Pain Catastrophizing in Severe Obesity
Monday, December 1, 2008BEST HEALTH BLOG FINALIST: The second round of voting is on – please vote AGAIN for your favourite health blog by clicking here
 Pain is one of the most common and debilitating problems in patients challenged by severe obesity. Not just a consequence of mechanical complications of obesity (osteoarthritis, back pain, plantar fasciitis, fibromyalgia, etc.), pain is often a key barrier to physical activity and thus weight management. In fact, excess pain can promote psychological (e.g. depression, anxiety) and behavioural (e.g. binge eating) factors that may further promote weight gain.
Pain is one of the most common and debilitating problems in patients challenged by severe obesity. Not just a consequence of mechanical complications of obesity (osteoarthritis, back pain, plantar fasciitis, fibromyalgia, etc.), pain is often a key barrier to physical activity and thus weight management. In fact, excess pain can promote psychological (e.g. depression, anxiety) and behavioural (e.g. binge eating) factors that may further promote weight gain.
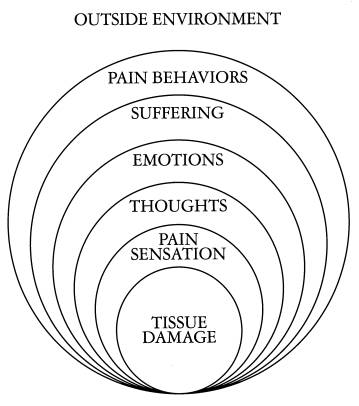
This issue is of even more importance in patients who display the now well-described phenomenon of pain catastrophizing, or the maladaptive responses to pain (tendency to focus on and magnify pain sensations with an intense sense of unbearable suffering and helplessness) that plays an extremely important role in how pain is perceived and processed. Pain catastrophizing now accounts for a substantial proportion of pain-related disability.
Studies in patients with fibromyalgia show that pain catastrophizing is associated with increased activity in brain areas related to anticipation of pain (medial frontal cortex, cerebellum), attention to pain (dorsal ACC, dorsolateral prefrontal cortex), emotional aspects of pain (claustrum, closely connected to amygdala) and motor control. Thus, catastrophizing influences pain perception through altering attention and anticipation, and heightening emotional responses to pain.
In another recent study by Tamara Somers and colleagues from Duke University, morbidly obese patients with osteoarthritis (OA) reported higher levels of pain catastrophizing than OA patients in the overweight and obese category. The severely obese patients who engaged in a high level of pain catastrophizing reported having much more intense and unpleasant pain, higher levels of binge eating, lower self-efficacy for controlling their eating and lower weight-related quality of life.
The relationship between pain catastrophizing and eating behaviour is of particular interest, as high-fat and high-sucrose foods have been shown to increase pain tolerance. Thus, binging on highly-palatable foods may be a compensatory response to emotional distress and pain. It is not difficult to see how patients can enter into a vicious cycle of pain, increased eating, weight gain, more pain, more eating, and so on.
In routine practice, pain catastrophizing can be easily and reliably assessed with questionnaires like this one, which can be scored like this.
Fortunately, pain catastrophizing is responsive to cognitive behavioural therapy, with clinically relevant improvements in upto 50% of individuals.
I would have little doubt that failure to recognize and address pain catastrophizing increases the likelihood of further weight gain and disability in patients with severe obesity.
AMS
Edmonton, Alberta


