Human Hypothalamic Obesity
Friday, May 30, 2014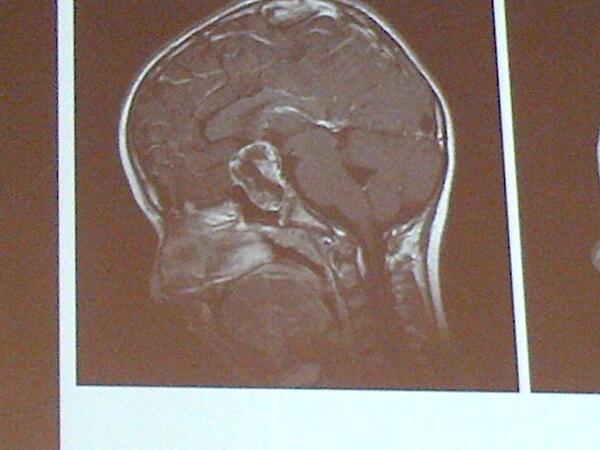 The second day of the 21st Europena Congress on Obesity in Sofia, Bulgaria, featured a plenary talk by Herman Mueller from Oldenburg, Germany, on the important lessons to be learnt from human forms of hypothalamic obesity.
The second day of the 21st Europena Congress on Obesity in Sofia, Bulgaria, featured a plenary talk by Herman Mueller from Oldenburg, Germany, on the important lessons to be learnt from human forms of hypothalamic obesity.
As readers are well aware, the hypothalamus is the key region in the brain for the regulation of energy balance – through its influences both on hunger and satiety as well as energy expenditure.
The best example of severe obesity caused by damage to the hypothalamus comes from patients with craniopharyngoma, a tumour that can partially or fully destroy the hypothalamus.
Indeed, craniopharyngoma are the most common form of sellar tumours.
Mueller presented his findings from a series of over 300 patients with craniopharyngoma recruited from Germany, Austria and Switzerland.
About half of the patients with craniopharyngoma develop severe obesity, whereas the other half maintain normal body weights.
It turns out that obesity may be one of the first signs of craniopharyngoma in children, sometimes preceding the diagnosis of this problem by over 24 months.
As expected, quality of life significantly reduces the quality of life in patients with hypothalamic obesity.
Interestingly, Mueller was unable to find marked differences in energy intake in patients with craniophyrongoma. Rather, accelerometric studies demonstrated reduced physical activity, increased daytime sleepiness and reduced night-time melatonin levels.
In fact, many of these patients had severe dysregulation of sleep cycles, which may in turn have contributed to weight gain.
Unfortunately, systematic study of this issue is complicated due to the fact that most centres see very few cases of this rather rare tumour.
Mueller emphasized that once hypothalamic obesity is established in patients with hypothalamic involvement, obesity becomes lifelong even if the tumour is fully surgically resected.
Thus, Mueller warns agains “radical” surgery in individuals without hypothalamic involvement to avoid damaging the hypothalamus.
With regard to treating severe obesity in patients with craniopharyngoma, Mueller notes that surgery may provide some relief. He described the case of a patient with severe hypothalamic obesity, who responded favourably to adjustable gastric banding, although not all patients experience sustainable weight loss. Nevertheless, the best results have been reported for gastric bypass and sleeve gastrectomy, although data on long-term follow-up remains scarce.
As for medical and behavioural therapy, Muellar was less optimistic – his extensive review of these studies showed rather modest and inconsistent results, often limited by side effects.
As for future interventions, one will need to await further developments in the pharmacological management of obesity and perhaps more radical treatments such as deep brain stimulation.
@DrSharma
Sofia, Bulgaria


