Obesity Classification: Time to Move Beyond BMI?
Tuesday, July 28, 2009While I am taking a brief break from clinics and other obligations (including daily blog posts), I will be reposting past articles, which I still believe to be relevant but may have escaped the attention of the 100s of new readers who have signed up in the past months.
The following was first posted on 30/03/08 (the Edmonton Obesity Staging System suggested in this original post, is now published in the International Journal of Obesity. Also note the foresight expressed in this post in light of Margaret Wente’s thought-provoking comment published in yesterday’s Globe and Mail – as this “classic” blog post demonstrates, we were well over a year ahead of Margaret in our thinking about what constitutes obesity and who needs treatment – good to see the mainstream media catch up!).
 Current definitions of obesity based on BMI and waist circumference (WC), while widely accepted, are hardly helpful in counseling individual patients. Readers of my blog are probably quite familiar with my views on this.
Current definitions of obesity based on BMI and waist circumference (WC), while widely accepted, are hardly helpful in counseling individual patients. Readers of my blog are probably quite familiar with my views on this.
As most clinicians will readily agree, when dealing with indiviual patients, both measures lack sensitivity and specificity with regard to identifying the presence or risk of obesity-related risk factors, comorbidities, psychopathology, global functioning or quality of life.
In fact recent epidemiological studies emphasize that good health including low morbidity and mortality is possible over a wide range of BMI. Thus, basing the decision on who to treat and who to leave well alone solely on measures of weight or size is neither sensible nor does justice to the complexity of the relationship between excess body fat and its impact on health and well-being. The well-established obesity-chronic disease paradox makes decisions on who to treat and who not to treat even more uncertain.
Telling healthy large people who have no apparent comorbidities, functional limitations or reduced well-being to lose weight may be counterproductive in that it can introduce and reinforce dissatisfaction with body image, foster frustrations and despair (given the poor long-term success of weight loss attempts) and lead to unhealthy behaviours focusing on weight loss (e.g. excessive exercise or dieting) rather than on healthy lifestyles (which are possible at almost any weight).
Thus, for practical purposes, it is important to move beyond defining who needs obesity treatment simply based on BMI and/or WC to a more clinically meaningful system.
Indeed, what we direly need is a classification of obesity that is clinically relevant in that it helps identify patients who have or are at high-risk of obesity-related complications and are most likely to benefit from treatment.
In this context, it may be worthwhile to look at the systems of classification and staging used for other disease states.
Oncologists have long used the TNM system to classify the extent of cancer spread. This system has established itself for the classification and staging of the vast majority of cancers not only because it is clinically meaningful in that it reflects extent of disease, indicates prognosis and allows evaluation of treatment response but also facilitates surveillance and research.
Psychiatrists and other mental health workers now routinely report on their patients using the five axes set out in the DSM-IV, each of which refers to a different domain of information that help the clinician plan treatment and predict outcome. The five axes are:
Axis I Clinical Disorders (all mental disorders except Personality Disorders and Mental Retardation)
Axis II Personality Disorders and Mental Retardation
Axis III General Medical Conditions (must be connected to a Mental Disorder)
Axis IV Psychosocial and Environmental Problems (for example limited social support network)
Axis V Global Assessment of Functioning (Psychological, social and job-related functions are evaluated on a continuum between mental health and extreme mental disorder)
While these systems are by no means simple or easy for the layman to understand, they are clinically useful and provide a standardized framework within which it is possible to describe the extent and impact of disease in a way that all clinicians, researchers and payors will understand.
Contrast these systems to the rather simplistic obesity classification, where knowing that a given person has Class II obesity (BMI 35-39.9) tells you virtually nothing about that person’s health or well being. Furthermore, it provides no meaningful guide in determining outcomes: e.g. someone who weighs 120 Kg with a BMI of 39 (Class 2 obesity) despite losing 10 Kg (8% weight loss) still has Class II obesity (BMI 36). This classification neither tells us what (if any) comorbities were actually present or whether (or not) these actually got better.
Now I am no expert on disease classification and realise the large amount of work and consensus meetings that go into developing these classification systems. But I am a clinician, who regularly sees patients and would be happy to see even the simplest form of staging that provides a meaningful framework.
The simplest classification I can think of would be to use a staging system similar to the following:
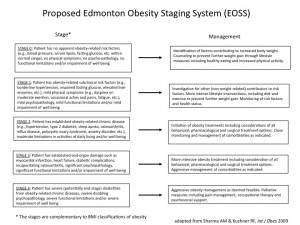
Stage 0: no apparent obesity-related risk factors (blood pressure, lipids, glucose, etc.), physical symptoms, psychopathology, functional limitations, or impairment of well-being
Stage 1: presence of obesity-related sub-clinical risk factors (elevated blood pressure, impaired fasting glucose, fatty liver, etc.), mild physical symptoms (dyspnea on moderate exertion, occasional aches and pains, etc.), mild psychopathology, mild functional limitations or mild impairment of well-being
Stage 2: presence of established obesity-related chronic disease like hypertension, type 2 diabetes, sleep apnea, osteoarthritis, reflux disease, polycystic ovary syndrome, depression, anxiety disorder, moderate limitations in activities of daily living and/or well being.
Stage 3: established end-organ damage like myocardial infarction, diabetic complications, severe osteoarthritis, significant psychopathology, significant functional limitations and impairment of well-being
Stage 4: severe (end-stage?) disabilities from obesity-related chronic disease, severe disabling psychopathology, severe functional limitations and severe impairment of well-being
Thus for e.g. a 24 year-old physically active female with a BMI of 32 with no measurable risk factors, functional limitations or self-esteem issues would have Class I, Stage 0 Obesity – benefits of treatment will be marginal or non-existent.
A 32 year-old male with BMI of 36 with hypertension and sleep apnea would have Class III, Stage 2 Obesity – definite indication for obesity treatment.
A 45 year-old female with BMI of 54 who is in a wheel chair because of severe gonarthritis with severe hypoventilaltion would have Class III, Stage 4 Obesity – will require aggressive obesity treatment unless deemed palliative.
But this may not be the only conceivable system. In fact, given the significant importance of psychopathology, personality traits, physical disease, psychosocial and enviromental factors as well as global functioning, I wonder if an approach similar to the axes in DSM-IV may be best. Of course, one could easily envision combinations of both systems, e.g. applying staging to Axis III disorders.
Obviously any such system would need careful definitions and perhaps a complex manual of diagnostics and classifications similar to DSM-IV – but at least we would have a way to assess, describe, treat, monitor and research obesity in a way that goes beyond the relatively meaningless anthropometry-based classification, which is nothing short of useless in clinical practice.
I can see why health authorities, professional organisations and even clinicians may be reluctant to devise a more complex classification of obesity – all I can say is that the present classification does not provide a meaningful framework in which to make clinical decisions or evaluate outcomes. There is certainly a need for a more complex system to guide practice (and research).
More often than not in clinical medicine – simple is simply wrong!
AMS
Edmonton, Alberta


