Activity of Friends and After-School Activity in Kids
 Here is a piece of research, where one could have probably guessed the results – if your close friends are active after school, so are you!
Here is a piece of research, where one could have probably guessed the results – if your close friends are active after school, so are you!
Thus, according to a paper by Sabina Gesell and colleagues from Vanderbilt University School of Medicine, Nashville, Tennessee, published in PEDIATRICS, a social network analysis in 83 public school students participating in 2 structured aftercare programs found that while children did not form or dissolve friendships based on physical activity levels, existing friendships heavily influenced their level of physical activity.
In fact, the strongest predictor of the amount of time children spent in moderate-to-vigorous activity in the afterschool hours was the activity level of their immediate friends.
It appears that children consistently made adjustments to their activity levels of 10% or more to emulate the activity levels of their peers.
This effect was largely independent of age, sex or obesity status.
“Children did not select friends based on activity level. Active children did not have more (or fewer) friends than nonactive children, nor were they more (or less) likely to be chosen as friends. Friendships were more likely to be based on homophily in age, school, gender, and race.”
Thus, the authors conclude that friendship ties play a critical role in setting physical activity patterns in children as young as 5 to 12 years.
From an intervention perspective (especially in light of yesterday’s post on the Active Health Kids Report Card), it is very likely that children’s activity levels can be increased, decreased, or stabilized depending on the activity level of their immediate social network.
“Given the opportunity to either change activity level to match that of their friends, or keep activity level constant, children were 6 times more likely to adjust their activity level. Children became either more active or more sedentary as they emulated the behaviors of those in their immediate network.”
Thus, if you could just get a couple of kids within a network to be more active after school, their best friends will likely follow.
Or, as the authors suggest:
“An intervention that embeds inactive children with active peers may improve activity levels across the entire social network. Such a strategy could startwith a group of very active children and implement a “rolling enrollment” of inactive children into the group. It would be critical that these inactive children form friendships with the active children for them to become more active themselves.”
Unfortunately, getting kids to become friends is no easy task, so this may be easier said than done.
AMS
Edmonton, Alberta
![]() Gesell SB, Tesdahl E, & Ruchman E (2012). The Distribution of Physical Activity in an After-school Friendship Network. Pediatrics PMID: 22641755
Gesell SB, Tesdahl E, & Ruchman E (2012). The Distribution of Physical Activity in an After-school Friendship Network. Pediatrics PMID: 22641755
.
.
Active Healthy Kids Report Card Calls To End ‘Hyperparenting’?
 Yesterday, Active Healthy Kids Canada released its 2012 Report Card on Physical Activity.
Yesterday, Active Healthy Kids Canada released its 2012 Report Card on Physical Activity.
It probably comes as no surprise to anyone that once again the overall grade is ‘F’.
As noted before, inactivity is not a problem specific to obese kids, most Canadians kids (lean or overweight) are simply not active enough – period!
Among the 24 grades assigned in the Report Card, key grades include:
• “F” for Active Play & Leisure
• “F” for Physical Activity Levels
• “F” for Screen-Based Sedentary Behaviours
• “D+” for Active Transportation
• “D+” for Family Physical Activity
• “F“ for Federal Government Investments
• “C-” for Provincial/Territorial Government Investments
One of the few As in the report card (an A- to be precise) was given for the proximity & availability of facilities, programs, parks & playgrounds indicator which, (unchanged from last year) shows that the large majority of Canadian children and youth live in communities where the built environment has characteristics that are conducive to physical activity and opportunities for physical activity are nearby and available. So I am really not exactly sure what more communities can be expected to do here.
Also, notably, one of the few B grades in the report was given to sport & physical activity opportunities at school, reflecting the fact that over half of schools in Canada offer a number of intramural and intervarsity sports, and the majority of parents report that schools offer other physical activity or sport programs outside of regular PE classes. While, as noted before, this may not always be conducive to promoting more physical activity in the less-competetive ‘non-natural-born-athlete’-type kid, it is also not clear exactly how much more schools could or should be doing to get kids moving (perhaps less is more?).
I, for one, tend to believe that the key problem is exactly what is highlighted in the accompanying press release:
“Barriers, including screen time and parental safety concerns, force children and youth into highly-controlled environments, where they have little opportunity for active play. Fifty-eight per cent of Canadian parents say they are very concerned about keeping their children safe and feel they have to be over-protective of them. Safety concerns, whether or not they are founded, such as crime, traffic, neighbourhood danger, outdoor darkness and lack of supervision, discourage parents from letting their children and youth play outdoors.”
As Mark Tremblay, Chief Scientific Officer, Active Healthy Kids Canada, points out:
“Kids of all ages should have regular opportunities for active play, where they can let loose, explore, run, climb, crawl and play in parks with friends, like their parents once did.”
Unfortunately, the solution suggested by Active Kids, namely,
“To address safety concerns, parents and caregivers can take turns supervising and playing with children outdoors or encourage kids to play with a buddy.”
is not exactly helpful, when parents and caregivers themselves are sedentary and exhausted and lack the time to spend with their kids.
It is no surprise that double income households (the rule rather than the exception), while great for the economy, also means one person less at home to actually do the supervising. I am, frankly, not at all surprised when most parents, after a busy work day and a long commute, barely managing to stop to pickup up the dinner pizza on their way home, realising that all of the regular household chores still await them, often simply lack the energy to also spend a couple of extra hours every day ‘supervising’ their kids on the playground.
Perhaps it is simply time to cut those kids loose – yes, there will be trouble, knees will be scratched, arms will be broken, clothes will be torn, tears will be shed – but so what? It never harmed us – it sure won’t harm our kids.
As Tremblay points out,
“Active play is fun, but it is also shown to improve a child’s motor function, creativity, decision-making, problem-solving and social skills.”
Perhaps our very effort to save our kids from harm is exactly what is harming them the most?
Please, let your poor kids eat those germs!
AMS
Edmonton, Alberta
Is When You Eat as Important as What You Eat?
 Recently, a number of studies have looked at the impact of sleep deprivation, disruption of the sleep-wake cycle, and shifts in circadian rhythm on feeding behaviour and propensity to gain weight (facit: they are all bad!).
Recently, a number of studies have looked at the impact of sleep deprivation, disruption of the sleep-wake cycle, and shifts in circadian rhythm on feeding behaviour and propensity to gain weight (facit: they are all bad!).
This is probably because, a complex biological clock machinery translates time information into physiologically meaningful signals by the regulation of hundreds of clock-controlled output genes (CCGs) that control virtually all aspects of cellular function.
From an evolutionary perspective this makes a lot of sense as certainly bodily functions make sense in the wake state but are not required whilst asleep, while other functions are best managed during night time, when the organism should normally be asleep.
Now there is work emerging that some of these metabolic changes can be reset or readjusted by the timing of food intake.
One such study is the one by Barclay and colleagues form the Max Planck Institute of Biophysical Chemistry, Göttingen, Germany, just published in PLoS One.
Based on the emerging body of evidence that shiftwork is associated with adverse metabolic pathophysiology potentially involving direct physiological effects of nocturnal light exposure, or indirect consequences of perturbed endogenous circadian clocks, the researchers used a two-week paradigm in mice to model the early molecular and physiological effects of shiftwork.
During this time, animals were kept awake during their regular sleeping hours and were provided foods either during their normal waking hours or their ‘night shifts’.
According to their findings although the two weeks of timed sleep restriction had rather modest effects on diurnal activity patterns, feeding behavior, and clock gene regulation in the circadian pacemaker of the suprachiasmatic nucleus, microarray analyses revealed considerable global disruption of diurnal liver transcriptome rhythms, enriched for pathways involved in glucose and lipid metabolism.
Much of these metabolic abnormalities were prevented by restricting food intake during the ‘night shift’ and providing access to foods only during the beginning of ‘normal’ waking hours.
Thus, the authors conclude that,
“Although altered food timing itself is not sufficient to provoke these effects, stabilizing peripheral clocks by timed food access can restore molecular rhythms and metabolic function under sleep restriction conditions.”
They thus further speculate that,
“…strengthening the peripheral circadian system by minimizing food intake during night shifts may counteract the adverse physiological consequences frequently observed in human shift workers”.
Obviously, these findings need to be replicated in human shift worker. I, for one, can certainly attest to the fact that the notion of not eating during long night shifts may well prove a challenge for most people (particularly during the wee hours of the morning when cravings for sweets and junk food seem the hardest to resist). On the other hand, I do recall that the nights, where I had a normal dinner prior to starting a shift were less problematic than taking a midnight or early morning break for a meal.
I would certainly love to hear from readers about their experiences with eating and weight gain during shift work and how they deal with shifting sleep wake cycles.
AMS
Red Deer, Alberta
![]() Barclay JL, Husse J, Bode B, Naujokat N, Meyer-Kovac J, Schmid SM, Lehnert H, & Oster H (2012). Circadian desynchrony promotes metabolic disruption in a mouse model of shiftwork. PloS one, 7 (5) PMID: 22629359
Barclay JL, Husse J, Bode B, Naujokat N, Meyer-Kovac J, Schmid SM, Lehnert H, & Oster H (2012). Circadian desynchrony promotes metabolic disruption in a mouse model of shiftwork. PloS one, 7 (5) PMID: 22629359
.
The Significance of Excess Fat in Non-Obese Individuals
 Regular readers will be well aware that excess body weight, or even excess body fat, is not always associated with health risks. In contrast, it is now increasingly recognised that excess body fat (especially visceral fat), may constitute an important health risk even in individuals well below the conventional BMI cutoffs for obesity.
Regular readers will be well aware that excess body weight, or even excess body fat, is not always associated with health risks. In contrast, it is now increasingly recognised that excess body fat (especially visceral fat), may constitute an important health risk even in individuals well below the conventional BMI cutoffs for obesity.
Readers wishing to learn more about the nature of these so-called ‘lean-but-fat’ (LBF), ‘thin-on-the-outside fat-on-the-inside’ (TOFI) or ‘metabolically obese but normal-weight’ (MONW) individuals are directed to an excellent review article by Louise Thomas and colleagues from Imperial College London, UK published in Nutrition Research Reviews.
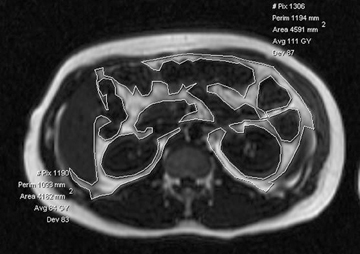
As the article stems from the Metabolic and Molecular Imaging Group at Hammersmith Hospital, it contains a nice selection of MRI images depicting these different phenotypes.
As the authors note, lean individuals with the typical metabolic phenotype more commonly associated with obesity
“…have been shown to have reduced insulin sensitivity, increased abdominal adiposity, a more atherogenic lipid profile, and raised blood pressure, accompanied by physical inactivity and a low VO2max. The combination of these factors is thought to predispose ‘metabolically obese but normal-weight’ subjects to an increased risk of type 2 diabetes and CVD.
This phenotype has been further refined using MRI to show disproportionate deposition of visceral adipose tissue, with many lean subjects having more visceral adipose tissue than overweight or obese subjects. This TOFI (thin-on-the-outside fat-on-the-inside) sub-phenotype has been observed in both male and female subjects, and increases an individual’s risk of metabolic disease.”
As they further note,
“Identifying subjects classified as TOFI may be important, since they may be at increased risk of metabolic disease compared with more obese subjects with less visceral fat. Incidence of ‘metabolically-obese but normal-weight’ has been reported to be between 13 and 18 %, which is similar to the incidence of TOFI (12 % women, 14 % men).”
Overall, these finding are in line with our own observations that EOSS Stage 0 overweight and obese individuals, which comprise about 5-10% of the obese population, do not appear to have an increased risk for cardiovascular mortality, while over 50% of individuals in the BMI 25-30 range can meet the criteria for EOSS Stage 2 and 3 and with the same risk of cardiovascular complications as their obese counterparts.
Unfortunately, despite the lower total amount of body fat, it appears that sustainably reducing body fatness is no less difficult in lean folks with excess body fat than in obese individuals. As I recently heard some one point out in a presentation (I forget who), losing and keeping off 5% of your body weight is as difficult (or easy) whether you are a 100 lbs or 300 lbs.
AMS
Edmonton, Alberta
![]() Thomas EL, Frost G, Taylor-Robinson SD, & Bell JD (2012). Excess body fat in obese and normal-weight subjects. Nutrition research reviews, 1-12 PMID: 22625426
Thomas EL, Frost G, Taylor-Robinson SD, & Bell JD (2012). Excess body fat in obese and normal-weight subjects. Nutrition research reviews, 1-12 PMID: 22625426
.
Weekend Roundup, May 25, 2012
 As not everyone may have a chance during the week to read every post, here’s a roundup of last week’s posts:
As not everyone may have a chance during the week to read every post, here’s a roundup of last week’s posts:
- The 5As of Obesity Management™
- Core Principles of Obesity Management
- Metabolically ‘Healthy’ Obesity is Not Associated With Higher Mortality Risk
- Calorie Restricted Diet Decreases Breast Cancer Biomarkers in Post-Menopausal Women
- Register Now: Workshop on Obesity and Mental Health, Toronto, June 26-28
Have a great Sunday! (or what is left of it)
AMS
Edmonton, Alberta


