Nazar BP, Pinna CM, Suwwan R, Duchesne M, Freitas SR, Sergeant J, & Mattos P (2012). ADHD Rate in Obese Women With Binge Eating and Bulimic Behaviors From a Weight-Loss Clinic. Journal of attention disorders PMID: 22930790
.
Seasonal Affective Disorder
 Today’s post is another excerpt from “Best Weight: A Practical Guide to Office-Based Weight Management“, recently published by the Canadian Obesity Network.
Today’s post is another excerpt from “Best Weight: A Practical Guide to Office-Based Weight Management“, recently published by the Canadian Obesity Network.
This guide is meant for health professionals dealing with obese clients and is NOT a self-management tool or weight-loss program. However, I assume that even general readers may find some of this material of interest.
SEASONAL AFFECTIVE DISORDER
Seasonal affective disorder (SAD) is a recurring depression with seasonal onset and remission. SAD primarily occurs in the winter months and it is postulated that the decrease in daylight hours alters circadian rhythms and affects melatonin and serotonin levels.
A number of factors distinguish SAD from major depressive disorder. Especially important here is that SAD is often associated with increased rather than decreased appetite.
There are two primary treatment modalities for SAD. Light therapy involves exposure to visible light that produces a minimum of 2,500 lux at eye level. Daily treatment duration depends on the intensity of the light: two hours a day are needed with a light emitting 2,500 lux, while 30 minutes a day is sufficient with 10,000 lux. Light therapy devices are readily available in specialty health-care stores and on the Internet. SAD can also be treated with pharmacotherapy using antidepressants in the same way one would treat non-seasonal depression.
To date, no study has demonstrated additional benefit from combining light therapy and pharmacotherapy.
© Copyright 2010 by Dr. Arya M. Sharma and Dr. Yoni Freedhoff. All rights reserved.
The opinions in this book are those of the authors and do not represent those of the Canadian Obesity Network.
Members of the Canadian Obesity Network can download Best Weight for free.
Best Weight is also available at Amazon and Barnes & Nobles (part of the proceeds from all sales go to support the Canadian Obesity Network)
If you have already read Best Weight, please take a few minutes to leave a review on the Amazon or Barnes & Nobles website.
Will Losing Weight Make You Less Depressed?
 Regular readers will appreciate the importance of mood as a driver of ingestive behaviour. While typically depression is associated with a loss of appetite, atypical depression can lead to increased cravings for “comfort” foods, especially those high in sugar and fat.
Regular readers will appreciate the importance of mood as a driver of ingestive behaviour. While typically depression is associated with a loss of appetite, atypical depression can lead to increased cravings for “comfort” foods, especially those high in sugar and fat.
Depression is also well recognized as a major barrier to weight loss in that individuals with depression will appear less motivated, report lower energy levels, and have poor sleep patterns, all of which can in turn affect diet and physical activity.
So while depression can clearly drive weight gain and make weight management more challenging, a question often asked is whether weight loss will actually improve mood.
This question was now addressed by Anthony Fabricatore and colleagues from the University of Pennsylvania in a paper just published in the International Journal of Obesity.
The authors conducted a comprehensive meta-analyses of over 5971 articles, including 394 randomized controlled trials, regarding the relationship between weight loss and depression.
Thirty-one studies, in almost 8000 participants were included in the final analysis.
Comprehensive lifestyle modification was found to be superior for reducing symptoms of depression than control and non-dieting interventions.
Lifestyle modification was also marginally better in improving mood than dietary counseling or exercise-alone programs.
Of particular note (given my recent post on the nutritive benefits of exercise), exercise-alone programs were superior to control interventsions in reducing symptoms of depression.
Nearly all active interventions improved depression but there was no relationship between the amount of weight lost and the reduction in depression symptoms.
Health at every size (HAES) enthusiasts will likely argue that the improvement in mood has more to do with the active interventions (which include eating healthier and increasing physical activity) than with the actual weight lost – something that would be hard to argue with given that the amount of weight lost appears to have little impact on the actual improvement in mood.
Thus, rather than concluding that weight loss leads to an improvement in mood, it would perhaps be more accurate to conclude that lifestyle modifications AIMED at weight loss ALSO, on average, tend to improve mood.
This of course would not be hard to believe given the evidence that both dietary intake of certain (unhealthy) nutrients as well as increased physical activity can significantly decrease symptoms of depression.
Certainly, this study does not change my opinion that in many patients mood disorders need to be identified and addressed as a “root cause” of weight gain and that weight loss, without lifestyle change, is unlikely to improve mood.
Clearly the notion held by many of my patients, that they would be so much less depressed if only they could lose some weight, is not borne out by this data – rather I would suggest to them that a healthier lifestyle will probably improve their mood irrespective of whether or not they actually lose weight.
But of course, as always, I defer the last word on this to my readers…
AMS
Edmonton, Alberta
Fabricatore AN, Wadden TA, Higginbotham AJ, Faulconbridge LF, Nguyen AM, Heymsfield SB, & Faith MS (2011). Intentional weight loss and changes in symptoms of depression: a systematic review and meta-analysis. International journal of obesity (2005) PMID: 21343903
Resistant Depression? Screen for Sleep Apnea
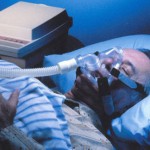 Depression is a common finding in overweight and obese patients trying to lose weight. So is obstructive sleep apnea.
Depression is a common finding in overweight and obese patients trying to lose weight. So is obstructive sleep apnea.
Unfortunately, the symptoms of sleep apnea can mirror those of major depressive disorder: tiredness and low energy levels, lack of interest and motivation to pursue your favourite activities, trouble with concentration, memory or decision making, and weight gain.
A paper by Mitsunari Habukawa and colleagues from the Kurume University School of Medicine, Fukuoka, Japan, just published online in Sleep Medicine, reminds us to screen overweight patients who do not respond adequately to antidepressant therapy for sleep apnea.
The authors describe 17 patients, who, despite pharmacotherapy for depression, continued having signs of major depressive disorder and were diagnosed with sleep apnea.
After two months of CPAP treatment for sleep apnea, their depression scores significantly improved.
Improvement in depression scores paralleled the reduction in sleepiness.
The results illustrate that patients with depression, who despite adequate pharmacotherapy continue having residual symptoms, should be screened for sleep apnea and treated if found positive.
An important corollary to this is that overweight and obese patients presenting with sleep apnea, should perhaps also be screened for signs of major depression.
Given the close association between excess weight, depression and sleep apnea, it is probably wise to regularly screen all patients presenting for obesity treatments for both conditions.
While simply treating depression and/or sleep apnea in people with excess weight is unlikely to result in significant weight loss, when present, both conditions can pose important barriers to successful weight management and must therefore be adequately addressed.
AMS
Edmonton, Alberta
p.s. Join my new Facebook page for more posts and links on obesity prevention and management
Habukawa M, Uchimura N, Kakuma T, Yamamoto K, Ogi K, Hiejima H, Tomimatsu K, & Matsuyama S (2010). Effect of CPAP treatment on residual depressive symptoms in patients with major depression and coexisting sleep apnea: Contribution of daytime sleepiness to residual depressive symptoms. Sleep medicine PMID: 20488748


