Fracture Non-Union in Obesity
Monday, June 9, 2008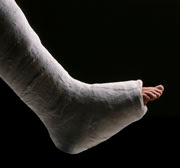 On Saturday (June 7), I presented at a session on How Obesity Affects Orthopaedic Care at the 2nd joint meeting of the American and Canadian Orthopaedic Associatons in Quebec City.
On Saturday (June 7), I presented at a session on How Obesity Affects Orthopaedic Care at the 2nd joint meeting of the American and Canadian Orthopaedic Associatons in Quebec City.
Despite being on the last day of this meeting, the session was surprisingly well attended, probably a reflection of the increasing awareness of issues around orthopaedic care for patients with severe obesity.
While I presented my usual take on how obesity is now a widespread chronic disease, I did take away some interesting aspects related to orthopaedic care of patients with obesity that I was unaware of.
For example, George Russell (Jackson, Mississippi) in his talk mentioned the issue that in severely obese patients immobilization of fractures with a plaster cast poses a significant problem due to the “cushioning” effect of the surrounding adipose tissue. This results in an increased risk of “non-union”, often requiring additional internal or external fixation to ensure healing.
Russell also presented an interesting view of how differences in body fat distribution pose specific problems in orthopedic surgery on hips and knees. Thus, in patients with the “large belly – thin limb” phenotype, the operation on the limbs is relatively easy, but, given the association between large bellies and cardiometabolic risk, these patients are at greater risk for poor wound healing and cardiovascular problems. In contrast, patients with “large limbs – thin bellies” present problems related to the size of the limbs resulting in a greater risk for bleeding and wound infections. Obviously, patients with “large bellies – large limbs” are at increased risk for both types of complications.
In a talk on orthopaedic problems in childhood obesity, Benjamin Alman (Sick Kids, Toronto) mentioned the issue of “relatively” (i.e. in relationship to their body mass) lower bone density in children with overweight and obesity, an issue that may increase the likelihood of traumatic fractures in these kids – again, something I had not previously thought much about.
Bassam Masri (UBC, Vancouver) confirmed that despite slightly greater risk and less functionality following joint replacement in patients with severe obesity, their satisfaction is no smaller than that or non-obese patients – clear indication that obese patients should not be denied surgery simply because of their size. But don’t expect to see spontaneous weight loss after surgery – in fact weight sometimes even goes up in overweight patients following surgery (I have blogged on this before).
I was particularly happy to note that all three surgeons called upon their colleagues to show compassion and deliver care with the same professional attitudes with which they approach their non-obese patients.
Overall, a most interesting session. I am delighted to see the orthopaedic surgeons taking this great interest in this (unfortunately) increasingly important issue.
AMS
Edmonton, Alberta


