Have Diabetes? Find a Surgeon!
Tuesday, March 24, 2009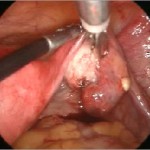 Type 2 diabetes mellitus is one of the most prevalent and expensive “lifestyle” diseases.
Type 2 diabetes mellitus is one of the most prevalent and expensive “lifestyle” diseases.
Here some numbers from the website of the Canadian Diabetes Association:
– The personal costs of diabetes may include a reduced quality of life and the increased likelihood of complications such as heart disease, stroke, kidney disease, blindness, amputation and erectile dysfunction.
– Approximately 80% of people with diabetes will die as a result of heart disease or stroke.
– Diabetes is a contributing factor in the deaths of approximately 41,500 Canadians each year.
– Life expectancy for people with type 2 diabetes may be shortened by 5 to 10 years.
– People with diabetes incur medical costs that are two to three times higher than those without diabetes. A person with diabetes can face direct costs for medication and supplies ranging from $1,000 to $15,000 a year.
– By 2010, it’s estimated that diabetes will cost the Canadian healthcare system $15.6 billion a year and that number will rise to $19.2 billion by 2020.
So imagine, what if a relatively straightforward laparoscopic operation, which takes 30-90 mins and lets you go home the very next day, cures this condition – in most cases forever?
This may very well be the case if we trust the results of a sytematic review by Henry Buchwald and colleagues from the University of Minnesota, published in this month’s edition of the American Journal of Medicine.
The paper reviews over 600 surgical studies in a total of over 135,000 patients, of whom around 22% had type 2 diabetes.
These are the results:
• Type 2 diabetes was resolved in 78% and resolved or improved in 87% of patients undergoing bariatric surgery.
• Both weight loss and diabetes resolution were greatest for patients undergoing biliopancreatic diversion/duodenal switch, followed by gastric bypass, and least for banding procedures.
• Clinical findings were substantiated by the laboratory parameters of serum insulin, HbA1c, and glucose.
• These findings were maintained for 2 years or more.
To be fair, the authors note several limitations of their study, the most important being the high attrition of patients available for follow-up, the diversity of reporting formats for diabetes outcomes, and the lack of information on specific subpopulations such as different ethnic groups. However, they also note that the the pattern of results for key outcomes in this meta-analysis are so consistent across studies, that they are hard to refute.
Although most of these studies did not study “hard outcomes”, we do know from the SOS Study (with a post-operative follow-up of 15 years and a follow-up rate of 99.9%) that surgery in patients with severe obesity can reduce total mortality by 30% and in a study from Utah, diabetes-related mortality was reduced by around 92%.
In contrast, recent studies of medical diabetes treatment failed to find any significant effect of better glucose control on mortality in patients with poorly-controlled diabetes (e.g. the Veterans Study)
I guess it is fair to ask – should perhaps bariatric surgery now be considered the “Gold Standard” for the treatment of type 2 diabetes, at least in patients with severe obesity? Should conservative diabetes treatments be reserved only for patients who do not meet surgical criteria? Tough questions that challenge much of current diabetes management – after all, why treat a condition for life, when it can be cured?
However, before running aboard with this idea, a word of caution – as I have blogged before – bariatric surgery involves far more than just surgery.
Nevertheless, in the light of these findings it does seem strange to me that a search for the term “bariatric surgery” on the website of the Canadian Diabetes Association comes up empty – I wonder why.
AMS
Edmonton, Alberta


