What Do Doctors Advise Patients About Losing Weight?
Thursday, December 2, 2010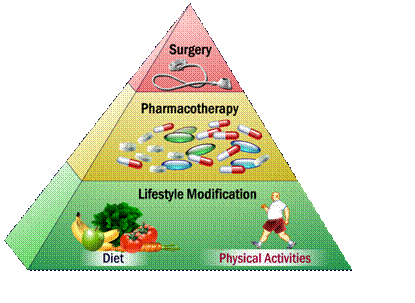 Obesity is a medical problem and obesity treatments should be initiated by trained health professionals.
Obesity is a medical problem and obesity treatments should be initiated by trained health professionals.
This solid piece of advice, of course assumes that trained health professionals actually know something about obesity treatment.
But is this assumption really valid?
We addressed this issue in a study just published in the Journal of Obesity, in which we surveyed 33 Canadian medical practices (36 physicians) regarding their obesity management recommendations in a total of 1788 consecutive overweight/obese adult patients.
It turns out that none of the evidence-based obesity management strategy was recommended by physicians in more than 50% of patients.
The most common recommendation/referral was for exercise (49% of cases) closely followed by dietary advice (46%).
Only 5% of patients meeting current eligibility criteria for bariatric surgery were referred for surgery.
Male patients were 30% less likely to be initiated or continued on anti-obesity pharmacotherapy than female patients.
Each BMI point was associated with a 2% increased chances of being prescribed an anti-obesity drug and private coverage increased the chances of a prescription by almost 80%.
Notably, one of the common reasons that weight management efforts were not initiated was “patient refusal”.
Interestingly, these results may actually be painting a much rosier picture than the reality: of the over 2000 doctors that were contacted to participate in this study, only 50 agreed to participate, but only 36 (from 27 primary care and 6 specialist practices) actually recruited any patients.
I am not sure, but it may be fair to assume that these participating practices actually had higher levels of interest and expertise in weight management and were therefore more likely to initiate weight management strategies than your average physician.
Obviously, we did not measure whether patients actually followed any of the advice or were in any way successful in managing their weight as a result of any advice they did receive.
Nevertheless, we think that this study clearly documents that before we can cheerfully advise all patients with excess weight to address this issue with their doctors, we better ensure that doctors (and other health professionals) can actually give appropriate advice that will indeed help patients better manage their weight.
If you have stories about appropriate or in-appropriate advice that you have received from a health professional, I’d love to hear about it.
AMS
Acapulco, Mexico
Padwal RS, Damjanovic S, Schulze KM, Lewanczuk RZ, Lau DC, & Sharma AM (2011). Canadian Physicians’ Use of Antiobesity Drugs and Their Referral Patterns to Weight Management Programs or Providers: The SOCCER Study. Journal of obesity (Online), 2011 PMID: 21113310


