Does Neuronal Scarring Determine the Body Weight Set Point?
Thursday, July 7, 2011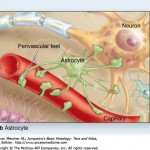 As regular readers are well aware, one of the major dilemmas in obesity management is the fact that virtually any attempt at weight loss is counteracted by complex mechanisms that aim to restore the body back to initial weight.
As regular readers are well aware, one of the major dilemmas in obesity management is the fact that virtually any attempt at weight loss is counteracted by complex mechanisms that aim to restore the body back to initial weight.
So far, no one has discovered a way to reverse or ‘reset’ this mechanism so that, once weight is lost, the body ‘relaxes’ and ‘accepts’ that new, lower body weight again.
This is why, no matter what program, diet, exercise, medication or surgery you chose for weight loss, when you stop the program, diet, exercise, medication, or reverse the surgery, your weight comes back – there are almost no exceptions to this rule.
So how does weight gain lead to this apparently ‘permanent’ resetting of the body-weight ‘set point’?
A recent paper by Tamas Horvath (Yale) together with colleagues from the US, Europe and Australia, published in the Proceedings of the US National Academy of Science, suggests that ‘micro-scarring’ of neurons that regulate hunger and satiety in the hypothalamus (the key homeostatic centre of eating behaviour) may play an important role in this process.
The researchers first studied the microscopic organisation of synapses (nerve-nerve contacts) in the anorexigenic (hunger-suppressing) proopiomelanocortin (POMC)-expressing nerve cells of the arcuate nucleus in lean rats that were vulnerable or resistant to diet-induced obesity.
There was a clear quantitative and qualitative difference in the synaptic organisaton of POMC cells between these animals, with a significantly greater number of inhibitory inputs in the POMC neurons in weight-gain susceptible rats compared with resistant rats.
Then, when given similar high-fat diets, the POMC cells of weight-gain resistant rats formed more connections whereas the susceptible animals actually lost synapses.
Importantly, this loss of synapses was associated with a process called ‘reactive astrogliosis’ or ‘glial-scarring’ whereby, in an ‘inflammatory’ response, astrocytes ensheath the POMC neurons, thereby making them ‘permanently’ inaccessible to new synapses (hence the use of the term ‘scarring’).
In addition, this formation of glial ‘scar’ tissue, also made the POMC cells less accessible to blood vessels (i.e. increased the blood-brain barrier).
As all ‘scarring’ processes in the body, these micro-scars are in essence, irreversible, or in other words, permanent.
Thus, these findings clearly show how increased caloric intake in ‘obesity-prone’ rats (and humans?) can lead to permanent changes in the cell-architecture of the arcuate nucleus thereby essentially ‘locking in’ the new ‘set point’.
Obviously, no diet, exercise, medication or surgery will undo the ‘scarring’ in these key centres of the brain (in the same way that no diet, exercise, medication or surgery will undo a scar in your skin or anywhere else in your body) – which is perhaps why none of these interventions will ever lead to ‘permanent’ weight loss unless they are continued in the long-term.
Although this may sound very disappointing and discouraging, these findings may eventually lead to new treatment strategies that can help prevent the ‘resetting’ by reducing or preventing the ‘inflammation’ that promotes the formation of astrogliosis with weight gain.
Perhaps, as in rats, those ‘rare’ people who appear to be (genetically?) weight-gain resistant or have less problem losing weight and keeping it off, can do so simply because they have more synapses in their POMC neurons to start with, easily grow more synapses when exposed to excess calories, or simply do not develop the ‘micro-scarring’ in their brains with weight gain.
Of course, scar or no scar, none of this means that treatments don’t work – of course they do, as long as the treatments continue.
So, the runners, who lost weight running, will have to keep running, the dieters, who lost weight dieting, will have to keep dieting, the patients who had bariatric surgery, can expect weight regain if they ever reverse the surgery – when the ‘treatment’ stops, the weight comes back!
As I have said before, the first measure of success in obesity management is stopping the gain – less weight gain – less scarring?
Successful obesity management is prevention!
AMS
Edmonton, Alberta
Horvath TL, Sarman B, García-Cáceres C, Enriori PJ, Sotonyi P, Shanabrough M, Borok E, Argente J, Chowen JA, Perez-Tilve D, Pfluger PT, Brönneke HS, Levin BE, Diano S, Cowley MA, & Tschöp MH (2010). Synaptic input organization of the melanocortin system predicts diet-induced hypothalamic reactive gliosis and obesity. Proceedings of the National Academy of Sciences of the United States of America, 107 (33), 14875-80 PMID: 20679202


