Will Lifestyle Changes Improve Polycystic Ovary Syndrome?
Thursday, September 22, 2011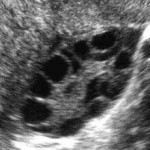 Polycystic ovary syndrome (PCOS) affects 4% to 18% of reproductive-aged women and is associated with significant reproductive, metabolic and psychological problems.
Polycystic ovary syndrome (PCOS) affects 4% to 18% of reproductive-aged women and is associated with significant reproductive, metabolic and psychological problems.
Obesity, not always, but often, an accompanying problem, worsens the presentation of PCOS. Current treatment guidelines for PCO, therefore, strongly recommend ‘weight management’ (both weight loss and the prevention of excess weight gain) through diet and exercise as an initial treatment strategy.
But how effective are these ‘lifestyle’ strategies and how consistent are the improvements?
This was the topic of a recent review by Lisa Moran and colleagues from Australia, published in the Cochrane Database of Systematic Reviews.
The authors identified six randomised controlled trial (including a total of 165 participants). Three studies compared physical activity to minimal dietary and behavioural advice or no advice; three compared combined dietary, exercise and behavioural interventions to minimal intervention.
Although these interventions resulted in modest weigh loss (~3.5 kg) and significantly reduced testosterone levels and associated male-pattern hair growth (hrisutism) as well as fasting insulin levels, there was no relevant effect on glucose or lipid levels or other cardiovascular risk factors.
Notably, none of these studies examined the impact of these interventions on quality of life, patient satisfaction or reproductive health (a common problem in PCOS). There was also no assessment of depression or anxiety, which have been reported to be commonly associated with PCOS.
Perhaps, as the authors point out, the most important result of this analysis is the apparent paucity of large studies that have addressed this issue – surprising enough, given that as many as 1 in 5 women of reproductive age may present with this problem and PCOS is a major cause of female infertility.
As the authors note:
“This review has identified that there are limited well-designed studies in lifestyle intervention in PCOS that are available to guide clinical practice.”
Given the impact of PCOS on reproductive health, it is most surprising that
“There are no existing RCT data identified in this review to assess whether lifestyle intervention improves reproductive outcomes including fertility, menstrual regularity or ovulation”
The overall conclusion is thus rather sobering:
“With the current evidence, it is not possible to comment on the relative effectiveness or sustainability of different durations or types of lifestyle interventions, or their relative success, in a weight loss or non-weight loss environment or with overweight or non-overweight participants……this indicates a considerable gap in the research literature.”
On other hand, this paucity of data should not be interpreted to show that interventions aimed at weight management do not impact on fertility or reproductive health in overweight and obese women with PCOS. Indeed, there is now accumulating anecdotal evidence that more significant weight loss (as can be achieved with bariatric surgery) may prove most beneficial in women with PCOS both in terms of reducing symptoms as well as in improving chances of conception.
Still, one wonders why a topic of such importance has not received more attention from researchers or funding agencies.
AMS
New York, NY
Moran LJ, Hutchison SK, Norman RJ, & Teede HJ (2011). Lifestyle changes in women with polycystic ovary syndrome. Cochrane database of systematic reviews (Online) (2) PMID: 21328294


