Hindsight: Regulation of 11β-HSD Genes in Human Adipose Tissue – Influence of Central Obesity and Weight Loss
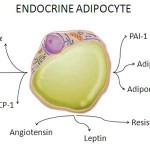 11β-hydroxysteroid dehydrogenase (11β-HSD) belong to a class of hormones that play key role in the regulation of gluco- and mineralocorticoids in a wide range of tissues.
11β-hydroxysteroid dehydrogenase (11β-HSD) belong to a class of hormones that play key role in the regulation of gluco- and mineralocorticoids in a wide range of tissues.
11βHSD exists in two forms (encoded in different genes):
Type 1 (11β-HSD1), highly expressed in key metabolic tissues including liver, adipose tissue, and the central nervous system, where it reduces inactive cortisone to the active ‘stress’ hormone cortisol that activates glucocorticoid receptors, and
Type 2 (11β-HSD2), highly expressed in aldosterone-selective tissues, including colon, salivary glands, and placenta, where it oxidizes active cortisol to inactive cortisone and prevents inadvertent activation of the mineralocorticoid receptor.
In a study we published back in 2004 in OBESITY RESEARCH, we examined the expression of both forms of the 11β-HSD gene in subcutaneous adipose tissue biopsies of 70 postmenopausal women. We also examined the influence of weight reduction and in vitro effects of several modulators of adipocyte gene expression on 11β-HSD genes in primary cultured human adipocytes.
As described previously, the 11β-HSD1 gene was highly expressed in human adipose tissue (whereas 11β-HSD2 was detectable at lower levels).
Adipose tissue 11β-HSD1 gene expression was increased two-fold in obese women and was positively correlated with waist circumference and homeostasis model assessment (HOMA) index of insulin resistance.
In contrast, 11β-HSD2 gene expression was reduced by half in obese women.
Interestingly, weight loss did not change gene expression levels of either 11β-HSD gene.
Cortisol increased 11β-HSD1 gene expression in isolated human adipocytes in vitro, whereas estradiol, triiodothyronine, angiotensin II, and pioglitazone had no influence.
From these findings we concluded that that increased expression of the 11β-HSD1 gene is associated with metabolic abnormalities in obese women and that increased expression of this gene may contribute to the previously reported increased local conversion of cortisone to cortisol in adipose tissue of obese individuals.
Thus, increased expression of 11β-HSD1 may well contribute to the development of insulin resistance and the metabolic syndrome commonly associated with central obesity.
Interestingly enough several pharmaceutical companies (including Merck and Boehringer Ingelheim) are currently developing selective inhibitors of 11β-HSD1 as agents to treat obesity and the metabolic syndrome.
According to Google Scholar, this paper has been cited 144 times.
AMS
Edmonton, Alberta
Obesity and Mental Health, Day 3: First Do No Harm
 The 3rd and final day of the Hot Topics Conference on Obesity and Mental Health focussed on the potential obesogenic side effects of medications commonly used to manage mental health disorders.
The 3rd and final day of the Hot Topics Conference on Obesity and Mental Health focussed on the potential obesogenic side effects of medications commonly used to manage mental health disorders.
As pointed out by Rohan Ganguli (Toronto), persons with schizophrenia, bipolar disorder, and other psychotic illnesses, have rates of obesity 2-3 times that of the general population. They also have 2-3 times the rates of diabetes, heart disease, and premature mortality, when compared to the general population. The increased prevalence of these chronic conditions are due to multiple factors, but it has become clear that certain antipsychotics, particularly some of the newer antipsychotics, mood stabilizers, and antidepressants, contribute to the increased risk of obesity. His presentation provided a succinct overview of the evidence from controlled clinical trials regarding the risk of weight gain for different psychotropic medications. He also proposed prescribing strategies, which would minimize the exposure to these risks. This presentation was nicely complemented by Tony Cohn’s (Toronto) talk on the importance of metabolic monitoring for adults prescribed antipsychotic medications
This problem, unfortunately, is also relevant in the treatment of mental health disorders in kids. In her presentation on the Canadian Guidelines on Monitoring and Management of Metabolic Side Effects of Second Generation Antipsychotic Medications in Children, Tamara Pringsheim (Calgary) discussed the considerable evidence that second generation antipsychotic medications are associated with metabolic side effects in children, including weight gain, increased waist circumference and body mass index, as well as elevations in cholesterol, triglycerides, glucose and insulin levels. These metabolic complications can have long-term adverse effects on cardiovascular health. With the more widespread use of antipsychotic medications in children, there is a need for formal guidelines on how to monitor children for adverse effects of these medications.
The Canadian Alliance for monitoring Safety and Effectiveness of Antipsychotic medications in Children (CAmESA) guidelines seek to provide health care providers with evidence based recommendations on what, when and how to monitor children started on an antipsychotic medication for metabolic and extrapyramidal side effects. Companion guidelines have also been created which provide evidence based recommendations on the management of metabolic and extrapyramidal side effects if they are detected over the course of monitoring drug safety in kids.
The considerable problem of obesity and mental health in the Aboriginal population was discussed by Piotr Wilk from London, Ontario.
The issue of first doing no harm, especially in public messaging about obesity, was addressed by Gail McVey (Toronto). She noted that in our quest to prevent childhood obesity it is imperative that we avoid the costly mistake of triggering the competing public health issues of disordered eating, weight-related bullying and associated depression, anxiety and social exclusion. Professionals need to capitalize on opportunities for greater integration by agreeing to adopt a common set of child and youth health indicators and to settle on an integrated approach to prevention across the broad spectrum of weight-related problems. nowhere is this common vision more important than in the messaging delivered to children and youth about healthy weights.
Similarly, as pointed out by Annick Buchholz (Ottawa), dialogue between researchers and clinicians from the fields of eating disorders and obesity can take advantage of evidenced-based frameworks and key treatment approaches from the field of eating disorders and discuss its applications to working with individuals and families struggling with weight management issues. Treatment approaches such as externalizing the problem, promoting positive body image, de-emphasizing weight as a goal in treatment, understanding ambivalence, and working closely with families in treatment are all important approaches to this problem.
On a slightly different note, Peter Selby (Toronto) discussed the potential learning from tobacco prevention. Given that behaviours are determined by the net effects of the current and embodied opportunities and constraints in global, macro, mezzo, and micro environments interacting with biological and psychological abilities of the individual, disorders of consumption such as smoking and excess eating share common pathways and are modifiable through policy and clinical interventions. High reach interventions focussing on policy and legislation are likely to have a bigger impact on health than only a high risk approach to obesity. However, mitigation of unintended consequences of such measures must also be considered in order to prevent disparity in the disease burden.
Thus, after 3 days of intense presentations and discussions, I believe that the participants left with a much better appreciation and understanding of the links and commonalities between obesity and mental health.
I, for one, certainly felt very pleased to see many of the concerns and approaches discussed by the participants at this conference, nicely reflected in the 5As of Obesity Management.
Presentations from this conference are available for download here.
AMS
Edmonton, Alberta
FDA approves lorcaserin, first weight-loss drug since 1999
As a means of boosting weight loss results without surgery, lorcaserin “addresses one of the greatest therapeutic gaps we have in medicine,” said Dr. Arya M. Sharma, an obesity expert and professor of medicine at the University of Alberta in Canada.
Obesity and Mental Health: Day 2 – ‘Stressed’ is ‘Desserts’ Spelled Backwards
 On the day 2 of the Hot Topics Conference on Obesity and Mental Health, Zul Merali and Alfonso Abizaid from the University of Ottawa (working as a tag team) discussed the importance of stress as a driver of overeating. They described a a fascinating possible role of ghrelin as an important mediator that allow organisms to meet the energetic challenges of stress (which generally does require the organism to spend more energy).
On the day 2 of the Hot Topics Conference on Obesity and Mental Health, Zul Merali and Alfonso Abizaid from the University of Ottawa (working as a tag team) discussed the importance of stress as a driver of overeating. They described a a fascinating possible role of ghrelin as an important mediator that allow organisms to meet the energetic challenges of stress (which generally does require the organism to spend more energy).
Thus, ghrelin, a hormone that increases hunger and adiposity, is not only secreted when energy stores are low, but also in response to stressors. Chronic stress leads to chronically elevated levels of this hormone in tandem with increases in appetite and weight gain. These effects are prevented by pharmacological blockade of ghrelin receptors and are absent in mice with targeted mutations to the ghrelin receptor. These ghrelin receptor deficient mice, however, are more susceptible to stress-induced depressive like behaviors. Thus, although ghrelin response to stress may induce hunger and overeating, organisms that do not (or cannot) elicit this response may be more likely to develop depression like symptoms in the face of stress.
Shelly Russell-Mayhew (U Calgary) spoke on body dissatisfaction and weight and shape concern, two components of body image that have particular relevance for obesity and mental health. Body dissatisfaction is a consistent correlate of obesity in youth. While this may well be seen as a negative consequence of obesity, it is also important to recognise that body dissatisfaction often leads to dieting/unhealthy weight control practices. In youth, dietary restraint, or the vigilant restriction of caloric intake, in turn is associated with obesity and is predictive of future weight gain. Overweight children are even more concerned about weight than their normal-weight counterparts and normal-weight children with high weight and shape concern report higher body dissatisfaction and depressive symptoms. A focus on the promotion of healthy body image for children of all weight statuses could reduce the impact of multiple negative psychological outcomes. This is particularly important because of evidence that perceived weight rather than actual weight is more predictive of psychological distress and body satisfaction predicts less weight gain over time.
Ronnie Kolotkin, the developer of the Impact of Weight on Quality of Life questionnaire (IWQoL-Lite), a widely used questionnaire that assesses quality of life in obese persons and has been translated into over 60 languages, emphasized that assessing quality of life in obesity may be just as important as, or even more important than, measuring body weight or body mass index.
Other presentations on Day 2 included talks by Nick Finer, UK, on the potential role of gut hormones for treating obesity, Teodor Grantcharov (Toronto) on surgical treatments for obesity, Valerie Taylor (Toronto) on pregnancy and the post-partum period as windows for obesity and mental illness, Michael Vallis (Halifax) on the use of motivational interviewing, Anthony Fabricatore (Pennsylvania) on predictor of weight loss response in bariatric surgery, Rohan Ganguli (Toronto) on the potential and limitations of behavioural interventions for weight loss in psychiatric patients, Fannie Dagenais (Montreal) on efforts to change social standards on weight and body image, and Mary Forhan (Hamilton) on the factors that contribute to engagement in every day life of people living with severe obesity.
Overall, a most interesting a day, that ended with a plenary engagement of the participants in drafting the Toronto Charter on Obesity and Mental Health, which will be officially released in the coming days.
AMS
Toronto, Ontario
Mental Health and Obesity: Day 1
 Yesterday, in my talk, at the sold-out standing-room-only Hot Topics Conference on Obesity and Mental Health here in Toronto, I pointed out that individuals presenting with obesity often also present with mental health problems ranging from mood to attention deficit or addiction disorders. In addition, they often have eating disorders, poor self-esteem and body image and other challenges that affect their eating and activity behaviours. Thus, routine assessment and management of mental health problems should be part of obesity management practice. I also presented a brief overview of the Canadian Obesity Network’s 5As of Obesity Management.
Yesterday, in my talk, at the sold-out standing-room-only Hot Topics Conference on Obesity and Mental Health here in Toronto, I pointed out that individuals presenting with obesity often also present with mental health problems ranging from mood to attention deficit or addiction disorders. In addition, they often have eating disorders, poor self-esteem and body image and other challenges that affect their eating and activity behaviours. Thus, routine assessment and management of mental health problems should be part of obesity management practice. I also presented a brief overview of the Canadian Obesity Network’s 5As of Obesity Management.
Roger McIntyre (U of Toronto) presented data showing that individuals with bipolar disorder (BD) are differentially affected by overweight, obesity, and abdominal obesity. The hazards posed by excess weight in the Bd population on illness presentation, clinical course, and outcome have underscored the need to prioritize the prevention and treatment of overweight in this vulnerable population. Emerging evidence indicates that overweight/obesity may adversely affect neurocognitive performance in individuals with BD and may also be inversely associated with other addictive behaviours (e.g. substance use disorders). The contribution of distal adversity (e.g. childhood physical, sexual abuse) as a vulnerability factor for obesity has not been sufficiently reported or characterized. He also presented results from two recently completed studies documenting the effect of obesity on white matter integrity and as well the (positive) impact of bariatric surgery on the course of BD.
Randy Sansone (Wright State University, Dayton, Ohio) spoke on the role of borderline personality disorder (an Axis II dysfunction that is characterized by inherent difficulties with self-regulation), which may coexist in syndromes that are characterized by self-regulation difficulties. Perhaps, not surprisingly, studies in various eating disorder samples clearly suggest that restrictive personality styles are associated with restrictive eating pathology whereas impulsive personality styles are associated with impulsive eating pathology. Present data indicate that slightly over one-quarter of obese individuals may suffer from varying degrees of borderline personality disorder. Obviously, this has a number of clinical implications, particularly in terms of assessment, treatment strategies, and outcome.
Allan Kaplan (U of Toronto) focussed in his presentation on the fascinating phenomenology and etiology of the two commonest recognized eating disorders, bulimia nervosa and binge eating disorder, and their relationship to obesity. Needless to say, all health professionals dealing with obesity have to be well qualified to recognise and address these eating disorders in their patients and, if necessary, refer patients to the appropriate provider for treatment.
Other talks on this first day of the meeting included presentations by York University’s Caroline Davis on ADHD, Rudy Berthoud from the Pennington Biomedical Research Centre, Baton Rouge, LA, on neural Integration of metabolic, cognitive, and emotional signals in the control of ingestive behaviour, and Alain Dagher from McGill University on the neurobiology of appetite and a discussion of whether or not hugner and appetite should be seen as addictions.
Overall, a most interesting first day complemented by great discussions and exciting poster presentations.
Today’s presentations certainly promise to be as interesting.
AMS
Toronto, Ontario


